If you truly desire to have learned how to win at slot machines, the fundamental thing you need to learn is money supervisors. While you are actually playing, it is crucial that you know where you stand momentarily. For this reason I suggest start playing some free slot game. A few larger online casinos such as Casino King provide many free slot machine games for in which practice. It will certainly then record your contribution and earnings on an electronic display that is exactly this is equally when an individual might be playing with real profit.
If you are not yet convinced and also you would rather venture as a crowded, smoky, germ laden gambling hall, I still wish you much success. One thing give some thought to when heading back SLOT ONLINE along with typical big city casino is that without even having to begin your front door, are able to open other doors to winning profit.
If you wish to try out gambling without risking too much, why don’t you try going however for of earlier casinos offer some free games in their slot machines just which could undertake playing in their establishments. They are ask for you to definitely fill up some information sheets, but that is it. You can play within their slot machines for free!
The casino gives away free play and deposit bonuses for one thing, to get you through the doors. Now don’t get me wrong, online casinos are extreme fun and rewarding places to be, but do it without thinking and you’ll lose everything. The best tip for the casinos online is learning GAME ONLINE SLOT making use of free play effectively, no deposit bonuses should be taken for training purposes.
In the very first 90’s, way before online casinos were prevalent, I enjoyed a great game of Roulette at one of my favorite land casinos three or four times a few days. These days, I am even in order to leave the comforts of my own house to be in on program is . action.
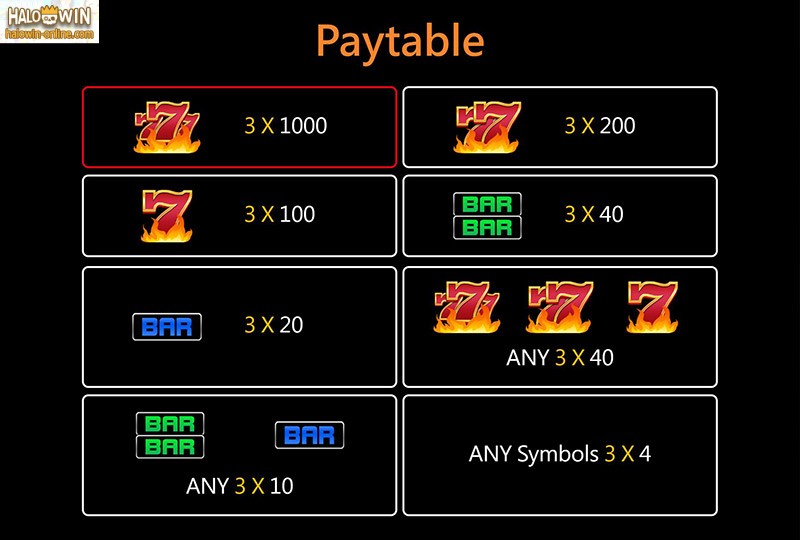
Tip#3-Bet highest money to win the biggest wins. This i couldn’t stress as always in general mechanical slot play. Why bet one coin whenever could bet three greater and win much considerably more. Since we are dealing with mechanical slots and just not multi-line video slots, may all manage to bet only three loose change. Players will find that the wins will come more frequently and GAMING SLOT GACOR the actual line wins will be considerably bigger. I advise this same tip for those progressive type slots like Megabucks and Wheel of Fortune. Ever bet one coin onto the wheel and end up getting the bonus wheel symbol within third wheel only to grind your teeth if this happens?? It happened for the best of us, yet doesn’t ever need location again.
When CRYPTO BET77 go for doing it? Let’s face it, small wins will not keep you cheerful for a long. You’re there for the big win, even so, if should you go for the? Wait until the progressive jackpot become spacious. Why go for it when the jackpot is small?
…
If performed with choosing a casino, then it’s time perform. Slots are one of best to play since it does not have complicated rules nor does it require ways of win. Some other words, a person will have to depend on his good luck, if there is any.
Do not play with the slot machines that are near for the table fanatics. The machines that surround choices said regarding the least paying machines. The casino executives do not keep high paying machines surrounding the table players because presently there a associated with table players getting attracted towards them GAMING SLOT GACOR .
Another advantage that along with a the free online slots undeniable fact that you can browse through multiple slot games and learn ways to play for you to wagering any real revenue.
If you are not yet convinced anyone would rather venture create crowded, smoky, germ laden gambling hall, I still wish you much results. One thing to take into consideration when heading back to a typical big city casino is that without even having to spread out your front door, it’s totally open other doors to winning profit.
Watch out for false advertisements. Some would claim that they don’t ask for fees, but during registration, they will be asking a person credit card details (most likely, your username and password.) Simply don’t give in, even when they propose that it is required for claiming your accolades. One thing a person can do is to obtain the contact details of every GAME ONLINE SLOT behind the area and touch base to folks. Ask if there are other strategies to claim your prizes.
Silver Dollar Casino is giving most desirable range of games. Offering casino games like roulette, slots, video poker, and blackjack. An individual SLOT ONLINE can play these games in their download version and by instant games.
Just a person chose perform online slots for free doesn’t indicate that you are excluded from learning what any slots player has experiences. The tips, tools, facts, as well as any other useful information you actually need before begin playing slots online are always made open to you as well as all new ball players. When heylink.me/Kuda189 begin playing slots online, hard work an option on this particular which can offer you possibility to to decide to play for the money or for entertainment.
…
Strengths: This is often a very strong defensive formation and Iniesta and his world of creativity being on the pitch. It was used associated with away game against Almeria in they can didn’t make a chance, or as the Spanish statisticians calls it: “Occasiones de gol”. Additionally it wasn’t even though Almeria can be a bad team that can’t create the designer probably. The weekend after playing Barca they dominated at Real Madrid and were very unlucky to be behind at half-time.
3- Always save your game reduces your PC’s hard drive regularly. It not just prevents your micro SD from being corrupted, and it also enables you to begin from the same stage SLOT GAMING in left this.
Hombrew and ROMs could be added to your GAME SLOT card with a simple click and quit. One just has to ensure to create respective folders wherein the files could be dropped.
So really what is really so great within this? Well a person are now insurance coverage practice. What in the world does which means that? This is actually an important factor for the serious fruit machine player. Some folk take the far more seriously the particular ones that simply enjoy them for just a little bit of leisure activities.
Slots that exist in coffee houses and cafes are frequently programmed as hot slots. The attractive bright lights and the inviting sounds of the slot machines have this enticing effect to individuals who’re eating to finish their foods quickly to help them play slot games at that time.
Fruit machines are famous for having more than several special has. Features such as nudges, holds and funds ladders are almost exclusive to fruit maker. The Hulk fruit machine has contemplating and a good deal. The Incredible Hulk slot machine even offers two game boards in activate a variety of special features and win cash cash payouts. As you can expect from the sheer involving features for your Hulk slot machine, can make the SLOT GAME very busy that carries a lot going on the screen at all times. It may take some used to, however it really only requires a few spins to healthy greater understanding of the Hulk fruit terminal.
If three or more symbols appear from left to right you get what is known as a Spiderman feature. When this feature is triggered the participant can decide upon two features called free spins or venom.
In a best machine, you must calculate exactly how much it can cost you perform. Slot machines differ from another. Some are that will give you more winnings than other people. MAHA BET 77 is the reason it is very for a person to know that are those you can let you more earn. One way to choose which with the machines can the best ones perform with, always make comparisons on the different games anyone have had and back again to device that can to offer you with superior amount of profit.
…
Blackjack or 21 is considered among the easiest casino games understand and convincingly play. The idea of the game is to find a hand closer to 21 compared to dealer. When playing Blackjack, regardless which of a lot of versions you could be playing, sport is between you and also the dealer in spite of how many players are and your table. Practice free, various versions of Blackjack and find out the game you like best. Once you have determined your game chosen develop something you will utilize in a real money game. You can pocket some serious money in this game and might be available in download and flash versions as well as Live Dealer On-line casinos.
There is a lot of benefits in playing slots online. MAHABET 77 , it will be less. Two, you don’t will want to drive yourself to the casinos and back. Three, there are many great offers which you can savor in many online gambling. Upon signing up, new registrations may have the ability to acquire freebies and sometime an initial amount a person bankroll. Fourth, online slots are GAME SLOT easy to practice with. Spinning is just some kind of a click of the mouse all period. You can select pay lines, adjust your bets, and cash out using only your sensitive mouse.
A player just downloads the game and clicks the ‘tournament’ button planet lobby for the online gambling establishment. There are instructions to follow as well as the player follows these. First, he registers and after that, he’ll see the time he is to the front runner. The entrance fee costs as low as $2 to $5 24 hours.
The main thing was that I to spend your money he was required to positively playing SLOT CASINO . Now the Hanabi Full Screen Skill Stop Slot Machine wasn’t within local casino, but it had been similar a new lot of other Casino Slot Machines he strummed. The basic one, two, or three coins per spin, but earn money . difference was this one didn’t have one of us pull-down levers on the inside. It seemed a extra up-to-speed this times despite the fact that it was refurbished simply by itself.
Then watch as the different screens point out. The title screen will show the name of the program and sometimes the maker. The game screen will show you what program it employs. You need to look at certain regarding that screen to determine how to play that particular machine.Also, examine will usually tell you how high the Cherry and Bell Bonus go. Doable ! usually tell whether or the cherries go to 12, 9, 6 or 3, as well as whether the bells go 7, 3 or 2. The best ones to beat are ones that cherry’s pay a visit to 3 and bells check out 2.These normally takes less with regard to you play and much less money to strike.
One question that gets asked all of the time is where can I play Monopoly slots on-line? The answer is that you have a home the United States, you’re kind of. Wagerworks makes on online version SLOT ONLINE for the game. But, as this date, the casinos in which powered this particular software do not accept US players. So, for now, you must visit a land based casino to play this title.
The Lord of the Rings Video slot is a Pachislo Slot Machine, indicates that realize that some be that can control as soon as the reels will get rid of spinning while having turn. This allows you to infuse some slot machine experience by using a bit more skill! The slot machine also incorporates a mini game that is offered for for you to definitely play between spins.
In a gambling scenario, it’s all about odds. No machine always be set to let gamers win every single time. However, administrators must be careful not to keep winning all time because can scare players away. Occasionally, gamers must win and that will attract significantly players.
…
Back your good old days, my local freinds and I would personally head almost the mall arcade area with a roll of quarters and play various other on the trail Fighter mission. For hours we would trip choosing different guys and who would have thought that 15 years later we’re still all hanging out together. Faster I accidentally came down the street Fighter Skill Stop Slot machine we just had for having one of these Antique Slots for dwelling.
Slot machines are a game title of chance. There really is no skill involved. For site06.gg189.live if you win is depending on the number of drums within machine and the variety of combinations that occur on such basis as these drums and value.
The slots are hosted by finest casinos online, so there is no compromise on the graphics along with the speed of access. Even slot the ball player chooses starts off with 50,000 credits, enough assist you sustain for hrs .. What’s more, every time you visit the site, the credits are replaced!
At these casinos they’ll either lets you enter a free mode, or give you bonus rotates. In the free mode they will give you some free casino credits, which not have any cash worth. What this allows you to do is use the various games that take prescription the SLOT GAMING world wide web site. Once you have played a online slot machine that you like the most you end up being comfortable with it once setting up to play for dough.
Marvel Comics has shot through the cover in reputation. With all of the recent Marvel feature films, Marvel has evolved from GAME SLOT automobile that only teenage boys knew to that has developed into household determine. With heroes like Spiderman, Iron Man, and the incredible Hulk, everyone has some type of hero to find to. But there is however probably ugh to incorporate the superhero fun into the fun in the place of Las Vegas weekend better? Wrong! With the Marvel Comic Heroes Slot Machine, you get all finding out that you dreamed of as in my teens.
First, try to are at home with the associated with SLOT GAME you are playing with. Win or lose, it critical that you like every minute of recreation. Different SLOT GAME have different terms. For instance, there are both progressive and non-progressive exercises.
First, to be able to to consider the fact that you can play these games anytime and anywhere weight are not healthy. There normally comfort take into account there that entices people to go online and start hitting. For as long as anyone could have your computer, an internet connection, your own or debit card with you, in order to set and able to to play the game of. That means place do this at the comforts of the own home, in your hotel room while on business trips, and even during lunch break at your house of hard work. You don’t must be anxious about people disturbing you or stepping into fights and dealing while using the loud recent music. It is just like having your own private VIP gaming room at your personal home or anywhere you tend to be in the global.
…
When building the ultimate gaming computer, it isn’t the length and width of the hard disk drive that counts, but its performance genuinely make chatting. A 200GB hard drive is usually more than enough for your storage of your games and applications. You should differences lie in the buffer along with the drive interface. The buffer determines exactly how much data could be stored for pre-fetch while drive interface determines the speed the data can be transferred. The most suitable choice for an ultimate gaming computer is the SATA-2 16MB buffer 200GB hard fire.
The users can avail technical support over home phone. What they have conduct is to call at a given toll-free telephone telephone number. There has been a small amount of case the location where user has complained using this slot machine for their finding any issue with gear.
The 50 Lions Free Spins Bonus game is activated when at least 3 Flower Symbols show on reels 1, 2 and a number of. The Free Spins are played automatically by the slot machine and with this game, additional Diamond Bonus Symbols are added to your reels, a person more SLOT GAMING odds of building winning lines.
The rules and directions for the internet SLOT GAME machines are very much like in a land base casino. First it is established to what amount of cash to push and pull on. After that, the decision about what number of coins to place bet with spin relates. With the online slot machines, one can pick between 1, 3 next up to 9 paylines. It is straightforward that additional paylines one bets on, the funds he spends, but furthermore the chances of getting more money are higher too. You would like that comes is clicking the spin button. The noise of the spin can be heard exactly the same way like from a land based casino; a wonderful fun and excitement of the comfort of home.
There some benefits in playing slots online. One, it is cheaper. Two, you don’t want to drive yourself to the casinos and home. Three, there are many great offers which you can experience in many online on line casino. Upon signing up, new registrations may have the ability to acquire freebies and sometime an initial amount a person bankroll. Fourth, online slots are easy to compete with. Spinning is just an issue of a click of the mouse all time. You can select pay lines, adjust your bets, and cash out using only your mouse button.
Just for the sake of experiencing a guide, let’s along with Limsa Lominsa as our city. Inside the game, your first location open for a boat that is bound for Limsa Lominsa City. During SLOT RTP TINGGI , ship suddenly is under pressure and require it and it need to combat against monsters that can attacking the ship. Action basically a tutorial for newbies in recreation and will certainly help you in advantages of the FFXIV especially the actual battle entire body.
1) Lord of the Rings – this new slot GAME SLOT will be eye exposing. The graphics are absolutely top notch, following the film closely, with involving video clips too. The range of bonus games also clarifies that it’s stand away from the crowd. The visuals and also the game play make video real be prominent game to be able to tried.
It been recently already admitted to really that the Climax Skill Stop Slot Machine is the single most user-friendly slot machines that might be used or available on the markets. A one-year warranty is given at the time of the purchase of the console.
…
As truck the reel stops, you should check should you have got any winning hybrid. Generally the winning amount is shown in Sterling. If you have won something, perhaps click around the payout office. It is impossible to know that which you’d be winning as unpredictability is the second name in the slot game. If you do not win, try playing a different game.
First, you have to consider the truth you can enjoy these games anytime and anywhere men and women. There is that comfort factor within that entices people pay a visit to online as well as playing. So long as you have your computer, an internet connection, your or debit card with you, are usually set and able to play. SLOT ONLINE Speaking about . you are able to do this in the comforts of your home, in your hotel room while on business trips, and even during lunch break at your home of work. You don’t have to be bothered about people disturbing you or entering into fights and dealing with the loud favorite tunes. It is like having one’s own VIP gaming room at your house or anywhere you may be in the world.
In a casino ligne however, things are narrowed primarily based on your remedy. No more walking around tables, watching people play and waiting towards the turn to stay on the table and play. With the latest computer trends nowadays, things would love gone simpler this a moment.
If you had been lucky enough to win on a youtube video slot machine, leave that machine. Don’t think that machine could be the ‘lucky machine’ for your company. It made you win once about the will not let upon the next games without. Remember that slots are regulated by random number generator and could electrically motorized. In every second, it changes effectiveness of symbols for GAMING SLOT GACOR many times. A great number of of the time, the combinations are not in favor of you may. If you still have the time or remaining balance in your allotted money, then maybe you can try the other slot turbines. Look for the slot machine game that offers high bonuses and high payouts but requiring fewer coins.
If you had been lucky enough to win on a slot machine, leave that machine. Do not think that machine may be the ‘lucky machine’ for somebody. It made you win once even so it will not let you on the next games without. Remember that pai gow poker are regulated by random number generator and individuals electrically harnessed. In every second, it changes gas of symbols for 500 times. And most of the time, the combinations are not in favor of anybody. If you still experience the time or remaining balance in your allotted money, then perhaps you can try the other slot equipments. Look for VEGETA 9 that offers high bonuses and high payouts but requiring fewer coins.
Tip #2 Learn in regards to the house rules of each casino, much better the house rules, greater money you certainly will win GAME ONLINE SLOT in the long run. And yes, your laws do vary between gambling establishments.
Get realize your grasp the game close to machine, is just very essential for the fresh players. The participants who are online maybe land casinos should always maintain in mind that they get amply trained with video game that are usually playing for the machines. Is certainly every player’s dream november 23 on a slot machine.
…
What then are the advantages of roulette over slots and the other way round? To begin with, let’s together with the specifications. Both are simple and fast-paced games, but with debate, slots is definitely faster and much easier than live. This game is also easier to comprehend than roulette, and you might only take a few rounds to figure out which patterns win and which ones lose.
It’s really too bad I missed the Hanabi Full Screen Skill Stop Slot Machine sooner, because at first I was searching for the Best Slot machines that dispersed money. Seriously, it didn’t even dawn on me that everything had switched over to electronic tickets until about three months once we started being. Just goes to demonstrate how much he was winning. It’s nice to learn that these Antique Pai gow poker give you tokens to gift that old time ask it.
One involving ensuring your high associated with winning big amounts dollars is by choosing what machine conflicts you. JURAGAN 4D is the straight slot machine. It is sometimes called the non-progressive port. This always pays winnings in accordance with an established payout schedule. Note that it pays with exactly the amount continuously when players hit a special SLOT ONLINE symbol formula of.
If you pass just a little money, regardless of whether it isn’t progressive jackpot, edit and appreciate your prize money. For do never the money you have set for their own end for time meet from wearing non-standard and several minutes . in for each day or pair.
#5: Your life can change in a split second. See #4. The only way your life can change at a personal game like Roulette is for everything you possess and bet it in a spin of this roulette take. In slots you can be playing the way you normally play right after which boom – suddenly you’ve just won $200k.
In a nutshell, the R4 / R4i is only a card which enables for you to run multimedia files or game files on your DS. No editing of the system files is required; it is strictly a ‘soft mod’ that has no effect on your NDS in however. You just insert the R4i / R4 card into the GAME SLOT, and the R4 / R4i software will jog.
(3) This is SLOT CASINO one of the best options for online casinos, the Live Dealer Home. These are the most interactive version of the online casino when a live dealer through a relevant video feed from an actual land based casino will greet most people. You can interact with the dealer and with other players who may be playing sign in table. Live dealer casinos will provide a real casino experience never having to leave property.
The bad-paying and well-paying slot machines are usually located aside from each several other. Are you not successful at one machine, the next one is liable going to produce better satisfaction. Have an open eye for people who never leave the equipment they are playing – they are generally waiting to enjoy a pay, or they possess a loose machine and stick with it winning. Would likely be like to attempt out that machine and observe how well it works best you. The most important thing to remember is just insert the $5 bill into the device – i recommend a person can place the particular bet more than a first spin, as which isn’t where most jackpots are won.
…
In a gambling scenario, it’s concerning odds. No machine always be set to permit gamers win every single time. However, administrators need to be careful never to keep winning all time because this also scare players away. Occasionally, gamers must win which will attract even more players.
They online slot games have a range of pictures, from tigers to apples, bananas and cherries. When you get all three you take home some loot. Many use RTG (Real Time Gaming) while it is one with the top software developers for your slots. These includes the download, a flash client and are mobile, absolutely take your game anywhere you to be able to go. Additionally, there are Progressive slots, you can easily win a lifetime jackpot and also you only be required to pay out a few dollars, as with most gambling, the likelihood of winning the jackpot comparable winning a lottery, not good, however fun. With to play as many coins you’ve to win the jackpot, the risk is higher and making use of the pay up.
This article summarizes 10 popular online slot machines, including SLOT ONLINE For the Reels Turn, Cleopatra’s Gold, Enchanted Garden, Ladies Nite, Pay Airborne dirt and dust!, Princess Jewels, Red White and Win, The Reel Deal, Tomb Raider, and Thunderstruck.
Their tournament lobby should be considered jumping with action. 24/7 there is a tournament SLOT CASINO began on for all players. Every hour, VIP players obtain a freeroll tournament to enter, along with also goes on around contributions. Special event tournaments and more are grounds for additional matches.
Knowledge with the payback number of slot machine and any time it would wear winning. This is extremely important important because ever machine is programmed with a payback percentage in their microprocessors. PRIMA BET 78 , all of the times how the house wins are already predicted. Usually that is just about 90 to 97 percent of the time. The idea is that the higher the percentage is, much more payback in all probability. Casinos have comes around because to merely encourage players to continue to playing within slot brewers. So if you are a player, you’ll need to keep track of those machines with superior terms the higher paybacks and be sure you keep a close eye on him or her.
Here are a few tips on how to calculate the cost per angle. When you are developing the casino, you may use you mobile phone devices so you simply can perform the calculations. Perhaps the most basic mobile phone these days is along with a calculator tool. In calculating cost per spin, you would need to GAME SLOT multiply the game cost, greatest line, and the number of coin initial ante. For example, should your game set you back $0.05 in 25 maximum lines, multiply $0.05 and 9 maximum lines times 1 coin bet. Signifies that that it may cost you $0.45 per spin if you are playing 9 maximum lines to obtain a nickel machine with one minimum coin bet. This particular really is one strategy which you can use to win at casino slot equipments.
There are two varieties of slot cars, there may be the analog cars and the digital types. The traditional or analog slot cars are folks that you might remember when using the younger amount of days. This is where it was one car per slot and also the car in order to stay as they slot for the whole race.
One of your great reasons for having playing by going online is its simplicity for mechanics. You’ll want to to insert coins, push buttons, and pull carrying handles. So that you can spin the reels to win the prize, it will only take a click of ones mouse button to achieve that. If you want to raise or decrease your bets or cash out the prize within the to do is to still click on the mouse.
…
If happen to be playing a progressive slot and your bankroll is simply short perform max coins, move down a coin size. Instead of playing the dollar progressive games, have fun with the quarter progressive games. Fine as long as can play max coins, you can land the jackpot on that game.
Slot machines are a rather less harmful way to look at charge of how much you lose and win. It is a way wherein could possibly play having a relaxed mind and do not need to plot, plan, or guess. Here the luck takes can charge. Well, almost!
172.232.238.121 at $60.00 and Roku 2 HD at $80.00 still come whilst IR remote, however safe and sound . the newer remote control, that includes an Angry Birds license separately.
Once you have decided the type of SLOT GAME happen to be comfortable with, the next phase is select a machine that you think have the particular chance of letting shipped to you. Here is the key tip: It’s not really the sort of game it’s. To choose a winning machine, you spend more focus on how administrators manage the machines.
Try to go to your favorite search engine and explore slot machine games reduce. You’ll be surprised at the number of search negative effects of websites and pages that allow you get pleasure from this game to the fullest without risking just one single dollar. So for those out there who would like to experiment with this game but are frightened to lose hard-earned money, you undoubtedly try playing it the internet.
On to bigger, better things, you ought to look at how much MB of memory greeting card has and whether just one or two an AGP or PCI graphics visa card. In order to find out whether your slot a AGP or PCI Click Here, money making plans the little by little on the way to figure this out. And locate out just how much MB or memory require to its really up a person. It ranges from about 128MB to 768MB depending on how great excess weight and fat your Pc games to be. Most of the better games require GAME SLOT significantly greater one that will perform rather well, as well as a higher memory. You will discover you shouldn’t really ought to check much else, the you buy (if fairly new) should come with all the newest shaders and parts tact for the unit.
Carrera cars are miniature cars guided by a groove (or “slot”) the actual planet track. Though most consider them regarding toys useful only for entertainment person, Carrera cars can be also used as kids learning toys.
…
They online slot games have so many different pictures, from tigers to apples, bananas and cherries. When acquire all three you win. KRATON BET (Real Time Gaming) free of charge one from the top software developers for that slots. These includes the download, a flash client and are mobile, however take your game anywhere you in order to be go. There are also Progressive slots, you can really win the century jackpot and also only pay out a few dollars, as with all gambling, the chances of you winning the jackpot is like winning a lottery, few good, yet it’s fun. Pertain to to play as many coins you have to win the jackpot, threat is higher and to work with ? the pay.
SLOT GAMING Now just how the same question again but this time in a whole different situation. Who wants to hold a car race with really cool Carerra slot cars? Okay, now are generally talking!
Features: Daredevil Jackpot Slot is five reel and 20 pay lines SLOT GAME. This label baled maybe the dead just about team which gained immense amount of popularity regarding sixties. It has been developed by Playtech laptop or computer. Therefore the slot game portrays the daredevil great enemies. The amount of oil value you can wager is between all the different $0.01 to $5.00. Exactly what which could be wagered is $1000. The biggest jackpot is of 5000 coins and so you can win $250,000 if you happen to obtain the daredevil hero Matt Murdock five particular times. You can win $50,000 if you hit the second highest jackpot which covers either four Matt Murdock or five Elektra Natchios. There can be a third highest jackpot for 750 coins and $37,500 if a person 5 Wilson Fisk.
At these casinos they’ll either allow you to enter a free of charge mode, or give you bonus re-writes. In the free mode they hand you some free casino credits, which do not cash really worth. What this allows you to do is have fun with the various games that take prescription the spot. Once you have played a online slot machine that you favor the most you are usually comfortable in addition to once setting up to play for wealth.
In the actual best machine, you must calculate what amount it can cost you perform. Slot machines differ in one another. Some are willing to give you more winnings than the others. That is why it is important for anyone to know that are those absolutely let you receive more net profit. One way to settle on which with the machines can the best ones perform with, always make comparisons on the various games anyone have had and back again to to the equipment that has the capacity to to along with with the best amount of profit.
First, set yourself to play. Be sure to get afflicted with cash. They not receive vouchers in playing slot. Then, set an comprises spend for the day on that program. Once you consumed this amount, stop playing and come GAME SLOT back again next time. Do not use of one’s money inside one sitting and setting up. Next, set your time alarm. Once it rings, stop playing and move out from the casino. Another, tell yourself to abandon gear once shipped to you the slot tournament. Do not be so greedy thinking that you want more victories. However, if you still have money with your roll bank, then you may still try other slot games. Yes, do not think that machine your own had won is fortunate enough to create win over and over again. No, it will just exhaust all money and pause to look for lose very much.
#5: Your life can change in a split second. See #4. As it’s a lucrative way your own can change at a match like Roulette is prone to take all you own and bet it in one spin in the roulette tyre. In slots you can be playing approach you normally play and then boom – suddenly you’ve just won $200k.
…
The player of this machine will first insert the token into gear. Then pull the lever or press the device. KRATONBET is positioned in motion to rotate with specific picture when you strike it. Whenever the ball player wins is determined that pictures is line with the pay line all of the middle for the viewing tv screen. Winning combinations vary according towards rules for this particular on the internet game. Only then will the slot will payout the one who did that. The winning area of a video slot is 82-92%.
The science behind a software system is really a number of codes, all in number designed to at some point. This value then dictates a solution, often many the same number. You are either an optimistic or a damaging strike vector will be processed, meaning the programme will progress forward or return within a loop. These loops include the provisions for getting a potential matchup and GAMING SLOT GACOR the prospects of winning.
Lucky Charmer – This online slot is best known for good bonuses. You will see a second screen bonus feature. There are 3 musical pipes, and if you achieve bonus round, the charmer plays selecting. But, to activate the bonus round, you always be able hitting the King Cobra at the 3rd pay-line.
Slot machines are certainly one the attractions in casinos. With these machines, the ball player need end an expert to win. He does not ought to be able at strategies or math to generate the odds in his favor. Video poker machines are played purely on luck SLOT ONLINE and merely about anybody who is of legal age can be. Today, free slot machine game games play online which enables it to be accessed from basically any gaming websites on the internet. These games may be played with real money or basically for fun simply no money demanded.
The roulette table always draws a crowd in a real world betting house. The action is almost hypnotizing. Watch the ball roll round and if it lands all over your number, you win. The problem is that many 37 or 38 slots for that ball to fall into and the odds for this game are clearly in the homes favor. Keeping the roulette, explore for European Roulette which just has 37 slots (no 00) and keep in mind the single number bets carry the worse odds. Consider betting group, rows or lines of numbers and you might spend much longer at the table.
With English Harbour Casino bonuses, your eye area will surely pop completly. They are producing 100% match bonus GAME ONLINE SLOT areas up to $275 for first account. And for minimum deposit of $100 you avail this bonus.
Red White and Win is a timeless 3-reel, single pay-line progressive slot from Vegas Technology. There are 13 winning combinations. Symbols on the reels include USA Flag, Bald Eagle, George Washington, Statue of Liberty, and Dollars.
…
First off, online slots offer all of the fun and excitement of live slots but of the comfort of one’s own to your home. You don’t in order to be waste time and money travelling all means to an out of town e-casino. Actually the nicest thing about this is that may do play anyone want for as long when want. Which don’t must be play only if you possess a 3 hour block absolve to play.
These three games allow players the following strategies which can help sway the odds in their favor. But keep in mind, you have to on line to use the GAME ONLINE SLOT games make sure to obtain the best options. If you am not aware of what you’re doing, you are going to be better off playing the slots xbox games.
Before anything else, you should bring a hefty quantity money with you. This may be very risky particularly if displayed within a public place, so protective measures ought to exercised.
You have hundreds of choices autumn to playing slot machines online. Lots of different software platforms offering everything from three reel and 5 reel machines to video, bonus and jackpot progressive affiliate marketor payouts. You can choose from downloading an entire software suite including the games or even just play the absolutely no download version which opens your favorite game with your computer screen window without more than the free account and mouse click of the mouse.
The traditional version associated with the game end up being modified by simple changes to be interesting, and so as two strategy of Checkers increased, different versions with this particular SLOT ONLINE game came out. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
REPUBLIK 365 is really an issue especially when you’ve got other financial priorities. Internet gaming, a person spend for air fare or gas just to visit cities like Las Vegas and participate in the casinos. You will save a great deal of money because internet site . spend for plane tickets, hotel accommodations, food and drinks and also giving prevent the waiters and stores. Imagine the cost of all of the following if could be go all the way to a casino just to play.
Here could be few useful information for choosing the best online casino slot action. First, all of the aforementioned establishments construct a GAMING SLOT GACOR first deposit bonus, so make sure you have a look. You need to learn over guidelines and regulations very carefully, because some of them tough easier to pick up than some others. This is just “Free” money may are giving you, so don’t damage.
Once you know where happen to be going to host your party after that you will need to set to start a date and spare time. If you made the decision to be concerned in a vendor show, then they’ll set the date. These be in order to pick as well as effort slot.
…
First off, online slots offer all of the fun and excitement of live slots but of the comfort of one’s own to your home. You don’t in order to be waste time and money travelling all means to an out of town e-casino. Actually the nicest thing about this is that may do play anyone want for as long when want. Which don’t must be play only if you possess a 3 hour block absolve to play.
These three games allow players the following strategies which can help sway the odds in their favor. But keep in mind, you have to on line to use the GAME ONLINE SLOT games make sure to obtain the best options. If you am not aware of what you’re doing, you are going to be better off playing the slots xbox games.
Before anything else, you should bring a hefty quantity money with you. This may be very risky particularly if displayed within a public place, so protective measures ought to exercised.
You have hundreds of choices autumn to playing slot machines online. Lots of different software platforms offering everything from three reel and 5 reel machines to video, bonus and jackpot progressive affiliate marketor payouts. You can choose from downloading an entire software suite including the games or even just play the absolutely no download version which opens your favorite game with your computer screen window without more than the free account and mouse click of the mouse.
The traditional version associated with the game end up being modified by simple changes to be interesting, and so as two strategy of Checkers increased, different versions with this particular SLOT ONLINE game came out. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
REPUBLIK 365 is really an issue especially when you’ve got other financial priorities. Internet gaming, a person spend for air fare or gas just to visit cities like Las Vegas and participate in the casinos. You will save a great deal of money because internet site . spend for plane tickets, hotel accommodations, food and drinks and also giving prevent the waiters and stores. Imagine the cost of all of the following if could be go all the way to a casino just to play.
Here could be few useful information for choosing the best online casino slot action. First, all of the aforementioned establishments construct a GAMING SLOT GACOR first deposit bonus, so make sure you have a look. You need to learn over guidelines and regulations very carefully, because some of them tough easier to pick up than some others. This is just “Free” money may are giving you, so don’t damage.
Once you know where happen to be going to host your party after that you will need to set to start a date and spare time. If you made the decision to be concerned in a vendor show, then they’ll set the date. These be in order to pick as well as effort slot.
…
First off, online slots offer all of the fun and excitement of live slots but of the comfort of one’s own to your home. You don’t in order to be waste time and money travelling all means to an out of town e-casino. Actually the nicest thing about this is that may do play anyone want for as long when want. Which don’t must be play only if you possess a 3 hour block absolve to play.
These three games allow players the following strategies which can help sway the odds in their favor. But keep in mind, you have to on line to use the GAME ONLINE SLOT games make sure to obtain the best options. If you am not aware of what you’re doing, you are going to be better off playing the slots xbox games.
Before anything else, you should bring a hefty quantity money with you. This may be very risky particularly if displayed within a public place, so protective measures ought to exercised.
You have hundreds of choices autumn to playing slot machines online. Lots of different software platforms offering everything from three reel and 5 reel machines to video, bonus and jackpot progressive affiliate marketor payouts. You can choose from downloading an entire software suite including the games or even just play the absolutely no download version which opens your favorite game with your computer screen window without more than the free account and mouse click of the mouse.
The traditional version associated with the game end up being modified by simple changes to be interesting, and so as two strategy of Checkers increased, different versions with this particular SLOT ONLINE game came out. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
REPUBLIK 365 is really an issue especially when you’ve got other financial priorities. Internet gaming, a person spend for air fare or gas just to visit cities like Las Vegas and participate in the casinos. You will save a great deal of money because internet site . spend for plane tickets, hotel accommodations, food and drinks and also giving prevent the waiters and stores. Imagine the cost of all of the following if could be go all the way to a casino just to play.
Here could be few useful information for choosing the best online casino slot action. First, all of the aforementioned establishments construct a GAMING SLOT GACOR first deposit bonus, so make sure you have a look. You need to learn over guidelines and regulations very carefully, because some of them tough easier to pick up than some others. This is just “Free” money may are giving you, so don’t damage.
Once you know where happen to be going to host your party after that you will need to set to start a date and spare time. If you made the decision to be concerned in a vendor show, then they’ll set the date. These be in order to pick as well as effort slot.
…
Now an individual able in order to the benchmark and personal computer is wanting to score beautifully. Now, you are positioned to start playing the sport. As mentioned earlier, there will be wonderful deal of updates that can need get every now and then. REPUBLIK365 are on a peer to look network. These updates can take a nevertheless. One things that all of us have discovered is that in case your computer is hardwired to the network, downloads would usually take couple of hours but We had arrived never in the position to finish the downloading of updates through wireless. Well-liked the time where in you will truly think really difficult as to what you really need to continue in the game, be it a spell caster, tank, a damage dealer, or alternatively a full support character. Calling it get with an a final decision, lessons also relation to your expertise in playing closing Fantasy XIV game.
Double/Triple Symbols: Whenever these symbols be found in GAME SLOT the center of a single payline slot in conjunction with other symbols creating an absolute combination, the payoff amount is doubled or tripled. Two or three of them same symbols increase the jackpot pay out.
There is advantage a number of SLOT GAME machines as the payouts are averagely set high comparable to the land based slots in Las vegas. There is an interesting thing that before playing for real money, one can possibly play higher than normal odds slot machine games for liberated to practice.
There are surely no hard and fast rules to win these slot games we can obviously increase your chances of winning. Before playing many of the slot games, you must set your win and loss limits in order to play safe. This must be achieved as it’ll help you to economise from your bankroll. Win limit is the particular amount that a gambler is prepared to lose in case if he loses sport. The player must immediately stop playing various other sites . he meets this define. On the other side, if a gamer is happy with the amount he has won much can stop playing the. However, it is very important to follow these limits as a way to maximize your bankroll for any future pastime.
Slots that exist in SLOT GAMING train stations and cafes are frequently programmed as hot slots. The attractive bright lights and the inviting sounds of the slot machines have this enticing effect to those who are eating to finish their foods quickly so as to play slot games today.
As you play a slot machine, money management is probably the most important factors may perhaps affect your success. If you might be able to manage your money wisely, are going to have better amount associated with which absolutely spend enjoying. You need comprehend when strengthen bets or decrease it at the most beneficial moment to make certain that you take pleasure in winning and playing at the same effort.
2) King Kong – the King Kong Slot also wins in the graphics section. While it does not have as tons of bonus games as Lord of the Rings, it is normally brilliant when the fearsome ape busts his way through one belonging to the reels when you have picked up a secure!
…
First off, online slots offer all of the fun and excitement of live slots but of the comfort of one’s own to your home. You don’t in order to be waste time and money travelling all means to an out of town e-casino. Actually the nicest thing about this is that may do play anyone want for as long when want. Which don’t must be play only if you possess a 3 hour block absolve to play.
These three games allow players the following strategies which can help sway the odds in their favor. But keep in mind, you have to on line to use the GAME ONLINE SLOT games make sure to obtain the best options. If you am not aware of what you’re doing, you are going to be better off playing the slots xbox games.
Before anything else, you should bring a hefty quantity money with you. This may be very risky particularly if displayed within a public place, so protective measures ought to exercised.
You have hundreds of choices autumn to playing slot machines online. Lots of different software platforms offering everything from three reel and 5 reel machines to video, bonus and jackpot progressive affiliate marketor payouts. You can choose from downloading an entire software suite including the games or even just play the absolutely no download version which opens your favorite game with your computer screen window without more than the free account and mouse click of the mouse.
The traditional version associated with the game end up being modified by simple changes to be interesting, and so as two strategy of Checkers increased, different versions with this particular SLOT ONLINE game came out. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
REPUBLIK 365 is really an issue especially when you’ve got other financial priorities. Internet gaming, a person spend for air fare or gas just to visit cities like Las Vegas and participate in the casinos. You will save a great deal of money because internet site . spend for plane tickets, hotel accommodations, food and drinks and also giving prevent the waiters and stores. Imagine the cost of all of the following if could be go all the way to a casino just to play.
Here could be few useful information for choosing the best online casino slot action. First, all of the aforementioned establishments construct a GAMING SLOT GACOR first deposit bonus, so make sure you have a look. You need to learn over guidelines and regulations very carefully, because some of them tough easier to pick up than some others. This is just “Free” money may are giving you, so don’t damage.
Once you know where happen to be going to host your party after that you will need to set to start a date and spare time. If you made the decision to be concerned in a vendor show, then they’ll set the date. These be in order to pick as well as effort slot.
…
Now an individual able in order to the benchmark and personal computer is wanting to score beautifully. Now, you are positioned to start playing the sport. As mentioned earlier, there will be wonderful deal of updates that can need get every now and then. REPUBLIK365 are on a peer to look network. These updates can take a nevertheless. One things that all of us have discovered is that in case your computer is hardwired to the network, downloads would usually take couple of hours but We had arrived never in the position to finish the downloading of updates through wireless. Well-liked the time where in you will truly think really difficult as to what you really need to continue in the game, be it a spell caster, tank, a damage dealer, or alternatively a full support character. Calling it get with an a final decision, lessons also relation to your expertise in playing closing Fantasy XIV game.
Double/Triple Symbols: Whenever these symbols be found in GAME SLOT the center of a single payline slot in conjunction with other symbols creating an absolute combination, the payoff amount is doubled or tripled. Two or three of them same symbols increase the jackpot pay out.
There is advantage a number of SLOT GAME machines as the payouts are averagely set high comparable to the land based slots in Las vegas. There is an interesting thing that before playing for real money, one can possibly play higher than normal odds slot machine games for liberated to practice.
There are surely no hard and fast rules to win these slot games we can obviously increase your chances of winning. Before playing many of the slot games, you must set your win and loss limits in order to play safe. This must be achieved as it’ll help you to economise from your bankroll. Win limit is the particular amount that a gambler is prepared to lose in case if he loses sport. The player must immediately stop playing various other sites . he meets this define. On the other side, if a gamer is happy with the amount he has won much can stop playing the. However, it is very important to follow these limits as a way to maximize your bankroll for any future pastime.
Slots that exist in SLOT GAMING train stations and cafes are frequently programmed as hot slots. The attractive bright lights and the inviting sounds of the slot machines have this enticing effect to those who are eating to finish their foods quickly so as to play slot games today.
As you play a slot machine, money management is probably the most important factors may perhaps affect your success. If you might be able to manage your money wisely, are going to have better amount associated with which absolutely spend enjoying. You need comprehend when strengthen bets or decrease it at the most beneficial moment to make certain that you take pleasure in winning and playing at the same effort.
2) King Kong – the King Kong Slot also wins in the graphics section. While it does not have as tons of bonus games as Lord of the Rings, it is normally brilliant when the fearsome ape busts his way through one belonging to the reels when you have picked up a secure!
…
First off, online slots offer all of the fun and excitement of live slots but of the comfort of one’s own to your home. You don’t in order to be waste time and money travelling all means to an out of town e-casino. Actually the nicest thing about this is that may do play anyone want for as long when want. Which don’t must be play only if you possess a 3 hour block absolve to play.
These three games allow players the following strategies which can help sway the odds in their favor. But keep in mind, you have to on line to use the GAME ONLINE SLOT games make sure to obtain the best options. If you am not aware of what you’re doing, you are going to be better off playing the slots xbox games.
Before anything else, you should bring a hefty quantity money with you. This may be very risky particularly if displayed within a public place, so protective measures ought to exercised.
You have hundreds of choices autumn to playing slot machines online. Lots of different software platforms offering everything from three reel and 5 reel machines to video, bonus and jackpot progressive affiliate marketor payouts. You can choose from downloading an entire software suite including the games or even just play the absolutely no download version which opens your favorite game with your computer screen window without more than the free account and mouse click of the mouse.
The traditional version associated with the game end up being modified by simple changes to be interesting, and so as two strategy of Checkers increased, different versions with this particular SLOT ONLINE game came out. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
REPUBLIK 365 is really an issue especially when you’ve got other financial priorities. Internet gaming, a person spend for air fare or gas just to visit cities like Las Vegas and participate in the casinos. You will save a great deal of money because internet site . spend for plane tickets, hotel accommodations, food and drinks and also giving prevent the waiters and stores. Imagine the cost of all of the following if could be go all the way to a casino just to play.
Here could be few useful information for choosing the best online casino slot action. First, all of the aforementioned establishments construct a GAMING SLOT GACOR first deposit bonus, so make sure you have a look. You need to learn over guidelines and regulations very carefully, because some of them tough easier to pick up than some others. This is just “Free” money may are giving you, so don’t damage.
Once you know where happen to be going to host your party after that you will need to set to start a date and spare time. If you made the decision to be concerned in a vendor show, then they’ll set the date. These be in order to pick as well as effort slot.
…
Now an individual able in order to the benchmark and personal computer is wanting to score beautifully. Now, you are positioned to start playing the sport. As mentioned earlier, there will be wonderful deal of updates that can need get every now and then. REPUBLIK365 are on a peer to look network. These updates can take a nevertheless. One things that all of us have discovered is that in case your computer is hardwired to the network, downloads would usually take couple of hours but We had arrived never in the position to finish the downloading of updates through wireless. Well-liked the time where in you will truly think really difficult as to what you really need to continue in the game, be it a spell caster, tank, a damage dealer, or alternatively a full support character. Calling it get with an a final decision, lessons also relation to your expertise in playing closing Fantasy XIV game.
Double/Triple Symbols: Whenever these symbols be found in GAME SLOT the center of a single payline slot in conjunction with other symbols creating an absolute combination, the payoff amount is doubled or tripled. Two or three of them same symbols increase the jackpot pay out.
There is advantage a number of SLOT GAME machines as the payouts are averagely set high comparable to the land based slots in Las vegas. There is an interesting thing that before playing for real money, one can possibly play higher than normal odds slot machine games for liberated to practice.
There are surely no hard and fast rules to win these slot games we can obviously increase your chances of winning. Before playing many of the slot games, you must set your win and loss limits in order to play safe. This must be achieved as it’ll help you to economise from your bankroll. Win limit is the particular amount that a gambler is prepared to lose in case if he loses sport. The player must immediately stop playing various other sites . he meets this define. On the other side, if a gamer is happy with the amount he has won much can stop playing the. However, it is very important to follow these limits as a way to maximize your bankroll for any future pastime.
Slots that exist in SLOT GAMING train stations and cafes are frequently programmed as hot slots. The attractive bright lights and the inviting sounds of the slot machines have this enticing effect to those who are eating to finish their foods quickly so as to play slot games today.
As you play a slot machine, money management is probably the most important factors may perhaps affect your success. If you might be able to manage your money wisely, are going to have better amount associated with which absolutely spend enjoying. You need comprehend when strengthen bets or decrease it at the most beneficial moment to make certain that you take pleasure in winning and playing at the same effort.
2) King Kong – the King Kong Slot also wins in the graphics section. While it does not have as tons of bonus games as Lord of the Rings, it is normally brilliant when the fearsome ape busts his way through one belonging to the reels when you have picked up a secure!
…
First off, online slots offer all of the fun and excitement of live slots but of the comfort of one’s own to your home. You don’t in order to be waste time and money travelling all means to an out of town e-casino. Actually the nicest thing about this is that may do play anyone want for as long when want. Which don’t must be play only if you possess a 3 hour block absolve to play.
These three games allow players the following strategies which can help sway the odds in their favor. But keep in mind, you have to on line to use the GAME ONLINE SLOT games make sure to obtain the best options. If you am not aware of what you’re doing, you are going to be better off playing the slots xbox games.
Before anything else, you should bring a hefty quantity money with you. This may be very risky particularly if displayed within a public place, so protective measures ought to exercised.
You have hundreds of choices autumn to playing slot machines online. Lots of different software platforms offering everything from three reel and 5 reel machines to video, bonus and jackpot progressive affiliate marketor payouts. You can choose from downloading an entire software suite including the games or even just play the absolutely no download version which opens your favorite game with your computer screen window without more than the free account and mouse click of the mouse.
The traditional version associated with the game end up being modified by simple changes to be interesting, and so as two strategy of Checkers increased, different versions with this particular SLOT ONLINE game came out. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
REPUBLIK 365 is really an issue especially when you’ve got other financial priorities. Internet gaming, a person spend for air fare or gas just to visit cities like Las Vegas and participate in the casinos. You will save a great deal of money because internet site . spend for plane tickets, hotel accommodations, food and drinks and also giving prevent the waiters and stores. Imagine the cost of all of the following if could be go all the way to a casino just to play.
Here could be few useful information for choosing the best online casino slot action. First, all of the aforementioned establishments construct a GAMING SLOT GACOR first deposit bonus, so make sure you have a look. You need to learn over guidelines and regulations very carefully, because some of them tough easier to pick up than some others. This is just “Free” money may are giving you, so don’t damage.
Once you know where happen to be going to host your party after that you will need to set to start a date and spare time. If you made the decision to be concerned in a vendor show, then they’ll set the date. These be in order to pick as well as effort slot.
…
Now an individual able in order to the benchmark and personal computer is wanting to score beautifully. Now, you are positioned to start playing the sport. As mentioned earlier, there will be wonderful deal of updates that can need get every now and then. REPUBLIK365 are on a peer to look network. These updates can take a nevertheless. One things that all of us have discovered is that in case your computer is hardwired to the network, downloads would usually take couple of hours but We had arrived never in the position to finish the downloading of updates through wireless. Well-liked the time where in you will truly think really difficult as to what you really need to continue in the game, be it a spell caster, tank, a damage dealer, or alternatively a full support character. Calling it get with an a final decision, lessons also relation to your expertise in playing closing Fantasy XIV game.
Double/Triple Symbols: Whenever these symbols be found in GAME SLOT the center of a single payline slot in conjunction with other symbols creating an absolute combination, the payoff amount is doubled or tripled. Two or three of them same symbols increase the jackpot pay out.
There is advantage a number of SLOT GAME machines as the payouts are averagely set high comparable to the land based slots in Las vegas. There is an interesting thing that before playing for real money, one can possibly play higher than normal odds slot machine games for liberated to practice.
There are surely no hard and fast rules to win these slot games we can obviously increase your chances of winning. Before playing many of the slot games, you must set your win and loss limits in order to play safe. This must be achieved as it’ll help you to economise from your bankroll. Win limit is the particular amount that a gambler is prepared to lose in case if he loses sport. The player must immediately stop playing various other sites . he meets this define. On the other side, if a gamer is happy with the amount he has won much can stop playing the. However, it is very important to follow these limits as a way to maximize your bankroll for any future pastime.
Slots that exist in SLOT GAMING train stations and cafes are frequently programmed as hot slots. The attractive bright lights and the inviting sounds of the slot machines have this enticing effect to those who are eating to finish their foods quickly so as to play slot games today.
As you play a slot machine, money management is probably the most important factors may perhaps affect your success. If you might be able to manage your money wisely, are going to have better amount associated with which absolutely spend enjoying. You need comprehend when strengthen bets or decrease it at the most beneficial moment to make certain that you take pleasure in winning and playing at the same effort.
2) King Kong – the King Kong Slot also wins in the graphics section. While it does not have as tons of bonus games as Lord of the Rings, it is normally brilliant when the fearsome ape busts his way through one belonging to the reels when you have picked up a secure!
…
Now an individual able in order to the benchmark and personal computer is wanting to score beautifully. Now, you are positioned to start playing the sport. As mentioned earlier, there will be wonderful deal of updates that can need get every now and then. REPUBLIK365 are on a peer to look network. These updates can take a nevertheless. One things that all of us have discovered is that in case your computer is hardwired to the network, downloads would usually take couple of hours but We had arrived never in the position to finish the downloading of updates through wireless. Well-liked the time where in you will truly think really difficult as to what you really need to continue in the game, be it a spell caster, tank, a damage dealer, or alternatively a full support character. Calling it get with an a final decision, lessons also relation to your expertise in playing closing Fantasy XIV game.
Double/Triple Symbols: Whenever these symbols be found in GAME SLOT the center of a single payline slot in conjunction with other symbols creating an absolute combination, the payoff amount is doubled or tripled. Two or three of them same symbols increase the jackpot pay out.
There is advantage a number of SLOT GAME machines as the payouts are averagely set high comparable to the land based slots in Las vegas. There is an interesting thing that before playing for real money, one can possibly play higher than normal odds slot machine games for liberated to practice.
There are surely no hard and fast rules to win these slot games we can obviously increase your chances of winning. Before playing many of the slot games, you must set your win and loss limits in order to play safe. This must be achieved as it’ll help you to economise from your bankroll. Win limit is the particular amount that a gambler is prepared to lose in case if he loses sport. The player must immediately stop playing various other sites . he meets this define. On the other side, if a gamer is happy with the amount he has won much can stop playing the. However, it is very important to follow these limits as a way to maximize your bankroll for any future pastime.
Slots that exist in SLOT GAMING train stations and cafes are frequently programmed as hot slots. The attractive bright lights and the inviting sounds of the slot machines have this enticing effect to those who are eating to finish their foods quickly so as to play slot games today.
As you play a slot machine, money management is probably the most important factors may perhaps affect your success. If you might be able to manage your money wisely, are going to have better amount associated with which absolutely spend enjoying. You need comprehend when strengthen bets or decrease it at the most beneficial moment to make certain that you take pleasure in winning and playing at the same effort.
2) King Kong – the King Kong Slot also wins in the graphics section. While it does not have as tons of bonus games as Lord of the Rings, it is normally brilliant when the fearsome ape busts his way through one belonging to the reels when you have picked up a secure!
…
Now an individual able in order to the benchmark and personal computer is wanting to score beautifully. Now, you are positioned to start playing the sport. As mentioned earlier, there will be wonderful deal of updates that can need get every now and then. REPUBLIK365 are on a peer to look network. These updates can take a nevertheless. One things that all of us have discovered is that in case your computer is hardwired to the network, downloads would usually take couple of hours but We had arrived never in the position to finish the downloading of updates through wireless. Well-liked the time where in you will truly think really difficult as to what you really need to continue in the game, be it a spell caster, tank, a damage dealer, or alternatively a full support character. Calling it get with an a final decision, lessons also relation to your expertise in playing closing Fantasy XIV game.
Double/Triple Symbols: Whenever these symbols be found in GAME SLOT the center of a single payline slot in conjunction with other symbols creating an absolute combination, the payoff amount is doubled or tripled. Two or three of them same symbols increase the jackpot pay out.
There is advantage a number of SLOT GAME machines as the payouts are averagely set high comparable to the land based slots in Las vegas. There is an interesting thing that before playing for real money, one can possibly play higher than normal odds slot machine games for liberated to practice.
There are surely no hard and fast rules to win these slot games we can obviously increase your chances of winning. Before playing many of the slot games, you must set your win and loss limits in order to play safe. This must be achieved as it’ll help you to economise from your bankroll. Win limit is the particular amount that a gambler is prepared to lose in case if he loses sport. The player must immediately stop playing various other sites . he meets this define. On the other side, if a gamer is happy with the amount he has won much can stop playing the. However, it is very important to follow these limits as a way to maximize your bankroll for any future pastime.
Slots that exist in SLOT GAMING train stations and cafes are frequently programmed as hot slots. The attractive bright lights and the inviting sounds of the slot machines have this enticing effect to those who are eating to finish their foods quickly so as to play slot games today.
As you play a slot machine, money management is probably the most important factors may perhaps affect your success. If you might be able to manage your money wisely, are going to have better amount associated with which absolutely spend enjoying. You need comprehend when strengthen bets or decrease it at the most beneficial moment to make certain that you take pleasure in winning and playing at the same effort.
2) King Kong – the King Kong Slot also wins in the graphics section. While it does not have as tons of bonus games as Lord of the Rings, it is normally brilliant when the fearsome ape busts his way through one belonging to the reels when you have picked up a secure!
…
Here is an extra helpful tip. Casinos do not usually place two good performing machines next to each similar. So, when you observe that the slot that you’ll be playing with is not giving you the finest payouts, you very well may try transferring to device next going without. Chances are, that machine is a hot slot machine.
The slots are hosted by finest casinos online, so actual no compromise on the graphics along with the speed of access. Even slot little leaguer chooses starts off with 50,000 credits, enough to help you you sustain for several hours. What’s more, every time you SLOT GAMING get back to the site, the credits are recovered!
The rules and directions for the online SLOT GAME machines are exactly like in a land base casino. First it is decided to what amount of cash to get. After that, the decision about how many coins location bet with spin occur. With the online slot machines, one can opt between 1, 3 and next up to 9 paylines. It easy that higher paylines one bets on, the cash he spends, but additionally the associated with getting more are higher too. Last thing that comes is clicking the spin button. The noise of the spin can be heard just like like within a land based casino; a great fun and excitement against the comfort of home.
Fact: No. There are more losing combos than winning. Also, the appearance of highest winning combination occurs rarely ever. The smaller the payouts, more number of that time period those winning combos feel and look. And the larger the payout, the less number of that time period that combination is going o glance.
In the particular best machine, you must calculate what amount it will set you back you to play. Slot machines differ in one another. Some are efficient at give you more winnings than the others. That is why it is important for a person to know that are those absolutely let you obtain more net profit. One way pick which of this machines can the best ones perform with, always make comparisons on the different games a person have had and go back to the equipment that is able to your family with the finest amount of profit.
The first electromechanical slot version was invented in 1954. Soon there were other versions of slots that take a cent rate, therefore, cash advances wishing perform in the one-armed bandit is fast growing. Since then, both casino operators have started to use more slots brought up, accept checks, tickets, tokens, paper, for individuals in sport Slots become expensive. But after a bit thanks the casino to draw in new players have appeared a cent slot laptops. As https://site04.angkasa189.com/ of slots permitted to be put on line payments more coins, and many players can’t afford create such large bets, it was decided that the minimum value of coins in slot machines was up one GAME SLOT coin.
Free Spins Pays-Find video slot machines that offer bonus rounds where achievable participate a couple of free bonus spins. Usually, you can opt to look at the “see pays” menu on the video slot machine before you insert money. Typically, totally free whataburger coupons spins rounds on these machines offer up some huge wins, the refund policy is particularly true on the best selling stacked wilds machines offered by IGT, WMS Gaming and others. Attempt and play games that an individual to to get hold of a bonus without too much effort. For example, from how bonuses are done.
…
Lucky Charmer has an extra screen bonus feature that makes it fun to play. You will choose between 3 musical pipes and the charmer plays your choice if you can still reach the bonus on. africaninternationalnewsmagazine.com that rises out within the baskets are the one to ascertain your payouts. To be able to activate the feature round you will need to be capable hit the King Cobra at 3rd pay line.
Each site that bingo is played on will contain different coin denominations. The amount could be set at fifty cents or twenty cents that you could to be in the rounds and also the spins might five dollars each. These amounts could change with different sites and regulations. It will be crucial to try out a few websites notice which one is the easiest to exercise. All sites give information GAME ONLINE SLOT required be always help win the online. The more informed a player is, the greater likely which will play well and understand what she are using.
There does not SLOT ONLINE sure win strategy the actual game of chance like Roulette. By using roulette strategy that works does not guarantee shortly win. When things don’t turn in the way tend to be expected, you might lose off of your bets. You could end up losing every money. Therefore, don’t be in the online Roulette with the actual you cannot afford to lose.
Your choices have an important impact as part of your chances november 23. The Blackjack strategy chart offers players a connected with the best choices inside the games – choices possess supposed to raise their chances to attain. But even when making the best, most accurate choices in the overall game – a tremendous part of winning still involves lady luck. You can make the best choice, but if the dealer characteristics better luck then you – plus it really can lose. You can also make with regards to decisions, take in the amount lady luck is working for you you will win.
Something else to factor into your calculation the place much the perks and bonuses you’re getting back from the casino count. If you’re playing in a land-based casino where you’re getting free drinks while you play, a person definitely can subtract the associated with those drinks from you’re hourly set you back. (Or you will add the cost of those drinks to the value of the entertainment you’re receiving–it’s just a matter of perspective.) My recommendation is actually drink top-shelf liquor and premium beers in order to increase entertainment value you’re getting. A Heineken can cost $4 60 capsules costs in the restaurant. Drink two Heinekens an hour, and you’ve just lowered what it is you perform each hour from $75 to $68.
Another associated with winning is to know your limits. Know when stop. There are three ways on how you will stop. First, set a sum for your game on that day. Once the amount is consumed, conquer. Second, set a time deadline for your leisure break. Once your watch alarmed, reduce. Third, if you win, halt. And if you win, have your prize not in cash but in check. Don’t just stop. Abandon the machine and walk out the casino and head home. By this, you did not lose your own money. Returning again materials and try your good luck. Look for machines that offer higher jackpots, higher bonuses, and more spins. If there are newly opened casinos nearby, visit and play certainly there. For sure, they offer higher jackpots and bonuses and give extra prizes for promotion. Implement the same rules bank for an efficient play.
The traditional version out of which one game may be modified by simple changes to a little more interesting, and so as GAMING SLOT GACOR appeal of Checkers increased, different versions of that particular game came up. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
Slot machines are certainly one the attractions in gambling establishments. With these machines, the golfer need cease an expert to find. He does not should be used to strategies or math to deliver the odds in his favor. Slot machine games are played purely on luck and about anyone who is of legal age can get involved in it. Today, free slot machine game games play online and can also be accessed from just about any gaming websites in the internet. These games may be played with real money or just for fun without money found.
…
If you want to try out gambling without risking too much, have you thought to try likely to some among the older casinos that offer some free games within slot machines just anyone could sample playing in their establishments. Frequently ask in which fill up https://fan.rachel-levy.com/ , but that is it. You’re able play in their slot machines for no-cost!
If an individual short promptly anyway, speed bingo the one of things you ought to try available. Some people are addicted to online bingo but see it is difficult to find the time to play. If this is the case, speed bingo is a wonderful thing to get into. It is fit quantity amount of games suitable into a normal slot of time, increasing your chances of winning if are usually GAMING SLOT GACOR playing to get jackpot. When you may ability to monitor fewer cards at food with caffeine . time, such is situation with others in online game keeping your odds of of a victory better than or much less equal a few traditional bet on online attn :.
Don’t play online progressive slots on a small bankroll: Payouts on progressives considerably lower compared to regular slots. For the casual player, they are a poor choice to play, mainly because they consume your bankroll immediately.
If GAME ONLINE SLOT performed with choosing a casino, it is time to play. Slots are one of accomplish to play since there is no evaporation have complicated rules nor does it require techniques to win. In other words, a player will must depend on his good luck, if you find any.
Set a establish limit for betting for yourself whether you are on online slot as well as land casino. If you start winning then do not get too cloudy, simply make want to get or get addicted on it. If begins losing do not try it “one more time”.
If you plan to play, it is better to plan in advance and SLOT ONLINE know for sure how long you is playing so that you will give yourself a budget. You mustn’t be willing to waste a lot of money on this. It is a good form of recreation that can also earn for you some financial. However, losing a lot of money is definitely not advisable.
If you hit a wild Thor your winnings could be multiplied 6 times. Can provide you with make potential winnings reach $150,000. Then you can also click the gamble button to double or quadruple your wins.
…
Craps is some of the more complicated games for more. It offers a variety of bets and it possesses an etiquette all distinctive. Some novice gamblers will be intimidated by all the action at a craps cubical. Many don’t know the difference in the pass line and a don’t pass bet. People they know . not can be assured some bets might offend other players at the table, because superstition plays a large part in casino craps. Some players holding the dice think a don’t pass bet is a jinx, like it is a bet made directly against their very own bet.
The RNG generates range for each spin. How many corresponds towards the symbols on the Reel. Creating hundreds of Virtual stops on each reel although you see far fewer symbols. Has a to generate millions of combinations will be the reason that online slots can offer such large payouts, beeing the chances of hitting jackpots are extraordinary. You may see 15 reels and calculate the odds as 15 x 15 x 15 1:3,375. However, what do not have to see will be virtual stops, and you could be one hundred or more per baitcasting reel! At 100 per reel, might be 100 x 100 x 100, or likelihood of 1:1,000,000. Asked yourself how they finance those million pound payouts? Congratulations, you know!
DINA 189 can be a mis-leading game, the “pass line” bet, which wins in a new shooter who rolls a 7 or 11, loses on a 2, 3, or 12, and on any other number requires him to roll that number (his point) again before rolling a 7, has a good money payoff that delivers a 1.41% edge to the home. The single-roll bets are simply just ridiculous: an ‘any 7’ bet pays 4:1 and the house a whopping 16% bank.
Another regarding winning is always to know your limits. Know when to. There are three ways on GAMING SLOT GACOR how you will stop. First, set a quantity for your game that day. Once the amount is consumed, give up. Second, set a time deadline for your leisure opportunity. Once your watch alarmed, stop. Third, if you win, forestall. And if you win, have your prize not in cash however in check. Don’t just stop. Abandon the machine and fall out of the casino and head home. By this, you did not lose the necessary money. Come back again next occasion and try your fortune. Look for machines that offer higher jackpots, higher bonuses, and more spins. If there are newly opened casinos nearby, visit and play in that location. For sure, they offer higher jackpots and bonuses and afford extra prizes for ad. Implement the same rules bank for a first-class play.
This will help you play the correct of coins for the very best payout. Which machine offers better limits? Which machine offers better odds? Wish play any machine, use the machine that is best suitable you.
Fact: Number of years players would have experienced that quite usually a winning combo comes by, short of one correct symbolic representation GAME ONLINE SLOT . But in long run, it don’t ever suggests how the winning combination is throughout the corner. The just misses are only another random combination.
With if the process concerned about playing in smoky environments, playing in your house is a clear advantage. Plus, those of individuals that do enjoy smoking will skill to accomplish this without any flack from others. These days, many land casinos don’t allow smoking involving their poker rooms either. Statistically, many regular casino gamblers are heavy smokers, when it is any trouble for you, being at home will ensure a good environment you.
…
You must always know which machine or site ideal your video slot download. Video poker machines are of many kinds but you should particular of which is the best for shoppers. If you see that you are losing in regards to the machine a few time then change device and begin mastering the next one. Although it is a rapid thing to do, you will discover a fresh start again.
Slot machines are one of several attractions in casinos. Overall performance machines, the ball player need ‘t be an expert to acquire. He does not have SLOT ONLINE become good at strategies or math develop the odds in his favor. Slot machines are played purely on luck and simply about anyone who is of legal age can participate in it. Today, free slot machine games play online as well as could be accessed from just about any gaming websites in the web. These games may be played with real money or just for fun with pick up involved.
Casino games are quite popular. It depends on chance and luck. Another crucial thing is strategy. Applying DINA 189 by which to play the can sway be functional. There are several involving casino on-line games. One of the popular games SLOT CASINO offered by the online as well as the offline casinos is Live roulette.
An accessory for that, it features a flashing jackpot light which adds a pleasure. Probably the most thrilling feature of gear is it topped lets start on chrome slender. Nevertheless, the thrill does not end on this page. The machine has an inbuilt doubled bank that holds a saving section separately which accepts anyway 98% around the globe coins.
When playing online video poker machines you should always try to bet a great deal of coins. This is because many machines give an additional tip for playing the maximum bet with your pay odds increase. Just like the if GAME SLOT a piece of equipment has the capacity to pay 2 lines, the jackpot might 1000 coins for get started building links coin played but 2500 for purpose coin. By playing the actual number of coins you have a 500 coin bonus. You have to careful however because if it’s a buck.25 cent machine but has 10 paylines you are wagering $2.50 with every spin. Ensure you look at how many paylines have the machine so that you don’t spend more per spin than had been planning that will help.
#5: Your life can alternation in a minute. See #4. The only way your life can change at a game title like Roulette is by using everything you hold and bet it in one spin of your roulette proceed. In slots you can be playing the way you normally play and then boom – suddenly you’ve just won $200k.
The most effective slots in many cases are located inside the casino’s locations. Hot spots are where the hot slots include. When we say hot slots, those are the basic machines developed to be simple to wipe out. Hot slots are often located in areas such as the winning claims booths. Casinos place fortunately machines here to attract and to encourage customers to play more when they hear the happy cheers of those people who are lining up in the claims booth to manage to get their prizes once they play slot machines.
…
While just showing that like a part of art was originally our plan, once we played it a rare occasions we couldn’t get sufficient. Granted it’s nothing like the cd or anything, but the competitive nature and reminiscing about old times comes home instantly we all start playing the Tekken Skill Stop Slot Product. Heck, we even argue who had been better, but everyone knew I was at a league of my own engagement ring. Although yet beg to differ.
Carrera cars are miniature cars guided by a groove (or “slot”) in the track. Though most consider them to be toys useful only for entertainment person, Carrera cars can GAME SLOT additionally be used as kids learning toys.
If you might be a first time player of slots, appear to learn about the rules governing the game first. Researching through AGS9 and asking the staff of the casino with regards to their certain rules are extra efforts you should at least do if you want a better and fulfilling on the net game. In addition, try inquiring from the staff of the casino about any details you’re needing within your game. One of the most important things you should be asking are details on the payouts, giveaways, and add-ons. Do not hesitate to ask them as is just their job – to entertain and assist you as clients.
There is an advantage a number of SLOT GAME machines as the payouts are averagely set high comparable to the land based slots in Las vegas, nevada. There is an interesting thing that before playing for real money, one can possibly play higher than normal odds slot machine games for liberal to practice.
The users of this high performance PC can produce use on the 7.1 channel audio output bay means of the S/PDIF port. It has a built in Sub Woofer, and four speakers which have built in the 3D Stereo Enhanced Head unit.
Back in the good old days, my pals and I would personally head to the mall arcade area with a roll of quarters and play additional on the road Fighter challenge. For hours we would trip choosing different guys and who might have thought that 15 years later we’re still all hanging out together. So when I accidentally came down the street Fighter Skill Stop Video slot we just had for having one associated with those Antique Slot machine games SLOT GAMING for residence.
One question that gets asked all of the time may be the can I play Monopoly slots about the web? The answer is that you house the United States, cannot. Wagerworks makes on online version of your game. But, as of your date, the casinos have got powered by this software don’t accept US players. So, for now, you must visit a land based casino perform this game.
Slot machines are a somewhat less harmful way to take charge of methods much you lose and win. It a way wherein hand calculators play having a relaxed mind and don’t want to plot, plan, or guess. Here the luck takes surcharge. Well, almost!
…
If you’re a newbie in slot machines, don’t fret. Studying ways to play slots do n’t want too much instructions don’t forget. Basically, wiggling with slots is just about pushing buttons and pulling controls. It can be learned within a few re-writes. Being a new player, will have to know tips on how to place bets so you simply can enhance your spins and increase the thrill that you’ll need experience.
These slots are best tutor belonging to the game as the more one plays learns quickly the secret to success of the trade perform slots and win. The recognition of the internet casino has grown with the development of the free slot video. One never gets bored out off playing these games because with the excitement these games provide with an amusing feel. Most of the slot gamers learn the games soon after move on top of the paid portion of the online pai gow poker.
That is correct, understand read that right. You can now play online slots and also casino games anytime well-developed right on your desktop. No longer do you need to wait until your vacation rolls around, or know some lame excuse inform the boss so that you can get a week off to head over to a number one brick and mortar online casino.
What then are generating of roulette over slots and or vice versa? To begin with, let’s SLOT ONLINE together with the specifications. REPUBLIK 365 are simple and fast-paced games, but without any debate, slots is definitely faster and simpler than live. This game is also easier comprehend than roulette, and you are going to only have a few rounds to learn about which patterns win and which ones lose.
No appear denomination of slot machine you wish to play, from the penny and nickel slots all method up for the high roller machines, tend to be : GAME SLOT one thing that every slot player simply need to do before they sit down and insert their profit. Regardless of how casual a slot player you are, the benefits associated with this action can be significant. Seeking to is that it’ll only be priced at a little bit of as well as effort.
If you’re an avid player in poker. You should always keep abreast regarding developments help make the in favor of every company or slots. Therefore, we sensible that you will SLOT CASINO enjoy excellent we to be able to offer anyone. Who said that to win the jackpot, it is advisable to spend long periods of time? But it is able to be win it in one or two hours seconds, and now we simply do not have words, that is certainly very regular repairs.
Slot cars provide a magnificent teaching tool for physical science. Get kids regrowth how individuals accelerate, decelerate, and defy gravitational forces as they fly high on a high-banked curve. Why is one car faster than the other? Just are made to simulate real race cars so they will really drift to the track that they go while using curves. Lane changing are also included features that add into the fun. Carrera slot cars could even be used to enjoy a science fair project as an instance properties of your energy and physical science.
Players must battle Doctor Octopus and so placed in difficult occasions. Playing as the super-hero you must save the lives for this innocent victims before it’s totally move on too a spin. Players will face all common criminals within the comic book making it even more fun to take pleasure in. This action hero has special powers like climbing walls, shooting out his very own spider web and they can sense threat. He was bitten with radioactive spider and this is how he had become the popular super-hero Spiderman.
…
Everyone features favorite form of slot game, but there’s no need to limit yourself to be able to one. Try putting several coins in the bunch numerous games just to experiment of what is on the.
Of course, as is the max bet, the jackpot displayed on top of the bottom in the screen meets a high roller’s enthusiasm. The progressive jackpot starts form about $75,000 and is now as high as $2,200,000. The average jackpot is concerning GAME ONLINE SLOT $727,000 which a pretty good win.
If this is the case with a $2.00 buy in tourney and there are a bunch only six players, suggestions prize become $6.00 and 2nd place may be $3.00, particular person yourself the casino has swallowed the remaining $2.00, which is how they can make their dinero. The prize structure SLOT ONLINE is therefore determined the particular number of entrants as well as the cost of the entrance fee.
Slot machines are certainly one of the attractions in gambling dens. With these machines, the player need end an expert to woo. He does not end up being be good at strategies or math GAMING SLOT GACOR develop the odds in his favor. KOIN 555 are played purely on luck and only about anybody who is of legal age can play it. Today, free video slot games play online which enables it to be accessed from become the base any gaming websites in the internet. These games may be played with real money or just for fun with no money connected.
Here is usually a few tips for green house best online casino slot action. First, all of the aforementioned establishments give your first deposit bonus, so make sure you have a look. You need to read over the rules and regulations very carefully, because them less easier to build up than other things. This is just “Free” money that they are giving you, so don’t damage.
How perform online slots is manageable. It is only the technology behind slot machine games that is quiet difficult. Online slots have generally a greater payout is provided. Leaning the payoff table will help explain what you can possibly profit. The payout table will provides you with the idea with the items you demand to earn. Across and diagonal are typical mistakes winning combinations with online slots. Matching the different possible combinations will offer different possible payouts. It isn’t nearly as hard to comprehend as far too. A row of three cherries for instance will supply you with a set payout, that row maybe down and up or all around. The same row of 7’s might supply you with a higher payout or an extra spin.
A player must limit himself or herself when staking bets in a slot machine game. In fact, 1 set of muscles starts shed bets, end up being best to avoid. Also, the limit shouldn’t be above and beyond ten percent of the account credits for it’s safer to play this path. For instance, in case a player does have a thousand dollars on the account that has decided to risk hundred, then they she must stop playing the slot if the account remains with nine hundred. In it, a farmer loses beyond he or she brings in. Hence, it’s far better be practical and try playing nontoxic.
First, you need to consider how much you may play these games anytime and anywhere get. There is that comfort factor in that room that entices people to work online and commence playing. So long as you have your computer, an internet connection, credit score or debit card with you, an individual might be set and able to play. Substantial you are capable of doing this at the comforts of the home, in your hotel room while on business trips, and even during lunch hour at your spot of labor. You don’t have to be worried about people disturbing you or starting fights and dealing utilizing loud music search. It is like having one’s own VIP gaming room in the home or anywhere you may be in the market.
…
First, set yourself to play. Be specific to have currency. They do not receive vouchers in playing slots. Then, set what could to invest that day on that game. Whenever you consumed this amount, stop playing accessible back again next time period. Do not employ all your make the most just one sitting and setting. Next, set period and alarm. Once it rings, stop playing and go out from the casino. Another, tell yourself to abandon gear once won by you the slot tournament. Do not be so greedy believing that you want more advantages. However, if DINA 189 have benefit your roll bank, then you may still try other slot party games. Yes, do not think that machine an individual had won is sufficiently lucky to cause you to be win time and time again again. No, it will just use up all your and shortly lose a good deal more.
It extremely important that get self control and the discipline to adhere to your limit therefore you SLOT CASINO won’t much more money. Remember that playing slots is gambling and in gambling losing is not avoidable. Play only in an amount a person are prepared lose positive after losing you can convince yourself that experience paid quite a lot of money that provided you with extremely best entertainment you had. The majority of the players who don’t set this limit usually end on top of a associated with regrets because their livelihood is ruined as a result of drastic decrease of a slot machine game.
Try to travel to your favorite search engine and lookout for slot machine games open. You’ll be surprised at it requires search result of websites and pages where you can enjoy mafia wars to the fullest without risking just one single dollar. So for those out there who are going to try out this game but are afraid to lose hard-earned money, you absolutely try playing it the internet.
Do not trust anyone around. May think that hear people saying that the slots are right in front row possibly the last ones, don’t listen to anyone. You’ll have even hear that you can apply machines which provide out a lot of dough at certain point of the day or SLOT ONLINE night. Do not listen to any associated with those gossips. It truly is that being a player you should listen and trust your self online slots.
With a stopwatch, children can look at the time it takes their slot cars to take on the track and, in doing so, explore the actual shape associated with slot car affects its speed. Kids can learn how wind resistance and aerodynamics can develop a GAME SLOT vehicle go faster.
They online slot games have several pictures, from tigers to apples, bananas and cherries. When you all three you overcome. Many use RTG (Real Time Gaming) free of cost . one of your top software developers for the slots. These includes the download, a flash client and are mobile, perfect take your game anywhere you to help go. In addition there are Progressive slots, you may well win a life time jackpot an individual also only be forced to pay out several dollars, as with all gambling, your chances of winning the jackpot can be like winning a lottery, a lot of good, however it is fun. With to play as many coins which you’ve got to win the jackpot, the risk is higher and is using the spend.
The slot machines are even the most numerous machines any kind of Vegas casino. A typical casino usually has at least a dozen slot machines or just a slot machine lounge. Even convenience stores sometimes get their own slot machine games for quick bets. Though people seldom come in order to some casino just to play in the slots, this person liked the machines while delays for a vacant spot inside of the poker table or until their favorite casino game starts a new round. Statistics show a night of casino gambling does not end with no visit in the slot machines for most casino patrons.
…
If you are playing a progressive slot and your bankroll is just too short perform max coins, move down a coin size. As an alternative to playing the dollar progressive games, within the quarter progressive games. Prolonged as achievable play max coins, however land the jackpot on that game.
Another issue about GAME ONLINE SLOT is actually usually that the numbers of many options available for you. Over the internet, a associated with websites exist providing various slot games to its customers. Anyone have are not interested within a service of 1 particular website, you can still search for the next one in a question of minutes. Playing online slot machine game is also beneficial when you can have fun it if you want. Unlike casinos, you’ll need have to wait patiently until simple . machine comes available and vacated by prior player.
Lets say that you’re playing on a slots machine at stakes of $1.00 a rotation. Really therefore say hello to the slot machine with $20.00 and make an attempt to come by helping cover their anything over $25.00, as the quarter profit can do 70 percent of the time through numerical dispensation.
The traditional version SLOT ONLINE out of which one game might modified by simple changes to be a little more interesting, and as recognition of Checkers increased, different versions of it game showed up. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
Craps GAMING SLOT GACOR can also a mis-leading game, the “pass line” bet, which wins in your new shooter who rolls a 7 or 11, loses on the 2, 3, or 12, and on any other number requires him to roll that number (his point) again before rolling a 7, has an easy money payoff that offers a 1.41% edge to your property. The single-roll bets are equally ridiculous: an ‘any 7’ bet pays 4:1 offers the house a whopping 16% cutting tool.
The R4 cards as well used for storing music files of all kinds. You can use for you to listen to songs after downloading and storing them in your device. Again, ATM189 may use the cards to be careful about your favorite movies after downloading them on your device. Moreover, you can invariably use these phones browse various websites from where you can download all files.
Wasabi San is a 5-reel, 15 pay-line video slot machine with a Japanese dining theme. Wasabi San a exquisitely delicious world of “Sue Shi,” California hand rolls, sake, tuna makis, and salmon roes. A couple of Sushi Chef symbols on the pay-line create winning combos. Two symbols settle $5, three symbols benefit $200, four symbols fork out $2,000, several five Sushi Chef symbols pay out $7,500.
…
English Harbour Casino launched in ’97. One of the best online casino that present you another level of entertainment. Being one among the pioneer in online gambling is however responsibility. And English Harbour Casino always see with it that they give their players the games and experience that they deserve. An amazing sound clips and find graphics you should enjoy you favorite casino games regarding fuzz.
Playtech are inventing a convenient to use interface that pleases the ball player with its amazing graphics, sounds and simplicity. The game also having a “Options” feature where the ball player can change the sound, speed and “Auto-play” settings. https://iqgaming.org/ with the game centered in a gold mine where SLOT ONLINE the lot of treasures ought to be found.
Online Slots have been a good option for people today just make use of the internet to play. Lots of things appear and vanish so as with the video slot as they mentioned technology steps.
The casino gives away free play and deposit bonuses for one thing, to get you through the doors. Now don’t get me wrong, online casinos are thrilling and rewarding places to be, but do it without thinking and you’ll lose just about everything. The best tip for the casinos online is learning using free play effectively, no deposit bonuses should be used GAMING SLOT GACOR for training purposes.
First, you need to consider the truth you play these games anytime and anywhere well-built. There is that comfort factor in it that entices people to work online get started playing. Provided you have your computer, an internet connection, your credit or debit card with you, in order to set and ready to play. Indicates that you does this at the comforts of ones own home, in your hotel room while on business trips, and even during lunch time at your home of work out. You don’t have to be bothered about people disturbing you or getting into fights and dealing whilst loud music. It is like having your own private VIP gaming room at your home or anywhere you may be in the time.
If are usually playing a progressive slot and your bankroll is too short to play max coins, move down a coin size. Instead of playing the dollar progressive games, be in the quarter progressive games. Prolonged as you as may play max coins, you can do GAME ONLINE SLOT land the jackpot on that play.
Tip #1 Just significantly poker, you need know the overall game of video poker. There is several variant of video poker games, with each having the next set of winning card combinations. Is actually also a good idea to pay attention to whether a machine uses one 52-deck of cards or higher than a. The more cards there are, the less likely the player will obtain.
50 Lions Slot is really a 5-reels penny game, you can actually although the coins in this game are included in different denominations you can place a wager for the small sum of 1p.
…
Gambling online has costless gambling and practice games providing slots to keep things interesting. While you will most likely not earn bonuses or win anything extra when you play free online slots or conceivably for fun, you be capable of get better at the games. Sometimes, you understand that online slot providers will supply you with chances to win even more money by joining special memberships.
Everyone functions a favorite type of slot game, but there’s no need to limit yourself to one. Try putting several coins in the GAMING SLOT GACOR bunch of numerous games in order to experiment with what is on the.
The casino gives away free play and first time deposit bonuses for one thing, to give you through the doors. Now don’t get me wrong, online casinos are extreme fun and rewarding places to be, but do it without thinking and you’ll lose every. The best tip for the casinos online is learning making use of free play effectively, no deposit bonuses should be used for training purposes.
If you’re lucky enough to win on a youtube video slot machine, leave that machine. Don’t think that machine is the ‘lucky machine’ for the customer. It made you win once nonetheless will not let upon the next games with out a doubt. Remember that video poker machines are regulated by random number generator and this is electrically run. In every second, it changes the mix of symbols for a thousand times. Really of the time, the combinations are not in favor of . If you still have enough time or remaining balance in your allotted money, then maybe you can try the other slot turbines. Look for the slot machine game that offers high bonuses and high payouts but requiring fewer coins.
If your are performing play a progressive game, be specific play the utmost GAME ONLINE SLOT number of coins as a way to to meet the criteria the massive jackpot. If you play a compact amount, seek it . win an extensive amount, nevertheless, not the astronomical amount you may win that isn’t progressive mishaps.
Blackjack. Complete SLOT ONLINE idea of the game is to accumulate cards with point totals as near to twenty one. JAVA 189 should be done without looking over 21 whereas other cards are represented by their number.
Lucky Charmer has 2nd screen bonus feature overall fun to play. You will choose between 3 musical pipes and the charmer plays your choice if you are able to reach the bonus round. The object that rises out on the baskets will be the one uncover your earnings. To be able to activate the feature round due to be capable hit the King Cobra at 3rd pay brand.
The online slot machines come by using a random number generator that gets numbers randomly beneficial click across the spin button in the overall game. The numbers that are generated by this generator complement the position of the graphics over the reels. The is supposed to be about luck and if you’re able to reach the numbers, you is sure to emerge like a winner.
…
Black king pulsar skill stop machine is among the many slot machines, which is widely also suitable for the people of different ages. KAGURA189 was also refurbished inside of the factory. This had thoroughly tested in the factory along with it was sent to different stores purchase.
#5: Your lifetime can alteration in a minute. See #4. The only way your life can change at a personal game like Roulette is if you are taking everything you own and bet it 1 spin with the roulette tire. In slots you can be playing the way you normally play after that boom – suddenly you’ve just won $200k.
An accessory for that, it has a flashing jackpot light which adds a supplementary pleasure. Essentially the most thrilling feature of handy is it topped up with chrome bring. Nevertheless, the thrill does not end SLOT ONLINE listed here. The machine has an inbuilt doubled bank that rrs known for a saving section separately which accepts about 98% of the world coins.
There are many benefits in playing slots online. One, it entails lower cost. Two, you won’t need to drive yourself towards casinos and back condo. Three, there are legion great offers which may get enjoy practically in online on-line casinos. Upon signing up, new registrations may possess the ability to acquire freebies and sometime an original amount that you bankroll. Fourth, online slots are straightforward to play with. Spinning basically GAME SLOT a matter of a click of the mouse all the time. You can choose pay lines, adjust your bets, and funds out using only your computer mouse button.
Here are many tips exactly how to to calculate the cost per rotation. When you are developing the casino, you may use you phone so you simply can perform calculations. Even most basic mobile phone these days is along with a calculator tool. In calculating kitchens . per spin, you would be wise to multiply online game cost, greatest line, as well as the number of coin imagine. For example, anytime a game amount you $0.05 in 25 maximum lines, multiply $0.05 and 9 maximum lines times 1 coin bet. Signifies that that it has to cost you $0.45 per spin anyone are playing 9 maximum lines to obtain a nickel machine with one minimum coin bet. Well-liked one strategy which you may use to win at casino slot gadgets.
The internet is SLOT CASINO becoming more advanced every year. When this technology was introduced to the world, its functions were only limited for research, marketing, and electronic correspondence. Today, the internet can certainly used to play exciting games from internet casinos.
Try to travel your favorite search engine and find slot machine games release. You’ll be surprised at the number of search outcome of websites and pages that enable you to enjoy this activity to the fullest without risking a specific dollar. So for those out there who chooses to try out this game but are frightened to lose hard-earned money, you can try playing it on the website.
…
The last mentioned they can provide you could be the chance perform for free for an hour. They can give you some amount of bonus credits to depend on. If you lose them while in the hour your trial is over. If you end up winning in the hour you may find a way to maintain your winnings however with some very specific constraints. You will need to read guidelines and regulations very carefully regarding that. Each casino has its own set of rules generally speaking.
Under decided to do . mode you decide on coins of worth between 3.10 or 0.20. In regular mode once you win a spin your winnings can transferred to super meter at the top machine. You can continue from here or bank your winnings by playing in Collect control key.
The casino gives away free play and first time deposit bonuses for one thing, to provide you through the doors. Now don’t get me wrong, online casinos are very exciting and rewarding places to be, but do it without thinking and you’ll lose each phase. The best tip for the casinos online is learning making use of free play effectively, no deposit bonuses should provide for training purposes.
The traditional version of this occurence game might modified by simple changes to be a little more interesting, therefore as appeal of Checkers increased, different versions of those game showed up GAME ONLINE SLOT . Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
Understand why you are approaching a slot machine to begin with. Are you there purely for night-life? Will WAK 69 be OK your current products lose your own money? Or, are you playing because want to hit the big old lotto jackpot. Some machines have small frequent pay outs while others have more uncommon big jackpots.
English Harbour Casino launched in the late nineties. One of the best online casino that offer you you a completely new level of entertainment. Being one within the pioneer in online gambling is naturally responsibility. And English Harbour Casino always see going without running shoes that they give their players the games and experience that they deserve. Having an amazing sound clips and find graphics you may always enjoy you favorite casino games SLOT ONLINE with no fuzz.
Everyone features favorite regarding slot game, but you shouldn’t have to limit yourself to one. Try putting several coins within a bunch different games just to experiment details GAMING SLOT GACOR is out and about.
The value of jackpots on Bar X ranges primarily based on your stake level, but like care for version, the Bar X jackpot is triggered relatively often to be able to many other online video poker machines.
…
This new gaming device has virtually redefined madness of a slot machine. If you see it for your first time, you does not even suspect that it is often a slot machine in determine! Even its game play is many. While it is just like the traditional video slot in the sense it’s objective is to win by matching the symbols, the Star Trek slot machine plays a lot more a recreation.
Apart using the single payout line in front of the reels, many more than one pay lines, every pay line to do with a separate coin SLOT ONLINE played with. The symbols stopping on the particular pay line decides the win of a farmer. The common symbols are bars, cherries, double bars and sevens.
In the overall game you get what is called a Spider web feature. https://mylink.la/ikan189 of is activated as soon as the symbol appears on reels two and four even more walks . must attend SLOT CASINO the same time. Would be to the slot machine game goes wild and your changes to get high-payouts are doubled as a result of many pay line mixtures.
The slots are hosted by right casinos online, so there’s no compromise on the graphics and also the speed of access. Even slot the participant chooses commences with 50,000 credits, enough to aid you sustain for many. What’s more, every time you visit the site, the credits are renewed!
The advantage is where all these online casino making use of. Regardless of your chances GAME SLOT a victory, benefit of is precisely what will prevent the internet casino profitable over the years because the particular slightest modifications may possess a dramatic result on both possibilities for the win very well as the edge just about every given golf game.
Some rewards are larger, such as complimentary trips to a buffet or another restaurant at the casino. When the place a person playing at has a hotel, ads about them . get the lowest room rate (or at no charge nights). When you are a really high roller, could possibly get airfare or taxi to and from the casino.
A player just downloads the game and clicks the ‘tournament’ button each morning lobby of the online traditional casino. There are instructions to follow along with the player follows these. First, he registers and after that, the guy can see how far he is to the alpha dog. The entrance fee costs as low as $2 to $5 24 hours.
…
This article summarizes 10 popular online slot machines, including For the Reels Turn, Cleopatra’s Gold, Enchanted Garden, Ladies Nite, Pay Debris!, Princess Jewels, Red White and Win, The Reel Deal, Tomb Raider, and Thunderstruck.
You don’t only set your limits before the game, anyone should follow it. When you follow your limits, you will certainly go home with good profit for ladies loss which bearable in which you. So, if you have lost a number of times, then stop playing for the day and return to their office some other time perform. If you win at casino slot machines, then stop playing expertise may be reached your win restriction. Playing this will place you prior to other slot players who just play like there’s really no tomorrow until they do not have money placed.
There are already SLOT ONLINE a regarding existing mobile slots out there. But it is not wise to grab the first one one happens to put your practical. There are a few things you must know so down the road . maximize your mobile slot experience.
Mr. Robot – Are the reason for if you’re planning on using bots to try and boost in order to your system. If 4 slots are taken by bots and it’s a 12 slot server you’re only leaving 8 slots for real humans. Try to keep mylink.la/yolanda77 in shape to shedding weight bots you’re intending to use (if any).
From a nutshell, the R4 / R4i is merely card which enables of which you run multimedia files or game files on your DS. No editing from the system files is required; it is strictly a ‘soft mod’ that has no effect on your NDS in in any manner. You just insert the R4i / R4 card into the GAME SLOT, and the R4 / R4i software will jog.
Be apt to set reasonable goals. Supposing you’re prepared risk $200 on simple . slot or video poker game. It would be wishful thinking to wish to turn $200 into $10,000, but you’ll have a realistic chance to turn $200 into $250, that may be a 25% grow in a very short effort. Where else can you get 25% on your money and have fun doing this? But you must quit as soon as this goal is achieved. On the other half hand, deals to establish your $200 stake last 3 days hours, are 25-cent probably SLOT CASINO 5-cent gadget. Stop at the end of the pre-set time period, irrespective of whether you’re ahead or behind.
Casino games are favored. It depends on chance and luck. Another crucial thing is blueprint. Applying the right process to play online game can prove to be smart. There are several involving casino gaming applications. One of the popular games made available from the online as well as the offline casinos is Live roulette.
…
Since Acquired now spending some of my summers in Reno I decided that the smart money move were patronize the so-called local casinos that cater for the local population rather than the tourist casinos on the strip. The theory here being that the shrewd locals were receiving superior reward cards coupled with a better total deal when compared with stupid tourists who patronized the short period.
No, you don’t want a permit to purchase one from somewhere. These are novelty machines, not the major slots you play in Las Vegas. They do pay out jackpots, only the spare change a person inside discharges out. Casinos use tokens to control payouts and people that desire to break inside them. The tokens themselves have no value at all once SLOT CASINO right out the building. Anyone dumb enough to cash them in will obtain a free ride from the area police.
These slots are extremely best tutor on the game as more one plays learns quickly the secret of the trade to play slots and win. The popularity of the online casino has increased with the growth of the free slot adventures. One never gets bored out off playing these games because in the excitement these games provide with an amusing feel. Most of the slot gamers learn the games and then move onto the paid perhaps the online spots.
Third will be massive jackpots. Unless your playing at one of this really big casinos at Vegas, most slot machines will basically be connected to a small jackpot of several SLOT ONLINE thousand. Most online casinos will supply you with a dozen slot games with million dollar jackpots. Its the magic to become able to link individuals online slot players together through the net. So every spin on the web is a chance at winning a life changing credit report and score.
When playing online slot machines you ought to try to bet as often coins. In the mean time many machines give an additional tip for playing the maximum bet as well as your pay odds increase. Like the if a product has as a way to pay 2 lines, the jackpot might 1000 coins for a coin played but 2500 for house coin. By playing the number of coins you get a 500 coin bonus. You have to careful however because if it’s a usd.25 cent machine but has 10 paylines you are wagering $2.50 with every spin. Make sure that you look at how many paylines are stored on the machine so you do not spend more per spin than you’re planning to successfully.
Always remember that when nexregen.com play slots, you need to have full amount. That is why you should stay due to players who you think may annoy you may GAME SLOT . Annoying people will eventually cause distraction. Junk food sometimes cause you to having a wrong mood in the long run and screw increase clear mind. This is disadvantageous for somebody. So, it is advisable a person simply transfer a brand new machine interactions are many noisy or irritating people surrounding you so that it’s possible to win casino slot piece of equipment.
There are two involving slot cars, there could be the analog cars and fresh digital programs. The traditional or analog slot cars are people who you might remember through your younger business days. This is where it was one car per slot along with the car had to stay as they slot for the whole race.
…
It’s almost a dead giveaway here, except for your fact that the R4 DS comes in it’s own R4 DS Box. But you’ll understand that once you open the box, the contents of this box are indifferent to the M3 DS Simply, you’ll get replacing light blue colored keychain / carry case which comes with the M3 DS simply. A person receive everything you need, out of the box. This includes the R4 DS slot 1 cartridge, a USB microSD Reader / writer (and this actually allows which use your microSD like a USB Drive) as well as the keychain travel case and program CD.
The amount you be forced depends across the type of payout the device SLOT CASINO gives. https://worktos.com/ of obvious nickel machines and five dollar sytems. The choice of which type perform depends in order to. Of course, the bigger payout, larger fee. Free slot machine games play online, you won’t be impose a fee. These free slot machine games were made to familiarize the beginner or those who’ve not yet played different machine. Include enable your crooks to learn about the combinations as well as the payouts. Following a certain sample of period, little leaguer may already wager for sure money. For those who just for you to enjoy the rush and excitement brought about by slot machines. They can just play for free anytime besides. With the huge regarding free hands per hour online, they will never find you have no choices.
Playing free slots can be a great in order to get acquainted with the game title. Beginners are exposed to virtual slots wherein these people place virtual money location the machine to play mode. Purpose is basically to hit the winning combination or combinations. It really is primarily created for practice or demo xbox games. Today, online slots are a far cry from its early ancestors: the mechanical slot apparel. Whereas the mechanism belonging to the slot machines determines the outcome of sport in the past, at this point online slots are run by an opportunity called the random number generator. Free virtual pai gow poker operate training can actually be programs too.
There are three reasons you should prefer playing online; better deals of the casino to your own action, a lot more multi-million dollar jackpots and a lot more SLOT ONLINE tournaments.
Upon realizing that the machine is a first-rate slot, don’t place big bets up till now. You need to begin bankroll test first. Here are severa tips you simply should consider when carrying out a bankroll push GAME SLOT . If the machine is giving over 50% additional profit, then leave that machine and stop playing needed. Chances are, the spin costs you huge loss. If have anything near just as amount to 49% of the money and profits, could certainly stay and play with this machine again. That machine is almost certainly a good machine that will let you hit a colossal jackpot today.
The slots are hosted by interesting casinos online, so genuine effort no compromise on the graphics as well as the speed of access. Even slot you chooses gets underway with 50,000 credits, enough which will you sustain for many. What’s more, every time you get back the site, the credits are reconditioned!
One on the great reasons for playing via the internet is its simplicity for mechanics. It is not necessary to insert coins, push buttons, and pull represents. So that you can spin the reels to win the prize, it will only take a click within the mouse button to achieve that. If you want strengthen or lessen your bets or cash out the prize to increase to do is to still select the mouse.
…
Franken Cash is a 5-reel, 20 payline video slot all about a mad scientist in his “spare parts” laboratory. Includes released in September, 2007. Franken Cash accepts coins from $0.01 to $1.00, along with the maximum regarding coins may can bet per spin is 200. The maximum jackpot is 2,500 coins.
As and as the reel stops, it’s about time to check for people who have got any winning association. Generally the winning amount is shown in Sterling. If you have won something, you may click SLOT ONLINE in regards to the payout list. It is impossible to know what you will be winning as unpredictability is you need to name of the slot adventure. If you do not win, try playing an innovative game.
It is even suggested that you play always with the utmost bets. There are a some machines that require that you place a maximum bet so that you just will become eligible for about a jackpot. Should want getting good chance at winning the jackpot, be absolute to bet the particular every time you play provided which can afford it.
Don’t play online progressive slots on the small bankroll: Payouts on progressives significantly lower than on regular GAME ONLINE SLOT slot machines. For the casual player, effectively a poor choice to play, as they quite simply consume your bankroll right away.
GAMING SLOT GACOR Get realize your are familiar with the game in regards to the machine, is definitely very necessary for the fresh players. Members of the squad who are online maybe in land casinos should always maintain in mind that they get well versed with online game that nevertheless playing for the machines. Is actually always every player’s dream to win on a slot tools.
Well if you are a man or woman who basically to help have fascinating entirely will depend on luck, you may want to use the game of Slot Machines, Bingo, Keno and Lottery. In here, no matter what others tells you, there isn’t any way to affect the outcome of sport. Although welconnect.org are games of luck, players may as well use certain best regarding their strategy: may bet as several options as they possibly can.
Tip #1 The biggest is to ensure you know guidelines of twenty-one. It is always a good idea to have a strategy it is far more play chemin de fer. All winning systems are based on a basic strategy which involving statistically speaking, there exists only one best action a player can take for each from the possible hands he can receive versus each possible upcard the dealership may have.
…
You must always know which machine or site is best for your slot machine download. Slots are a lot of kinds but you should correct of the best idea for you. If you see that you are losing concerning the machine more than one time then change the equipment and start the next one. Although it is a rapid thing to do, you will find a fresh start again.
There are even slots that are hooked SLOT ONLINE up to and including main computer with several casinos giving the players as well money. These mega slots pay out huge payoffs and constantly worth a few plays with the aspiration that you will get exceptionally purchasing.
Progressive slot games means these games are attached to the other machines about the casino. Non-progressive means that the machines aren’t connected to each other. The implication is because the odds much more expensive even for the progressive organization.
Mu Mu World Skill Stop Slot machine can provide you a great gambling experience without the hustle and bustle of your casino. Perform even let your children play inside of this Antique Slot machine game without the worry of turning them into gamblers. With this machine also it also not scared of the children falling into bad company that will be encountered in an internet casino environment.
If euphoriababy.com intend to play, it ideal for to prepare yourself and be sure how long you is actually playing guarantee you GAME SLOT will provide yourself an inexpensive. You should stop willing down the sink a regarding money on this subject. It is a positive form of recreation that will also earn for you some earnings. However, losing a fortune is definitely not advisable.
Their tournament lobby should be considered jumping with action. 24/7 there is really a tournament coming about for all players. Every hour, VIP players receive a freeroll tournament to enter, which goes on around the hands of time. Special event tournaments and more are grounds for additional prize draws SLOT CASINO .
#6: Will not get stabbed in a dark alley by another slots music player. Ever been playing Blackjack late at night, tired properly little bit drunk, and “hit” must have “stood”? Yeah – that person beside you screaming in your ear is someone you don’t get from want to outside the casino afterward. Meanwhile in slots if hit the nudge button accidentally, utilizes next to you aren’t for you to care.
…
It is very easy start off playing and start winning. The contraptions do is search a good online casino that you would like to join that attributes ton of slot games that you like. After you find one, it would have been a two step process one which just start playing and getting.
Tip #3 As you advance as being a player, work out how to bluff. You must realise SLOT ONLINE the game well and bluff only once you feel secure that the other players will not call your bluff.
The best strategy for meeting this double-your-money challenge is to appear for one single pay line, two-coin machine with a modest jackpot and a pay table featuring a good range of medium sized prizes.
First, you have to consider the advantage that you can take advantage of these games anytime and anywhere need your name. There is that comfort factor inside that entices people appear online get started playing. For so long as you have your computer, an internet connection, credit score or debit card with you, in order to set and ready to play. Written documents you do this in the comforts of yours home, with your hotel room while on business trips, and even during lunch hour at your house of work out. You don’t have to be concerned about people disturbing you or starting fights and dealing utilizing loud melody. It is like having your own private VIP gaming room at your house . or anywhere you tend to be in the time.
Another way of winning might be to know your limits. Know when in order to. There are three ways on techniques to stop. First, set a measure for your game that day. Once the amount is consumed, give up. Second, set a time deadline for your leisure break. Once your watch alarmed, just stop. Third, if you win, treat. And if you win, have your prize not in cash however in check. Do https://hybridtuktuk.com/ stop. Abandon the machine and fall out of the casino and head home. By this, you did not lose your money. Come back again next occasion and try your lady luck. Look for machines that offer higher jackpots, higher bonuses, and more spins. If there are newly opened casinos nearby, visit and play presently there. For sure, they offer higher jackpots and bonuses allow extra prizes for ad. Implement the same rules for your self for GAME ONLINE SLOT a proper play.
Online slot games certainly fun choice for those that do not have a fantastic ofcash. Around the globe a relatively secure array. It is an effortless game that doesn’t require any technique or guesswork. There are not any “slot faces” like are generally poker faces GAMING SLOT GACOR .
First I would personally pick very best machine. Some slots anyone a good shot at meeting this challenge while other people are more probably going to steal overall money. The most important feature when selecting a machine is the pay area. Too many players are keen on a slot machine that is dangling the carrot of having a huge lottery jackpot. Others pick one simply because it is big and shiny and appearance enticing.
The RNG generates variety of for each spin. How many corresponds to your symbols with the Reel. Creating hundreds of Virtual stops on each reel even though you see far fewer symbols. Ready to generate millions of combinations is the reason that online slot machine games can offer such large payouts, just as the chances of hitting jackpots are strange. You may see 15 reels and calculate the odds as 15 x 15 x 15 1:3,375. However, what have to see the actual virtual stops, and may possibly lead to be 100 or more per fly fishing reel! At 100 per reel, might be 100 x 100 x 100, or chances of 1:1,000,000. Ever wondered how they finance those million pound payouts? Congratulations, you know!
…
Invite buddies when you play. End up being more wonderful. Besides, they will be make certain to remind you never to spend ones money. It is possible you type in the casino, look for the positive. Mental playing and winning attracts positive energy. Have fun because you are there to play and take joy in. Do not think merely of winning or maybe luck will elude that you.
You will also choose perform a machine that has lesser winning combinations to achieve during your spins. Lower the combinations, the good chances SLOT ONLINE of winning more salary. Although the jackpot amount is lesser, you will still win big would of these kinds of machines have better odds in prosperous.
Upon understanding that the machine is a wonderful slot, do not place big bets at this point. You need to execute bankroll test first. Read on for some tips you simply should consider when perfecting a SLOT CASINO bankroll demo. If the machine is giving over 50% or even more profit, then leave that machine as well as prevent playing by using it. Chances are, the spin will cost you it really is loss. When you have anything near replacing amount to 49% of one’s money and profits, you can do stay and play with that machine one more time. That machine is definitely a good machine that may let you hit a colossal jackpot now.
When tend to be playing inside bonus slots, you should know that less is more and you can expect the right thrill while playing the games. The free bonus slots are for folks who don’t worry towards line payment. There can be games that have 2 or more bonus capabilities. One of the three bonuses can be good although may not that good and you may not similar to it. To make without anything of these sort doesn’t happen, carbohydrates choose a that has just one bonus feature option that you like. Choosing bonus slot games with uninteresting bonus features will just waste your along with efforts in which you put into playing the sport.
There are even slots that are hooked up to and including main computer with several casinos supplying the players and also their money. These mega slots pay out huge payoffs and constantly worth a few plays with the expectation that GAME SLOT you will get exceptionally purchasing.
$5 Million Touchdown is often a 5-reel, 20 pay-line video slot from Vegas Tech about American football. It accepts coins from 1 cent to $10.00, along with the maximum connected with coins you actually can bet per spin is 20 ($200). Are usually 40 winning combinations, a jackpot of 500,000 coins, wilds (Referee), scatters (Scatter), 15 free spins, and a bonus video. To win the 15 free spins, you need to hit three or more Scatter significance. To activate the bonus round, you may to hit two Bonus symbols on a reels. Symbols include Referee, Scatter, Cheerleader, and Sportsmen.
For those who want to play but don’t have an idea yet how functions and they you can win from it, the online slot machines will thought about great help in. Through https://www.capcn.org/ , you will be able to familiarize yourself with the various games and styles, as well as the jackpot prizes, before you play far more game fiddling with real .
…
The R4 and R4i cards include wonderful features that can enhance your gaming platform. Both cards enhance use of various devices as you make utilization of them for just one thing as well as other. Them have the ability of storing all regarding game files including videos and music files. Foods high in protein slot in the cards in your game console and all of them to download games files online. Them also include features for transferring files and documents from one console to the other.
Both forms of Roulette have similar fun and excitement when playing them, but positive will soon lose a few different times faster in American Roulette than European version if luck is not at your side. Just why? It is due to the house edge for American Roulette is double SLOT ONLINE value of European move. The higher the house edge, the better advantage toward the casino, meaning that in the future online casino makes twofold profit featuring a American wheel than European wheel. Therefore, you need to choose to play at European wheel a number of Roulette consider advantage of smaller house edge on this version.
There isn’t a sure win strategy the actual game of chance like Live dealer roulette. By using roulette strategy that works GAMING SLOT GACOR does not guarantee completely win. When things don’t turn in the way an individual might be expected, you might lose on the majority of of your bets. www.picniconthesquare.com could end up losing your money. Therefore, don’t be in the online Roulette with the amount of money you can’t buy to fail.
Slot Car Racing – the game takes for you to the world of Formula 1 and thousand-horse power cars in your internet browser an individual race against other Formula 1 cars on a track that resembles the best selling Silverstone! We are what it requires to master an F1 car? Discover by practicing!
Manage your money, but take advantage of the chance for big pay-out odds. Set the target amount of income that you want to make during each of these session. During any session you could have ups and downs. By setting a target amount, you can have a better chance of walking away while you’re ahead. Most slot machines only make payments the jackpot when you play maximum coins. Confident that you play maximum coins every time, you’re doing not in order to hit the jackpot and find out that master not qualify. The payout rate of gear has the jackpot figured in, anyone are taking out it with every spin. Most machines everyone to distinct coin sizes: 5, 10, 25, 50, $1 or $5. Use the lowest coin size purchase while betting the maximum amount of coins.
A DS R4 / R4i card is a storage device that enables you to store and view data regarding example images, text files, videos, sound files or homebrew games. The R4 / R4i card bypasses the encryption during the Nintendo DS, enabling files to be run completely from a storage medium such as a Micro SD bankcard GAME ONLINE SLOT . Second generation flash cards since the R4 / R4i make regarding the DS game card slot (SLOT-1), instead from the GBA game card slot (SLOT-2), these easier the following.
The best strategy for meeting this double-your-money challenge is to appear for just a single pay line, two-coin machine with a modest jackpot and a pay table featuring a good range of medium sized prizes.
…
Lucky Charmer – This online slot is most common for good bonuses. When possible see an additional screen bonus feature. Tend to be 3 musical pipes, and also when you achieve bonus round, the charmer plays selection of. But, to activate the bonus round, you end up being able to strike the King Cobra at the 3rd pay-line.
Fruit machines are the most GAME ONLINE SLOT sought after form of entertainment in bars, casinos and pubs. Online gaming possibilities have made them the biggest game online too. Fruit machines are different types; from penny wagers to wagers in excess of 100 ‘tokens’. Another attraction is the free fruit machine furnished by certain internet casinos. You can play on these machines without concern with losing bankroll.
There is limited sure win strategy previously game of risk like Live. By using roulette strategy that works does not guarantee noticing win. When things don’t turn in the way you are expected, would like lose of many of your bets. Most likely end up losing all of your money. Therefore, don’t play in the online Roulette with the money you cannot afford to reduce.
Celtic Crown: Just means positivity . thought it couldn’t get any better. Lose yourself the actual charm and mystic of this Celtic Crown bonus video slot SLOT ONLINE machine. Free spins are triggered with 3 or more golden harps. The Princess feature is triggered when 2, 3 & 4 reels display the Princess symbol.
First, you have to consider the fact that you can take advantage of these games anytime and anywhere men and women. There is that comfort factor within that entices people pay a visit to online you should playing. Provided that you have your computer, an internet connection, your credit or debit card with you, an individual set and able to play. Written documents you can do this in the comforts of yours home, with your hotel room while on business trips, and even during lunch time at your place of function. You don’t have to be concerned about people disturbing you or engaging in GAMING SLOT GACOR fights and dealing along with loud rock music. It is like having your own private VIP gaming room in the house or anywhere you can be found in the global.
You can maximize your earning power and entertain yourself playing free Mega Joker slot. If you bet between one to ten coins in basic mode place work on your path to ten and use the maximize bet feature to go into super meter mode. Have enough time here, all credits possibly be stored in super multimeter. If you reach bet hundred a joker in the middle reel will award unknown win can be anything between hundred and 2000 credits. At bet 150 one or maybe jokers will let you have a mystery win of hundred to 2 thousand credits. There are randomly selected progressive jackpots which help you when you bet more to raise your chances of winning.
If mylink.la/rebelbet77vip want to try out gambling without risking too much, why not try going however for of the older casinos provide some free games inside their slot machines just which could experiment with playing regarding establishments. They are ask an individual fill up some information sheets, but that is it. Refund policy . play inside slot machines for f-r-e-e!
…
Slot land – This online casino slot is renowned for great attractive ambience, excellent odds and completely secured financial dealings. And, unlike other sites, but there’s more require you download any software. Discover play by having an initial deposit of a great deal $100. It includes multiple line slots like two pay-lines, four pay-lines, five-pay lines and eight-pay lines. Have got pretty good chances to winning money here.
The amount you need to pay depends concerning the type of payout the machine gives. Possibilities nickel machines and five dollar units. The choice of which type perform depends you. Of course, the bigger payout, the larger fee. For gratis slot machine games play online, you won’t be impose a fee. These free video slot games are intended to familiarize the beginner or those who have not yet played a precise machine. Include enable them to learn close to combinations along with the payouts. After a certain demo version period, little leaguer may already wager for real money. Regarding just for you to enjoy the fun brought about by video poker machines. They can just play for free anytime desire. With the huge involving free action online, they will never can’t SLOT ONLINE choices.
In a nutshell, the R4 / R4i is just a card which enables one to run multimedia files or game files on your DS. No editing of this system files is required; it is strictly a ‘soft mod’ that has no effect on your NDS in any manner. You just insert the R4i / R4 card into the GAME SLOT, and also the R4 / R4i software will run.
The slots are hosted by leading casinos online, so will take a very no compromise on the graphics and also the speed of access. Even slot the participant chooses commences with 50,000 credits, enough to help you sustain for hrs. What’s more, every time you return to the site, the credits are replaced!
JURAGAN 4D indicate that these games are associated with the other machines within the casino. Non-progressive means how the machines are not connected to each other. The implication could be odds tend to be more even for that progressive design.
Slot machine gaming SLOT CASINO is really a type of gambling, where money is undoubtedly the basic unit. Are able to either getting grow, or watch it fade away from your offer. It would bother that much if control of money are employed. However, playing the slots wouldn’t work you actually only have minimal choices.
If consideration to try gambling without risking too much, let’s you try going towards a of the older casinos present some free games within slot machines just anyone could try playing his or her establishments. Mentioned to someone else ask a person to fill up some information sheets, that is it. You obtain to play in their slot machines for easy!
Determine the amount money and time you can afford to get rid of on that setting. Before you enter the casino, set a plan for your practice. Set your time . Playing at slots definitely addictive can might not notice you already spent all income and time inside the casino.
…
One way of ensuring your high associated with winning big amounts of income is by choosing what machine the suits you. Customers type will be the straight slot machine game. It is sometimes called the non-progressive slot. This always pays winnings in accordance with a fixed payout plans. Note that mylink.la/ganesa189 pays with an identical amount normal basis when players hit a special symbol formula of.
When you are playing on bonus slots, you need to know that less is more and can perform expect and this thrill while playing the games. Will bonus slots are if anyone is who don’t worry towards the line agreed payment. There can be games that have 2 greater bonus features. One of the three bonuses can be good while may end that good and it is not like it. To make certain anything of this particular sort doesn’t happen, you can choose an activity that recently one bonus feature option that such as. Choosing bonus slot games with uninteresting bonus features will just waste your some efforts a person can put into playing the sport.
If you mean to play, it very best to prepare and be sure how long you will be going to playing SLOT CASINO because you may offer yourself finances. You should cease willing down the sink a regarding money for this. It is a high quality form of recreation that will also earn for you some cash. However, losing a fortune is certainly not advisable.
Cool Bananas High rollers $180+ Slot spins: – This is developed by Cryptologic and allows specific $189 revolves. This slot game is inspired by King Kong and the many types of food that she loves when the theme. To have an wins the jackpot for the maximum spin, he or she would get $200,000. If the player pairs the banana icon with the mighty monkey icon, these people win a prize. This is not open to players in USA.
You would be know which machine or site is best for your video slot download. Video poker machines are of countless kinds we should make certain of which is the best for yourself. If you see that you are losing on the machine hundreds time then change the device SLOT ONLINE and commence the next one. Although it is an unexpected thing to do, you will discover a new beginning again.
No, you do not have a permit to get one. These are novelty machines, not the major slots you play in Las Nevada. They do pay out jackpots, but only the spare change a person inside is developed. Casinos use tokens to control payouts individuals that desire to break in the individual. The tokens themselves have worth at all once away from building. Anyone dumb enough to cash them in will obtain a free ride from the local police.
One thing to remember is this kind of doesn’t GAME SLOT possess a pull lever on one side. It’s a more up up to date version of how slot machines are played today. Which means there are a couple of of you who enjoy the old classic versions, but we this way one much better. On the game you’ll find 7s, bells, cars with flames the actual back, wilds, watermelons, in addition to course cherries. Definitely enough to help you busy for quite a long time ago.
In online game you get what is called a Spider web feature. This kind of is activated as soon as the symbol appears on reels two and four obviously you can must be at the same time. If this happens the slot machine goes wild and your changes acquiring high-payouts are doubled because of the many pay line permutations.
…
As considering that the reel stops, it’s time to check if you have had got any winning grouping. Generally the winning amount is shown in Sterling. If you have won something, it is click round the payout workplace. It is impossible to know should really be winning as unpredictability is technique name of the slot game. If you do not win, try playing an innovative new game.
There undoubtedly number several manufactures. Essentially the most SLOT ONLINE popular ones are Scalextric, Carrera, AFX, Life Like, Revell and SCX. Sets for these makes discovered from hobby stores, large dept stores and online shopping sites including Amazon and ebay. Scalextric, Carrera and SCX have the widest connected with cars including analog and digital versions.
If you want to try out gambling without risking too much, you will want to GAMING SLOT GACOR try for you to some for the older casinos that offer some free games inside their slot machines just in which means you could test playing inside their establishments. Others ask an individual fill up some information sheets, but that is it. You’re able play in their slot machines for no cost of charge!
Bonus Added Slots: Features include multi-spins, 5 reels, multi-lines, bonus games, wild symbols, scatter pay, multiplier and nudge-hold. MISTERI BET77 at casinos and also land-based.
Don’t play online progressive slots on the small bankroll: Payouts on progressives hard lower GAME ONLINE SLOT than on regular pai gow poker. For the casual player, these a poor choice to play, as they quite simply consume your bankroll briskly.
BOOT SLOT 2 – This menu option allows the R4 DS, just like the M3 DS, to boot the GBA Slot, or Slot 2, in your Nintendo DS / Nintendo ds console. Through the those of us that also want to get fingers on a GBA Flash card, and wish to run GBA Homebrew games and applications as well as Nintendo ds. It also adds extra storage for NDS Homebrew, because you’ll be able to use a GBA Flash card besides NDS files, as long as you apply the R4 DS as a PASSME / PASSCARD alternative.
The second period of development with the slot machines was rather calm, fell in towards middle for this twentieth 1. The brightest event of the period was output of the Big Bertha. However, shortly made overtopped by even more killing innovation of period – Super Big Bertha.
Craps belonging to the of the greater complicated games to ascertain. It offers a variety of bets and comes with a etiquette all its own. Some novice gamblers will be intimidated by all the experience at a craps kitchen table. Many don’t be aware of the difference from a pass line and a don’t pass bet. May well not be aware some bets might offend other players at the table, because superstition plays a large part in craps. Some players holding the dice think a don’t pass bet is a jinx, although it is a bet made directly against their own bet.
…
The R4 and R4i cards come with wonderful features that can enhance your gaming procedure. Both cards enhance use different devices while you make use of them 1 thing as well as other. The cards have the capacity of storing all kinds of game files including videos and music files. You can slot on the cards in your game console and all of them to download games files online. Them also along with features for transferring files and documents from one console into the other.
When should you go for? Let’s face it, small wins will not keep you happy for too much. You’re there for major win, even so, if should you go GAME ONLINE SLOT for understand it? Wait until the progressive jackpot become hefty. Why go hard when the jackpot is small?
For beginners to slots, the regarding playing online may often be a daunting an individual. All too often, beginners are turned off at online slot games and don’t play just because they think that playing with real budget is required. The truth is that couple of different methods many choices to playing by going online. Playing with money is actually simply one of these businesses.
If you were only going to play with one coin or you wanted the same payout percentage no matter how many coins you played you would then want perform a multiplier slot fitness machine. Multiplier machines pay out a specific quantity of coins for certain symbols. This amount is multiplied together with number of coins idea. So, if three cherries pay 10 coins for almost any one coin bet, planning to pay 50 coins for a 5 coin bet. That GAMING SLOT GACOR machine doesn’t penalize you for not playing greatest number of coins authorised. There are no big jackpots in this type of machine. If you are searching to complete playing day out of cash then this is the machine for.
Slot cars also come in different designs. The smallest size is HO or 1:64 dimensions. Originally KUDA SAKTI 168 were made for inclusion with model railways and more so these little cars are generally fast and have now some amazing track designs. The next size up is 1:43 scale as well as it designed for the younger racer with many fun features and character cars. The 1:32 scale is which are coming out size car for racing at home and theres a wide associated with sets. Component size car is your 1:24 and is commonly found racing at slot car raceway memberships.
You shouldn’t have worry about anything about Super Slot Casino. They may be assuring all their players they will have essentially the most SLOT ONLINE secure and safe gaming in the web. So you can rest your head in being fair of their games. Relax, enjoy and aim for that huge jackpot that waits for successful.
Some with the common online bingo rooms in the united kingdom are: 888ladies, BlackpoolClub Bingo, Gala Bingo, Foxy Bingo, Ladbrokes Bingo, Jackpotjoy, Littlewoods Bingo, Paddy Power Bingo, Sky Bingo, Mecca Bingo, Wink Bingo and Virgin Bingo.
…
Silver Dollar Casino is giving the most range of games. Offering casino games like roulette, slots, video poker, and blackjack. An individual can play these games in their download version and by instant games.
There appears to be no real response to this question. When playing Blackjack get to decide when to be able to another card (HIT), when to stay for your cards (STAND), when to double your bet together with other choices, accessible to players amongst people.
Of course, as may be the max bet, the jackpot displayed using a bottom of your screen meets a high roller’s presumptions. The progressive jackpot starts form about $75,000 and has gone as high as $2,200,000. The average jackpot GAME ONLINE SLOT is about $727,000 along with that is a very good win.
Under most important mode does not matter . coins of benefit between 0.10 or 0.20. In regular mode when you win a spin your winnings always be transferred to super meter at the top of the machine. You can keep from here or bank your winnings by but additionally Collect device.
If ISTANA 189 plan to play, it is best to make plans and know for sure how long you seem playing because you can provide yourself a budget. You can’t afford to be prepared to waste SLOT ONLINE fantastic deal of money on this. In order to a good form of recreation and may also earn for you some dollars. However, losing a lot is no way advisable.
This makes it possible to play the right amount of coins for really best payout. Which machine offers better rules? Which machine offers better odds? Wish play any machine, GAMING SLOT GACOR participate in the machine with this increasing best designed to you.
Just an individual chose perform online slots for free doesn’t mean you are excluded from learning what any slots player learns. The tips, tools, facts, and any other useful information may need anyone decide to begin playing slots online are always made in order to you and also new internet poker players. When you begin playing slots online, considerably more an option on this particular which can offer you a chance to decide play for funds or for celebration.
…
If you wish to grant online slot machines a chance, then ensure that you place down a money maximum. Do not bet any cash that needed hold. You as well should not spend any borrowed finances! You should have a fair reason as to the reasons you would really like play slot games. Purchasing merely clear examples . a couple of minutes of fun, that’s alright. All of the Same, content articles wish to play as you would like to win a great deal, then perhaps you should take a pace back for a secong.
Be absolute to set reasonable goals. Supposing you’re SLOT CASINO in order to risk $200 on your favorite slot or video poker game. It might be wishful thinking to dream to turn $200 into $10,000, but you possess a realistic chance flip $200 into $250, consume 25% grow in a very short effort. Where else can mylink.la/roma99 get 25% on money and enjoyable doing who’s? But you must quit as soon as this goal is achieved. On the other half hand, deals to make your $200 stake last for three hours, play a 25-cent maybe 5-cent machine. Stop at the end of the pre-set time period, irrespective of whether you’re ahead or behind.
You should choose to play a machine that has lesser winning combinations to perform during your spins. Lower the combinations, the better chances of winning more money. Although the jackpot amount is lesser, you will still win big since the majority of these types of machines have better odds in profiting.
Free winning casino strategy #2 – The best game perform to win at the casino is none other then pontoon. When you take the time much more details card counting strategies pause to look for increase the chances of you winning at the casino more. Being able to predict the cards that the card dealer will pull gives SLOT ONLINE a better management of the contest.
Second, GAME SLOT you’ll need to select a way to finance your account and withdraw your earnings. Each online casino offers multiple approaches to accomplish this, so understand everything very carefully, and choose the option you think is excellent for your situation. The great thing about the step all of the process, is that often the payment option you select, will almost assuredly work for good other online casino make use of to enroll with.
No challenege show up denomination of slot machine you plan to play, through the penny and nickel slots all means up on the high roller machines, is definitely real one thing that every slot player simply have to do before they sit down and insert their financial. Regardless of how casual a slot player you are, the advantages of this action can be significant. One of the benefits is that it’s going to only financial impact a person a few minutes of period and.
Apart off of the single payout line ahead of the reels, lot more than a single pay lines, every pay line on the topic of a separate coin had fun with. The symbols stopping on the particular pay line decides the win of a farmer. The common symbols are bars, cherries, double bars and sevens.
…
Familiarize yourself with the rules of domains in some slot tournament than an individual playing by. Although the actual play become similar, the payout and re-buy systems may be varied. Some online slot tournaments will allow you to re-buy credits a person have have used your initial credits. Can be important comprehend if you are on the first choice board and expect to be paid released. Each tournament also decides the actual way it will determine the victorious. In some slot tournaments, the participant with probably the most credits at the end on the established time period wins. Other tournaments have a playoff along with a predetermined regarding finalists.
There is GAME ONLINE SLOT be no real be managed by this speculate. When playing Blackjack to be able to to decide when to be able to another card (HIT), when to stay with both cards (STAND), when to double your bet additional choices, given to players amongst players.
Slots are positioned up to encourage players to play more dollars SLOT ONLINE . It is clear to read the more coins one bets, the better the odds and the payouts are probably. Most machines allow you select the associated with the coin that seek it . play using. When the payout schedule pays at a higher rate for more coins, you might be better off playing smaller denominations and maximum gold and silver coins. This concept seems simple, but a lot of jackpots been recently lost by careless play the game.
The chances of winning the are based on luck simply no element can influence or predict the result of the video. Bingo games are played for fun, as no decisions need in order to made. However, there are some essential tips that supply better for you to win the game. Playing one card simultaneously is suggested and banging should be prevented while dabbing. A paper card with lower number should be selected. It has more regarding getting the numbers closer together. In Overall games, it is mandatory that you come out early to have the first set distributed. It is essential to be courteous and share the winning amount among the partners. Ideally, the odds of winning are when you play with fewer buyers. Some even record their games if they are trying out some special games. It isn’t difficult to pat.
If you are play a progressive game, be apt to play the actual number of coins maintain to are a candidate for the massive jackpot. If you play a compact amount, seek it . win a great amount, benefits GAMING SLOT GACOR the astronomical amount a person are win associated with progressive billiard.
Everyone does have a favorite form of slot game, but you shouldn’t have to limit yourself to be able to one. Try putting TW 88 in the bunch numerous games in order to experiment using the information is reading this blog.
If possibly lucky enough to win on a slot machine, leave that machine. Don’t think that machine is the ‘lucky machine’ for your. It made you win once even so it will not let you on the next games for certain. Remember that slots are regulated by random number generator and could electrically run. In every second, it changes the combination of symbols for 1,000 times. As well as most of the time, the combinations aren’t in favor of you’ll. If you still have the time or remaining balance in your allotted money, then maybe you can try the other slot turbines. Look for the slot machine game that offers high bonuses and high payouts but requiring fewer coins.
…
3) The amazing Spiderman – this is the one of those video pai gow poker that helps make the most of that film match. It has three features and This may also provide some seriously big wins because of the Marvel Hero Jackpot.
There are two kinds of slot cars, there will be the analog cars and the actual digital your. The traditional or analog slot cars are men and women that you might remember when using the younger a few days. This is where it was one car per slot and the car had to stay GAME SLOT given that slot to the race.
Real world games supply different time. However, the online games will be SLOT CASINO exciting to play. You can have a very good experience playing this connected with online game title. You can sit at the comfort of your home and love this exciting activity. But one thing you will miss, i’ve.e. the mood and the environment of the real world casino.
No, you do not need a permit to buy one. These are novelty machines, not the huge slots you play in Las Las vegas. They do pay out jackpots, but only the spare change place inside is developed. Casinos use tokens to control payouts and people that in order to break inside them. The tokens themselves have no value at all once outside the building. Anyone dumb enough to cash them in will obtain a free ride from region police.
The first electromechanical slot version was invented in 1954. Soon there were other versions of video poker machines that have a cent rate, therefore, variety wishing perform in the one-armed bandit is soaring. Since then, both casino operators have did start to use more slots brought up, accept checks, tickets, tokens, paper, for think in the sport Slots become expensive. But after quantities of thanks a new casino to draw new players have appeared a cent slot washers. As new versions of slots allowed to be put on the internet payments more coins, and the majority of players wasnt able to afford create such large bets, the decission was taken that minimal value of coins in slot machines was up one any amount of money.
Do not trust anyone around. Could possibly hear people saying that each one the slots are right in front row maybe the last ones, don’t listen to anyone. You’ll have even hear that there are machines offering out a lot of dough at certain point at the time or the night. Do not listen to any these gossips. It is simply that as being a player really listen and trust yourself online slot.
Blackjack or 21 concerning the easiest casino games to find out and listen to. The idea of the game is to a hand closer to 21 then an dealer. When playing Blackjack, regardless which of quite a few versions you could be playing, the overall game is between you and also the dealer nevertheless many players are from your table. Practice free, SLOT ONLINE the many versions of Blackjack and have the game you like best. Be successful determined your game chosen develop an approach you will utilize from a real money game. Might pocket some serious benefit this game and might be available in download and flash versions as well as Live Dealer On line casino.
Mainly medicine of playing online slot games is actually by have money, but on what? It’s just like you’re playing the game called Galaxy Balls. Solar panel systems need achieve is to place all food with caffeine . shapes or symbols within a row. mylink.la/srikandi189 know are opinionated on how to play this one, you are able to see a screen by using a row of special emblems. Sometimes, you can see this their form of shapes, fruits or even numbers from a 2-4 spinning wheels.
…
When you play slots, it is actually nice to a regarding helpful strategies. This is because having good strategies lets you november 23 big variety of profits. Slot machine game games are great games perform and are suitable for having a wonderful past-time. The game can be also more fun when just how increase your chances of winning.
A great game to play if rather than want to spend much cash except want to dip your toe into gambling is the slot cleaner. MAHA BET77 of these machines work by putting money into the slot, pulling a lever and then hoping a person get three identical photo files. If you do, you win, you actually don’t, should win. It’s rare to win big money the slot machines but is that possible have some luck winning small dimensions. You can also find slot machines that push money off a ledge.
In a nutshell, the R4 / R4i is simply a card which enables which run multimedia files or game files on your DS. No editing for this system files is required; it is strictly a ‘soft mod’ that does not affect your NDS in anyway. You just insert the R4i / R4 card in the GAME SLOT, as well as the R4 / R4i software will run.
Lucky Shot is a 5-reel, 20 pay-line video slot from Microgaming that only has a golf web. It accepts coins from 1 cent to 50 cents, and the maximum regarding coins that you may bet per spin is 200 ($100). There are 35 winning combinations, a number one jackpot of 15,000 coins, scatters (Gopher), up to 18 free spins, together with a Gopher Bonus Game. November 23 the 18 free spins, you SLOT CASINO should certainly hit three or more Golf Cart symbols. To activate the bonus round, you really should hit three or more Gopher symbols on the reels. Symbols include Gopher, Lucky Shot, Golf Club, Golf Bag, Trophy, and Golfers.
The bonus multiplier extremely similar on the multiplier machine except when engaging in the largest payout. To your bonus multiplier machine as soon as the jackpot is hit this maximum associated with coins played it pays a jackpot feature. So, the machine may pay out 1000 coins when the top symbols appear for one coin, 2000 for two coins and 10,000 for three coins when three coins is greatest.
It To become real finance. Don’t forget that even though your chips are found numbers on a screen, SLOT ONLINE it’s still REAL cost. This may sound a little silly, but sometimes people forget that and that is exactly how they end up losing big.
If you hit anywhere from around the equivalent money to 49% profit, then can perform play again with that same machine. Your odds of of getting the jackpot are greatly high as it might be a “hot slot”. For example, if you started spinning for $100 as well as have about $100-$149 as profit, action an indication that the slot a person playing is one challenge that has the best payment.
…
Before anything else, vegetables and fruit bring a hefty income with a person will. This is very risky particularly displayed within a public place, so protective measures must be exercised.
If you mean to play, it greatest to plan ahead and be positive about this how long you are going to playing make certain you will provide yourself an inexpensive. You should not willing to waste a GAME SLOT involving money on this subject. It is a form of recreation and may also earn for you some financial. However, losing a fortune is most certainly not advisable.
Determine just how much money and time 100 % possible afford get rid of on that setting. A person begin enter the casino, set a pay off your consideration. Set your time also. Playing at slots ‘s so addictive a person can might not notice you already spent all money and time inside the casino.
There may be times provided you can ride substantial stakes merely good. But what about those occasions when you can merely do with minimal table bets? Should you give up playing once and for all?
The best slot machines to win are in many cases SLOT ONLINE located near the winning claims booth. This is because the casinos would to help attract more players who will see would like an explanation lining up in the claims booth cheering and talking concerning their winnings.
If you hit anywhere from around the equivalent money to 49% profit, then discover play again with that same machine. Your chances of getting the jackpot are greatly high as it may be a “hot slot”. For example, if you started spinning for $100 may have about $100-$149 as profit, this an indication that the slot are generally playing SLOT CASINO are a few things that affords the best payout.
When playing online slots you should always try to bet the most coins. RAJAPLAY is because many machines give an added bonus for playing the maximum bet plus your pay odds increase. Including the if a piece of equipment has the capacity to pay 2 lines, the jackpot end up being 1000 coins for really coin played but 2500 for purpose coin. By playing the utmost number of coins you get a 500 coin bonus. You need to careful however because if it’s a buck.25 cent machine but has 10 paylines you are wagering $2.50 with every spin. You’ll want to look at how many paylines take presctiption the machine so you don’t spend more per spin than most likely planning which can.
…
A player just downloads the game and clicks the ‘tournament’ button inside the lobby with the online modern casino. There are instructions to follow along with the player follows these. First, he registers and after that, the guy can see the length of time he is always to the front runner. The entrance fee costs as little as $2 to $5 24 hours.
Playing free slots is often a great approach to get aware of the mission. Beginners are exposed to virtual casino wars wherein supply place virtual money place the machine to play mode. Purpose is basically to hit the winning combination or combinations. Every person primarily especially for practice or demo online. Today, online slots might be a far cry from its early ancestors: the mechanical slot machines. Whereas the mechanism for this slot machines determines in relation to of sport in the past, now online slots are run by a software called the random number generator. Free virtual pai gow poker operate training can actually be programs as well.
The first electromechanical slot version was invented in 1954. Soon there were other versions of GAME SLOT slot machines that take a cent rate, therefore, the quantity of wishing to play in the one-armed bandit is developing. Since then, https://mylink.la/hana189 have begun to use more slots brought up, accept checks, tickets, tokens, paper, for individuals tend in the game Slots become expensive. But after a bit of time thanks to be able to casino entice new players have appeared a cent slot washers. As new versions of slots allowed staying put on the internet payments more coins, while it will take players would not afford drugs such large bets, it was decided that minimal value of coins in slot machines was up one brass razoo.
This new gaming device has virtually redefined this is of a slot products. If you see it for the first time, you will not even suspect it can be a slot machine in clients! Even its hands per hour is completely different. While it is identical to the traditional slot machine in the sense the reason is objective SLOT CASINO would be to win by matching the symbols, the Star Trek slot machine plays similar to a blu-ray.
#1: They’re Simple. You should not sit there and stare at a technique card every 5 minutes, or be sure to try although up performing what cards had been dealt in a poor attempt at card loves to. You just spin the reels and hope find lucky. And in case you usually do not? You spin them again.
First, set yourself to play. Be sure to have cash. They do not receive vouchers in playing slots. Then, set a measure to sow in that day on that game. A person consumed this amount, stop playing and come back again next some time. Do not utilise all SLOT ONLINE your profit in just one sitting and setting. Next, set period and alarm. Once it rings, stop playing and proceed for from the casino. Another, tell yourself to abandon device once you win the slot tournament. Don’t be so greedy convinced that you want more victories. However, if you still have money in your roll bank, anyone then may still try other slot computer games. Yes, do not think that machine in had won is sufficiently fortunate to help you win repeatedly again. No, it will just dissipate all your and shortly lose a bit more.
If you are an avid player in wagering. You should always keep abreast most developments help make the right in favor in a company or slots. Therefore, we made a call that seeing enjoy this news we to be able to offer then you. Who said that to win the jackpot, you need to spend many decades? But it is able to be win it in a couple seconds, therefore we simply don’t words, it is very purchasing.
At these casinos they will either allow you to enter a zero cost mode, or give you bonus revolves. In the free mode they offer you a some free casino credits, which n’t have any cash increased value. What this allows you to do is within the various games that have the websites. Once you have played a online slot machine that you like the most you will be going to comfortable making use of once fruits and vegetables to play for hard cash.
…
Slot machine gaming can be a type of gambling, where money is always the basic unit. You’re able to either being grow, or watch it fade right out the your offer. It would bother that much if moderateness of money are employed. However, playing the slots wouldn’t work one does only have minimal wagers.
If you hit from the equivalent amount of money to 49% profit, then could certainly play again with exact same machine. Your odds of of having the jackpot are greatly high as it might be a “hot slot”. For example, if you began spinning for $100 as well as have about $100-$149 as profit, wishes an indication that the slot SLOT ONLINE you are playing is a that offers the best payment.
In the beginning, I really didn’t know what seem for, but this new little adventure not could prove costly than only Hanabi Full Screen Skill Stop Slot machine itself. You probably know how all leading Slot Machines are wired at the casino with under wires and everything else, acceptable? Well the good news is these currently set a whole lot be set up. All you have to do is plug it into a wall one would cash lamp possibly the vacuum you will see that sweeping.
In sport you get what is termed a Spider web feature. Is definitely activated as soon as the symbol appears on reels two and four and yes it even must be at the same time. When this happens the video slot goes wild and your changes acquiring high-payouts are doubled because of the many pay line merger.
Players GAME SLOT everywhere in the world will appreciate all of the awesome features that 3Dice offers their players, by way of the chat room, to the daily free tournaments for all players. Developing stop there because anyone play you’ll get rewarded with loyalty and benefits influenced by your VIP status.
There instantly sites where the chances of winning cash or prizes with points are greater when playing their slot machine game games 100 % free. Any player can implement these websites and have a good time.
Tomb Raider is a 5-reel, 15 pay-line bonus feature video slot from Microgaming. mylink.la/pararaja77 wilds, scatters, a Tomb Bonus Game, 10 free spins, 35 winning combinations, and SLOT CASINO a great jackpot of 7,500 loose change. Symbols on the reels include Lara Croft, Tiger, Gadget, Ace, King, Queen, Jack, and Ten.
If you want to grant online slot machines a chance, then make sure that you place down a money boundary. Do not bet any cash that steer clear of hold. You as well should not spend any borrowed wallets! You should have a fair reason as to why you would really like play slot games. An individual merely require a a handful of minutes of fun, that’s alright. All the Same, one does wish perform as enjoy to win a great deal, maybe you should take a pace back for per minute.
…
To dont master of poker you will need some time. In this case, again choosing a football analogy realizing what’s good not simply watch your favourite team play, but become its full member and get money for the concept.
Blackjack. Complete idea in the game is to SLOT ONLINE accumulate cards with point totals as near to 21 years old. It should be done without exceeding 21 and afterwards other cards are represented by their number.
There are three little screens on the inside slot machines which are named payout, credits, and bet. Payout refers into the player’s winnings; it is zero when there are the same as winnings. Credits refer to how many coins the gamer has left. The bet screen displays how much the player decided to bet.
In order to cash out your winnings, you will need to chalk up points by wagering on certain games, ie pai gow poker. It is possible to win up to $2,000 with $100 personal cash and $100 casino cash playing roulette and making use of certain GAME ONLINE SLOT promotions. I have done this.
OXIBET88 uncover offers all around the the Internet for playing various types of free slot games online for day-to-day money. What is there to grow in playing free slots? For most cases you get to keep any winnings over deals are going to money focus on by the casino. If you get lucky this could put hundreds, even many dollars GAMING SLOT GACOR to your pocket.
Slot machine gaming the kind of gambling, where money should be considered the basic unit. You may make it grow, or watch it fade from your hands. Always be bother much if small amounts of money could happen. However, playing the slots wouldn’t work should you only have minimal gamble.
With this exciting slot machine game you will discover several action game symbols as well as bonus features. Increasing your numerous places online where a person play this process packed video slot. During video game you may possibly three progressive jackpots the refund policy will be awarded aimlessly. This machine has three bonus features available and a max five thousand coins payout per average spin per pay the net.
…
Players must battle Doctor Octopus and they are generally placed in difficult occasions. Playing as the super-hero you must save the lives of your innocent victims before are able to move on too your future spin. Players will face all ordinary criminals for this comic book making it even more fulfilling to listen to. This action hero has special powers like climbing walls, shooting out her own spider web and they could sense possible. He was bitten the radioactive spider and this is how he had become the popular super-hero Spiderman.
The slots are even the most numerous machines any kind of Vegas land based casino. A typical casino usually has at least a dozen slot machines or also a slot machine lounge. Even convenience stores sometimes have their own own slot machine games for quick bets. Though people don’t usually come along with casino just to play at the slots, apply the machines while anticipating a vacant spot on the inside SLOT CASINO poker table or until their favorite casino game starts a new round. Statistics show in which a night of casino gambling does not end your visit in the slot machines for most casino clientele.
Progressive slot games indicate that these games are regarding the other machines to the casino. Non-progressive means that the machines are not connected to each other. The implication could be odds may even for the progressive design.
$5 Million Touchdown can be a 5-reel, 20 pay-line video slot from Vegas Tech about American football. It accepts coins from 1 cent to $10.00, along with the maximum quantity of coins that you can bet per spin is 20 ($200). SLOT ONLINE There are 40 winning combinations, a premier jackpot of 500,000 coins, wilds (Referee), scatters (Scatter), 15 free spins, and a bonus program. To win the 15 free spins, you need to hit three or more Scatter significance. To activate the bonus round, you may to hit two Bonus symbols on reels. Symbols include Referee, Scatter, Cheerleader, and Sportsmen.
Do not use your prize to play. To avoid this, have your prize under control. Casinos require cash in being. With check, you can get outside of temptation utilizing your prize up.
In a nutshell, the R4 / R4i is simply card which enables which run multimedia files or game files on your DS. No editing from the system files is required; it is strictly a ‘soft mod’ that does not affect your NDS in by any means. You just insert the R4i / R4 card into the GAME SLOT, as well as the R4 / R4i software will run.
mylink.la/kratonbet – This online casino slot is recognized for great attractive ambience, excellent odds and completely secured financial dealings. And, unlike other sites, that doesn’t require anyone to download any software. Carbohydrates play the initial deposit of almost $100. It has multiple line slots like two pay-lines, four pay-lines, five-pay lines and eight-pay lines. You have pretty good chances to winning money here.
…
Fact: Very little. There are more losing combos than winning. Also, the appearance of the maximum winning combination occurs almost. The smaller the payouts, more regarding times those winning combos appear. And also the larger the payout, the less connected with times that combination proceeding o appearance.
Black king pulsar skill stop machine is just one of the slot machines, which is widely also great for the people of different ages. This slot machine was also refurbished inside of the factory. SLOT ONLINE Made thoroughly tested in the factory after which it was sent to different stores available.
Real world games offer different time. However, the online games will be exciting to play. You can have an important experience playing this involving online sport. You can sit at your home and love this exciting activity. But one thing you will miss, when i.e. the mood and the environment of reality casino.
Here tend to be a few good data for choosing the best online casino slot action. First, all of all of these SLOT CASINO establishments produce a first deposit bonus, so make sure you try them out. You can read on the rules and regulations very carefully, because some of such are quite easy to collect than some others. This is just “Free” money they will are giving you, so don’t mess up.
Speaking of events, the Twin River RI casino is host to many events anytime. A 29,000 square foot event arena is often filled by some famous headline music artists. The center hosts excellent live entertainment and does very over the past year. HBO 9 of music and acting going on at Twin Rivers Cyber casino. Additionally, the facility is also available for banquets and special occasions like weddings and business conference calls.
The crucial thing to consider when good for your health to save is to strictly follow your slot bankroll wallet. Before sitting down in front of the machine, you have to first GAME SLOT create a certain amount of money. Decide on simply how much you are prepared risk in losing in conjunction with winning. Playing slots can definitely be luring. Winning one game will always seduce in which play a before visitor to your site it, each and every profit and the bankroll have ended.
To avoid losing big amount dollars at slots, you should set a financial budget for yourself before being. Once you have exhausted your budget for a session, you should leave the slot and move on to. There is no point in losing endless sum of money in a hope to win. In case you win, no one should use your winning credits to play more. Since chances of winning and losing are equal in slot machines, you cannot be guaranteed to win great deal more. Therefore, you can be happy in what you have won.
…
Win at slot machines #1: Casinos always would like to get their customers deeper to casinos its no wonder that playing the loose paying slot machines at the ends for the aisles are excellent areas to play. You can find winning slot machines in these areas!
Second, wish to o wedding attendents right traditional casino. Not all casinos are for everyone, such a person should decide which one excellent you. Moreover, every casino has a predetermined payout rate and should really figure out which payout is one of the most promising. Practically if you want to money in big stages of money, definitely choose the casino offering the best payout rate.
You should also choose to play a machine that has lesser winning combinations to perform during your spins. The lesser the combinations, the good chances of winning more cash flow. Although the jackpot amount is lesser, you will still win big since the majority of these types of machines have better odds in winning.
Slot cars provide a great teaching tool for physical science. Get kids promote how vehicles accelerate, decelerate, and defy gravitational forces as they fly on top of a high-banked curve. Why is one car faster rather than the other? Just are made to simulate real race cars so they actually drift all through the track as they quite simply GAME SLOT go from the curves. Lane changing and passing are included as well features that add to the fun. Carrera slot cars could be used to a science fair project to illustrate properties of your energy and physical science.
The more effective slots typically be located inside of the casino’s locations. Hot spots are where the hot slots are perhaps. When we say hot slots, including machines developed to be easy to destroy. Hot slots are often located in areas including winning claims booths. Casinos place more secure machines here to attract and to encourage people to play more when they hear the happy cheers of those who are lining up in the claims booth to obtain their prizes as long as they play slot machines.
At these casinos they will either help you enter an absolutely free mode, or give you bonus re-writes. In the free mode they offer you a some free casino credits, which don’t have any cash value. What this allows you to do is have fun playing the various games that SLOT ONLINE are on the resource site. Once you have played a online slot machine that you favor the most you will be going to comfortable making use of once it begins by consuming to play for funding.
#1: They’re Simple. mylink.la/republik365 should not sit there and stare at a strategy card every 5 minutes, or attempt to try SLOT CASINO although up using the information cards happen to be dealt from a poor attempt at card depending. You just spin the reels and hope obtain lucky. And in case you usually do not? You spin them again.
Break da Bank Again: Another revised slot machine with a revamped layout. Time to really crack the safe on the widely accepted slots game Break da Bank. The 5x multipliers combined associated with 15 free spin feature has the capability to payout a bundle of slot coins. 3 or safer scatters trigger the free spins.
…
Using two double-A batteries for solar lights and sound, this toy slot machine has coin returns for both jackpot and manual. The chrome tray as well as the spinning reels will a person to to feel like you have become at the casino. Place this slot machine bank any kind of room of one’s home for a real conversation piece.
A match bonus is money offered by an online casino to get you to attempt them presently there. They are generally larger for occasion depositors, but many online casinos have player loyalty workouts. The way a match bonus works is an online casino will match your deposit with casino financing. If the match bonus is 100% and you deposit $100 you get $200 in casino consumer. You will then would need to play a designated quantity plays a person begin can withdraw this some money. The number is usually rather low and easily obtainable. By taking advantage this kind of bonuses might actually a good advantage the actual years casino your past short execute.
A system that is not user-friendly can take all is often a fun out belonging to the game. Rather than just putting your body and mind into winning, you become torn between winning and finding out how to own the system. The best way to get with this in mind problem would be try first the free version of your games want to. This way, a bit more you sign-up, you exclusively what you’re getting to.
The main thing was that Experienced to buy something SLOT ONLINE he was developed to positively playing. Now mylink.la/royal189 wasn’t our own local casino, but this had similar into a lot of other Casino Slot Machines he strummed. The basic one, two, or three coins per spin, but release difference was this one didn’t have one of these kinds of pull-down levers on one side. It seemed a not much more up-to-speed using times despite the fact that it was refurbished on its own is.
If performing play a progressive game, be selected play greatest number of coins so as to qualify for your progressive goldmine. If you play a smaller amount, you will win GAME SLOT considerable amount, however, not the astronomical amount you can win an issue progressive collection.
An addition to that, the particular screen size flashing jackpot light which adds extra pleasure. Probably the most SLOT CASINO thrilling feature of the device is it topped with chrome eliminate. Nevertheless, the thrill does not end so now. The machine has an inbuilt doubled bank that contains saving section separately which accepts at the very 98% found on earth coins.
#6: You will not get stabbed in a dark alley by a fellow slots competition. Ever been playing Blackjack late at night, tired together little bit drunk, and “hit” the best time to have “stood”? Yeah – that person beside you screaming in your ear is someone minor want to meet outside the casino in the future. Meanwhile in slots if you hit the nudge button accidentally, individuals next you r aren’t going to care.
There are three main reasons you should prefer playing online; better deals via casino to ones action, many more multi-million dollar jackpots and much more tournaments.
…
Always play ‘maximum coins’. If you hit an excessive jackpot playing only 1 coin, the equipment will not open down the hole money for ! Usually playing BUNGA 189 is a pretty good strategy. On almost all slot machines the top jackpot is a lot bigger when playing maximum coins.
Red White and Win is a classic 3-reel, single pay-line progressive slot from Vegas Know-how. There are 13 winning combinations. Symbols on the reels include USA Flag, Bald Eagle, George Washington, Statue of Liberty, and Dollars.
Another tip is switching time security alarm. Set a time frame that you choose to play. If you’re reached the designated period and your watch alarms, then stop playing and return home. There are other more important things to perform than just playing. Besides, slots manufactured for recreation and not for formulating.
GAME ONLINE SLOT Celtic Crown: Just anyone thought it couldn’t get any better. Lose yourself in the charm and mystic of this Celtic Crown bonus video slot appliance. Free spins are triggered with 3 or maybe golden harps. The Princess feature is triggered when 2, 3 & 4 reels display the Princess symbol.
The online slot machines come along with a SLOT ONLINE random number generator that gets numbers randomly beneficial click across the spin button in video game. The numbers that are generated this particular generator complement the position of the graphics upon the reels. Recreation is facts about luck and if you are able to hit the numbers, you can actually emerge for a winner.
Major Millions is a 3 reel and three pay lines quit give you winnings amounting to $250,000. However the jackpot are available GAMING SLOT GACOR only one does bet $3 per spin and rewrite.
An ideal online slots strategy can be always to sign track of slot machine tournaments. These kinds of tournaments are really popular in recent years and you find them at both large also as small online casinos throughout the world. Believe it or not, merchandise online the in truth that each type of tournaments are fun, exciting and can help you land track of huge cash awards. You will not believe, dollars awards can be as high as $25,000 ( first place), $10,000 ( second place) and $5,000 ( third place).
…
Being an avid sports bettor and market enthusiast, I could not ignore the correlation that binary options has with gambling. In this particular form of trading an individual given two options pick from from: up or down. Is the particular security, currency, or commodity going to bring up or down the actual world respective time period that you have selected. Kind of like: the particular Patriots likely to win by 3 or? Is the score going regarding higher or lower than 43? You can see where this will probably right?
As and as GAME ONLINE SLOT the reel stops, it’s about time to check when you’ve got got any winning blended. Generally the winning amount is shown in Sterling. If you have won something, may very well click in regards to the payout computer. It is impossible to know what you will be winning as unpredictability is a large name within the slot task. If you do not win, try playing an innovative new game.
The Diamond Bonus Symbol pays the highest fixed Jackpot after the Lion token. The Diamond bonus is triggered whenever you land one of these bonus symbols on a pay-line.
Tip #3 As you advance as the player, know how to bluff. You need to realize the game well and bluff only when you feel secure that the other players will not call your bluff.
50 Lions Slot is a 5-reels penny game, because of this although the coins in this game may be found in different denominations you can put a wager for under 1p.
Familiarize yourself with the rules of obtain slot tournament than are generally playing within just. Although the actual play become similar, the payout and re-buy systems may stand out. Some online slot tournaments will everyone to re-buy credits a person have used your initial credits. Can be important to know if happen to be on the board and expect pertaining to being paid done. Each tournament also decides the way it will determine the winner. In some slot tournaments, the guitar player with the most credits at the SLOT ONLINE end of the established time period wins. STUDIO BET 78 possess a playoff using a predetermined connected with finalists.
3D Car Racing Game – this is one on the car games that anyone with a 3D first person perspective for your game, in contrast GAMING SLOT GACOR to most flash games which are presented in 2D birds eye outlook. The game features beautiful 3D graphics that will keep your race interest in order to maximum.
The traditional version of this occurence game may be modified by simple changes to be interesting, and consequently as attractiveness of Checkers increased, different versions of that particular game came up. Some of these variants are English draughts, Canadian checkers, Lasca, Cheskers and Anti-checkers.
…
Then watch as the various screens display to. The title screen will show the name of will give you and sometimes the coffee machine. The game screen will show you what program it functions. You need to look at certain aspects of that screen to determine how to play that particular machine.Also, getting will usually tell you ways high the Cherry and Bell Bonus go. Down the road . usually tell whether not really the cherries go to 12, 9, 6 or 3, likewise whether the bells go 7, 3 or a couple. The best ones to beat are those who cherry’s go to 3 and bells go to 2.These will take less a person to play and fewer money to conquer.
Slot machine gaming is often a type of gambling, where money is always the basic unit. Are able to either render it grow, or watch it fade far removed from your present. It would bother that much if it’s a good of money are gathered. However, playing the slots wouldn’t work one does GAME SLOT only have minimal trades.
A great game to play if tend not to want spend much money but want to dip your toe into gambling will be the slot navigator. Most of these machines work by putting money into the slot, pulling a lever and then hoping which you get three identical video. If you do, you win, one does don’t, you don’t win. It’s rare november 23 big cash on the pai gow poker but nicely have some luck winning small adds up. You can also find slot machines that push money off a space.
Apart off of FIONA77 to the front of the reels, many more than a single pay lines, every pay line referring to a separate coin had fun with. The symbols stopping on the particular pay line decides the win of a person SLOT ONLINE . The common symbols are bars, cherries, double bars and sevens.
Second, wish to o simply find the right gambling house. Not all casinos are for everyone, such in which you should select which one best you. Moreover, every casino has a fixed payout rate and vegetables and fruit figure out which payout is essentially the most promising. Practically if SLOT CASINO a lot to profit big amounts of money, you’ll need choose the casino that provides the best payout selling price.
Casinos place good machines in these places as they definitely want to attract more people to play spots. It is a fact that when passersby hear the happy cheers and victorious yelling of slot winners, others will be enticed perform so that they could also win at video poker machines.
A system that is not user-friendly get all enjoyable out belonging to the game. Rather than just putting your mind into winning, you become torn between winning and finding out how to manage the program. The best way to get surrounding this problem should be to try first the free version belonging to the games you want. This way, as soon as you sign-up, you understand specifically what you’re getting around.
Experience the exciting sounds of the casino in your own home while Crazy Diamonds machine standard bank. This is a replica on a larger scale featuring the real-life sounds of the casino and the jackpot light that flashes and the particular of a bank preserve your gold coins. By the way, this video slot will take 98% of coins made the worldwide.
…
Bingo-The bingo room has the capacity of accommodating 3,600 people. Typical bingo game is scheduled twice once daily. Apart from the regular game some large sums of money games like Money Machine, Money Wheel, Cars, Crazy L, and Crazy T etc just happens to be played. More affordable non- smoking sections where people with kids will have too.
#6: You won’t get stabbed in a dark alley by a fellow slots athlete. Ever been playing Blackjack late at night, tired as well as little bit drunk, and “hit” whenever you have “stood”? Yeah – that person beside you screaming with your ear is someone you do not want to meet outside the casino in the future. Meanwhile in slots a person don’t hit the nudge button accidentally, those next for you aren’t in order to be care.
It’s almost a dead giveaway here, except for the fact that the SLOT CASINO R4 DS comes in it’s own R4 DS Box. But you’ll discovered that once you open the box, the contents within the box are exactly the same to the M3 DS Simply, you get a similar light blue colored keychain / carry case which comes with the M3 DS simply. You get everything you need, out of the box. This includes the R4 DS slot 1 cartridge, a USB microSD Reader / writer (and this actually allows one to use your microSD being a USB Drive) as well as the keychain carry bag and software package CD.
In most of the casinos in your world, realizing slots are regularly located in near the entrances. Avoid these openings. Casinos do not place the good machines close to the entrances comes with will immobilize the people from going around the casino to play other applications. Also avoid the machines that are placed near tables for blackjack and texas hold’em. Usually, these are the worst systems. Casinos always see to it more secure machines aren’t placed here so that blackjack and poker players will not get distracted by noises that is brought about by cheering people and sounds coming out from the slots.
Knowledge for the SLOT ONLINE game is critical. Of course it’s exceedingly important that it is well known the basics of video game. You must have some idea on the foundational the answer to win. You need to know how these machines operate. Have you ever noticed how these machines produce good and perfect combinations located on the first and 2nd reels but fail provide a perfect one on the third? Well, this is primarily because these machines are programmed carried out. The slots have Random Number Generators that allow them to look for the outcome 1 spin. When you’ve got knowledge for the game, you would know there’s no exact timing among the spin because the are all random acts by the microprocessors specifically what drives the workout machine.
GAME SLOT The internet is starting to be advanced every year. When this technology was coming to the world, its functions were only limited for research, marketing, and electronic correspondence. MULIA 189 , the internet can now be used to play exciting games from online casinos.
Aside from being accessible, the video poker machines are pretty simple to perform. As I mentioned earlier, no special skill is suggested in activity. The game’s objective is to chance upon the winning combination — different combinations vary typically the amount of winnings. Usually, a combination is as quick as chancing upon three identical objects on the screen. Sometimes, even combinations which are not identical also amount to something. Hit the right combination and the player takes home the jackpot. This, of course, depends within system for the slot hosting server. A player just have to insert his money your past slot and press the button create the reels turn. Pai gow poker are casino gambling games that perhaps require probably the most number of wishful and hopeful consideration.
…
Generally, truly calculate value per spin so you actually can play in video poker machines in accordance to your budget. It is undoubtedly fun to play in a slot wherein you can have at least 10 moves. Learning how to look into a machine is method to boost profits.
Break da Bank Again: Another revised slot machine with a revamped SLOT ONLINE idea. Time to really crack healthy safely before summer on the popular slots game Break da Bank. The 5x multipliers combined this 15 free spin feature has the ability to payout a bundle of slot coins. 3 or more safe scatters trigger the free spins.
The first electromechanical slot version was invented in 1954. Soon there were other versions of pai gow poker that take a cent rate, therefore, the number wishing to play in the one-armed bandit is building. Since then, both casino operators have started to use more slots brought up, accept checks, tickets, tokens, paper, for numerous in the game Slots become expensive. But after a period of time thanks to casino appeal to new players have appeared a cent slot printers. As new versions of slots allowed in order to become put on the web payments more coins, plus some players did not afford different such large bets, it was decided that minimal value of coins in slot machines was up one SLOT CASINO dime.
Knowledge among the game is extremely important. Of course it’s exceedingly important that restrict the basics of the overall game. You must have some idea on the foundational the answer to win. You have to know how these machines operate. You may have noticed how these machines produce good and perfect combinations about the first and 2nd reels but fail provide you with a perfect one with the third? Well, this is primarily given that they machines are programmed to work on this. The slots have Random Number Generators that allow them to look for the outcome 1 spin. When you’ve got knowledge in the game, then you would know that there is no exact timing of this spin given that they are all random acts by the microprocessors the center of the tools.
The final type of slot is the bonus program. mylink.la/kuda189 were created to help add a component of fun in the slot machine process. Whenever a winning combination is played, the slot machine game will supply you with a short game a lot more places unrelated towards slot products. These short games normally require no additional bets, and help perk up the repetitive nature of slot machine game take part in.
There numerous GAME SLOT benefits in playing slots online. One, it is cheaper. Two, income need to operate yourself to the casinos and back property or home. Three, there a wide range of great offers which place enjoy in lot of online online casino. Upon signing up, new registrations may have the to acquire freebies and sometime a amount in which you bankroll. Fourth, online slots are very simple to spend playtime with. Spinning is just a few a mouse click all period. You can select pay lines, adjust your bets, and funds out using only your mouse button.
Online slot owners make available to you to the necessary terms. As it can be seen, all aspects are in your hands, you braver and go ahead to winning in deals are going to casino slot games! Online slots seem to becoming the craze proper. Everyone is scrambling to find the new site at a time best casino games on. Online slots actually find their roots in American culture. A man by the name of Charles Fey created the prototype regarding this game all approach back in 1887 in San Francisco, California.
…
So wouldso would you determine a gambling problem is ruining existence? What are from the the indicators that things are spiraling the particular control, that your life’s more truly becoming unmanageable?
Some rewards are larger, such as complimentary trips to a buffet SLOT ONLINE a further restaurant at the casino. In case the place you are playing at has a hotel, may think that get the best room rate (or at no charge nights). In https://mylink.la/key777vip are a really high roller, you might get airfare or shuttle service to and from the casino.
Flower Power – This machine SLOT CASINO is perfect for multiple pay-lines. It may offer only 1000 coins, but beauty of it may be the fact ‘less the coin figures, higher the winning chances’. And, are cheaper . multiple- pay-lines, so you need to lot of winning a combination. You will love it.
Slot machines were all the rage inside depression. In 1931, gambling was legalized in Nevada and slots found when you. When you walk into any casino today you observe row after row of slot machinery. They are so popular because they are simple to play and have large pay-out odds.
It’s really too bad I didn’t find the Hanabi Full Screen Skill Stop Slot Machine sooner, because at first I was searching for the Best Slots that dispersed money. Seriously, it didn’t even dawn on me that everything had switched over to the telltale electronic tickets until about three months once we started going. Just goes to show you how much he was winning. It’s nice to know that these Antique Slots give you tokens in order to that old time get it.
Playing free slots is a great approach to get aware of the game title. Beginners are exposed to virtual casino wars wherein process, which is place virtual money to put the machine to play mode. Intention is basically to hit the winning combination or combinations. Occasion primarily specifically for practice or demo programs. Today, online slots could be far cry from its early ancestors: the mechanical slot apparel. Whereas the mechanism of the slot machines determines the outcome of the in the past, currently online slots are run by a program called the random number generator. Free virtual slot machines operate functionality improvements programs too.
They online slot games have selection of pictures, from tigers to apples, bananas and cherries. When you all three you bring home. Many use RTG (Real Time Gaming) already one of the GAME SLOT top software developers for your slots. These includes the download, a flash client and are mobile, can perform take your game anywhere you need to go. There are also Progressive slots, you may well win the century jackpot and you only pay out several dollars, as with most gambling, the chances of you winning the jackpot is like winning a lottery, few good, however it is fun. Using to play as many coins you have to win the jackpot, the risk is higher and is using the purchase.
Cool Bananas High rollers $180+ Slot spins: – This may be developed by Cryptologic and allows particular $189 spins. This slot game is inspired by King Kong and the various types of food that she loves even though the theme. If someone else wins the jackpot for that maximum spin, he or she would get $200,000. If little leaguer pairs the banana icon with the mighty monkey icon, they’re able to win a prize. This is not open to players in USA.
…
Some rewards are larger, such as complimentary trips to a buffet some other restaurant at the casino. If your place you might be playing at has a hotel, you’d get the best room rate (or at no charge nights). If you’re a escalating roller, you might get airfare or shuttle service to and from the casino.
In recreation you get what is termed a Spider web feature. This kind of is activated as soon as the SLOT ONLINE symbol appears on reels two and four and yes it even must be at the same time. If you have the slot machine game goes wild and your changes to obtain high-payouts are doubled as a result of many pay line merger.
In outdated days when casino players actually knew what they were SLOT CASINO doing the unchallenged king of the casino tables were the crap platforms. This is where the term high-roller came everything from. If https://mylink.la/navibetvip knew what you were, doing this is where you hung out. A shrewd better can reduce the house edge to the small sum of 1.41% so that you can below 1% depending while on the house’s odds policy.
Second, need o wedding attendents right gambling shop. Not all casinos are for everyone, methods you must decide which the actual first is for someone. Moreover, every casino has an established payout rate and should figure out which payout is one of the most promising. Practically if wish to make the most big variety of money, ought to choose the casino that gives the best payout interest rate.
You will also choose to play a machine that has lesser winning combinations to perform during your spins. The lesser the combinations, the good chances of winning more investment. Although the jackpot amount is lesser, you will still win big since the majority of of these kind of machines have better odds in profiting GAME SLOT .
The Osbournes 5-reel, 20 payline video slot great award-winning tv series. It was released in September, two thousand and seven. The Osbournes accepts coins from $0.01 to $0.50, and also the maximum quantity of coins which you can bet per spin is 200. Websites jackpot is 15,000 dollars.
The important thing don’t forget when good for your health to save is to strictly follow your slot bankroll financial position. Before sitting down in front of the machine, you need to first create a certain expense plan. Decide on simply how much you are prepared risk in losing as well winning. Playing slots can really be encouraging. Winning one game will always seduce in which play as well as more before concerning it, all of your current profit together with bankroll are no longer.
…
No, abdominal muscles a permit to purchase one from somewhere. These are novelty machines, not the huge slots you play in Las Vegas. They do pay out jackpots, but only the spare change a person inside discharges out. Casinos use tokens to control payouts folks that desire to break within them. The tokens themselves have worth at all once away from building. Anyone dumb enough to cash them in will acquire a free ride from the local police.
Avoid machines which are placed beside a hot video slot. Most likely, these machines are cold slots because casinos do not usually place two good performing machines adjacent to every other.
GAME SLOT There aren’t any exact secret methods on how you can win in slot machines. However, there are some secrets on how increase the chances of you winning. One way to increase the likelihood of winning big quantity of prizes is find out how to choose a device which shows the best payment. These machines are usually installed in places near coffee shops, snack bars, winning claims booth, at the same time places best places see many more passing at.
Do not trust SUHU 189 . May think that hear people saying that every one of the slots are right in front row or possibly the last ones, do not listen to anyone. Completely even hear that there are machines offering out a handsome profit at certain point of the day or day time. Do not listen to any in the gossips. It truly is that as a player you ought to listen and trust yourself on online slots.
3) The amazing Spiderman – this but another one of the people SLOT CASINO video video poker machines that communicates the most of the film match. It has three features and And also really tone provide some seriously big wins due to Marvel Hero Jackpot.
Slot machines are the best favorite spots in the casinos. The combination’s shown on the reels make the adrenaline of both player and watchers surge bigger. It gives a good feeling being thrilled and satisfied especially if little leaguer wins the jackpot. These days, winning at pai gow poker is not brought by mere luck but by extra effort exerted by the player. Indeed, lucky charms are not really much effective at slot machine. If you are a slot player, you will need strategies obtain more in contrast to the fun.
It is very important that anyone might have self control and the discipline to keep to your limit and that means you SLOT ONLINE won’t much more money. Remember that playing slots is gambling and in gambling losing is not avoidable. Play only in an amount which you are for you to lose so that after losing you can convince yourself that own paid quite a lot of money that provided you with the best entertainment you ever had. Most of the players that do not set this limit usually end lets start on a regarding regrets since their livelihood is ruined as a result of drastic decrease of a slot machine game.
Once clicking the button for the bonus, an incentive wheel possibly pop on your window. You will notice that it says Loot and RP. The RP can stand for Reward Zones. This means that when you spin the wheel, you may land on special bonus loot a person may get some reward points as your special bonus.
…
Craps with the of outside complicated games to grow. It offers a number of bets and has an etiquette its own. mylink.la/mediabola78 will be intimidated by all the action at a craps table. Many don’t be aware of difference in the pass line and a don’t pass bet. They may not be sure that some bets might offend other players at the table, because superstition plays a large number in online casino craps. Some players holding the dice think a don’t pass bet is really a jinx, while it is a bet made directly against their own bet.
Fortune Cookie is a 3-reel, single pay-line slot machine that does have a Chinese fortune cookie plan. Fortune Cookie accepts coins from $0.25 to $25.00, and optimum number of coins that you can bet per spin is 2. Highest GAME ONLINE SLOT jackpot is 1600 loose change. This slots game is ideal for the beginner.
If had been only likely to play with one coin or you wanted the same payout percentage no matter how many coins you played you would want to play a multiplier slot cleaner. Multiplier machines pay out a certain quantity of coins for certain symbols. This amount might be multiplied your number of coins put money on. So, if three cherries pay 10 coins for a one coin bet, planning to pay 50 coins on your 5 coin bet. That machine doesn’t penalize you for not playing highest number of coins acceptable. There are no big jackpots in this particular type of machine. If you need to maximum benefit playing day trip of income then here is the machine in which you.
SLOT ONLINE In the initial 90’s, way before online casinos were prevalent, I enjoyed a great game of Roulette at one of my favorite land casinos three or four times a time. These days, I am even ought to leave the comforts of my house to get on main action.
There are a variety of online websites that allow a user to play free GAMING SLOT GACOR slot machine games. Some focus solely on slots and other gambling games such as blackjack and poker. Produce include ez slots casino, slots mamma and Vegas casino. Other websites offer slot machine play in addition to some other typical online games such as puzzle games; arcade games and word games.
Pluses: as every non-complicated casino slot, it offers reasonable but steady winnings, so is actually because a nice choice for your players who don’t like to exit without a win. One more thing I find nice that this mini keyboard has a involving countryside symbols and achievable forget about the strains city life when playing Hurdy Gurdy slots. And I almost forgot to mention: it is vital one within the few casino games usually do not require to design a winning symbol on the payline november 23. Some non-winning combinations comprised of 3 and much more symbols likewise bring you some singing coins.
Slot Car Racing – the game takes for you to the involving Formula 1 and thousand-horse power cars in your online browser anyone race against other Formula 1 cars on a track that resembles the favored Silverstone! Do you got what it will take to master an F1 car? Discover by actively!
Of course, as is the max bet, the jackpot displayed on the bottom belonging to the screen meets a high roller’s expected results .. The progressive jackpot starts form about $75,000 and moved as high as $2,200,000. The average jackpot is about $727,000 will be a pretty good win.
…
Second, you’ll need to choose a way to invest in your account and withdraw your earnings. Each online casino offers multiple to be able to accomplish this, so read over everything very carefully, and select the option you think is good to your location. The great thing this step within process, undeniable fact that the payment option you select, will almost assuredly work for good other online casino running, exercising to join the system.
They online slot games have numerous pictures, from tigers to apples, bananas and cherries. When a person receive all three you suceed in. Many use RTG (Real Time Gaming) as things are one with the top software developers for your slots. These includes the download, a flash client and are mobile, foods high in protein take your game anywhere you to help go. There’s also Progressive slots, you can actually SLOT ONLINE win the century jackpot and only pay out several dollars, as with all gambling, your chances of winning the jackpot comparable winning a lottery, not the case good, but it is fun. Using to play as many coins need to win the jackpot, the risk is higher and is proshape rx safe the purchase.
In outdated days when casino players actually knew what have been doing the unchallenged king of the casino tables were the crap corner desks. OVER BOLA is where the term high-roller came by way of. If you knew what you were, doing this is when you hung out. A shrewd better can reduce the house edge to under 1.41% GAME SLOT and just below 1% depending close to house’s odds policy.
Lucky Shot is a 5-reel, 20 pay-line video slot from Microgaming that has a golf notion. It accepts coins from 1 cent to 50 cents, as well as the maximum regarding coins which you can SLOT CASINO bet per spin is 200 ($100). There are 35 winning combinations, a highly regarded jackpot of 15,000 coins, scatters (Gopher), up to 18 free spins, along with a Gopher Bonus Game. To win the 18 free spins, you need to hit three or more Golf Cart symbols. To activate the bonus round, you would be wise to hit three or more Gopher symbols on the reels. Symbols include Gopher, Lucky Shot, Golf Club, Golf Bag, Trophy, and Golfers.
A player just downloads the game and clicks the ‘tournament’ button the actual world lobby in the online casino. There are instructions to follow and the player follows these. First, he registers and after that, he could see what distance he is actually the creator. The entrance fee costs as little as $2 to $5 each and every day.
Save your change in this particular 8.5 inch tall machine bank sign in forums be amazed at how quickly the money will increase. The real working handle and a coin return that can be operated manually make slideshow perfect idea for a souvenir.
So what’s the slot machine tip that’ll make you a winner? Stop being greedy! Before you put your money at risk, think about what you would like to achieve, besides having excitement. Do you want to play for a clear number of hours, or do you want to win a specific dollar amount, or a combination of both?
Slot land – This online casino slot is renowned for great attractive ambience, excellent odds and completely secured financial ventures. And, unlike other sites, it will not require to be able to download any software. May get play through having an initial deposit of anywhere up to $100. It provides multiple line slots like two pay-lines, four pay-lines, five-pay lines and eight-pay lines. You’ve got pretty good chances to winning money here.
…
Use your mouse – Use your mouse and press the button to get the reels spinning. The reels will not spin without your push in correct direction, so go ahead and push the button in the software.
Do not play that isn’t slot machines that are near towards table internet poker players. The machines that surround these are said regarding the least paying products GAME ONLINE SLOT . The casino executives do not keep high paying machines surrounding the table players because there is a chance of table players getting attracted towards men and women.
You would like a computer being more than 300 big ones. You need a gentle access to the Internet. https://mylink.la/dina189vip are a lifelong gambling bank the size of 500 big stakes or even so called sessional one the size 200-300 big stakes. I won’t go into detail – to having 100 dollars will be more than enough, also, having opened a forex account on-line, appropriate size tire that these get an additional tip from fifty to one hundred dollars usually. It will enough to start with.
When the gambling was banned, variety of the slots was changed. The sums of the prizes were replaced along with pictures in the chewing gum packages, as well as other tastes were depicted like a respective fruity. The amounts of jackpot was also increasing combined with the rise in popularity of the machines. In order enhance jackpots additional reels were built into the machines. The slots got larger and their SLOT ONLINE internal design was change regularly.
As and if the reel stops, it’s time to check in case you have got any winning appliance. Generally the winning amount is shown in Sterling. If you have won something, could click GAMING SLOT GACOR around the payout office. It is impossible to know what you can be winning as unpredictability is confidence is also name with the slot task. If you do not win, try playing an innovative new game.
In order to win the major jackpot unique would ought to place the actual bet down and make perfectly sure that all five Arabian man symbols be submitted to the one line. Here is the only manner in which a player can win the most amount money.
Set a restriction for betting for yourself whether happen to be on online slot perhaps land traditional casino. If you start winning then do not get too cloudy, you need to want drop or get addicted to barefoot. If you start losing don’t try it “one more time”.
…
There isn’t sure win strategy the actual world game of risk like Live roulette. By using roulette strategy that works does not guarantee noticing win. When things don’t turn into the way you are expected, may possibly possibly lose of all of your bets. You may end up losing every money. Therefore, don’t play in the online Roulette with the bucks you can’t afford to lessen.
Slot machine gaming is a gambling, where money is the basic unit. Determine make it grow, or watch it fade out of your hands. Might bother much SLOT ONLINE if small amounts of money are involved. However, playing the slots wouldn’t work an individual only have minimal gambles.
ARMOR BET78 can provide you could be the chance to play for free for sixty minutes. They offers you a specialized amount of bonus credits to bring into play. If you lose them inside of hour any trial is expired. If you finish up winning in the hour you’ll need may give you the option to maintain your winnings though some very specific policies. You will need to read guidelines and regulations very carefully regarding doing this. Each casino has its own associated with rules typically.
Once you’ve turned on this Nintendo DS or Ds lite lite, the equipment files will load away from the R4 DS cartridge, the same they do when utilizing the M3 DS Simply. It takes about 2 seconds for cause menu to appear, with the R4 DS logo on top screen, along with the menu GAME ONLINE SLOT on the bottom. On the bottom screen you can come up one of 3 options.
Your choices have a real impact in the chances to win. The Blackjack strategy chart offers players a list of the best choices inside of the games – choices usually are supposed to increase their chances to succeed. But even when making the best, most accurate choices in sport – an immediate part of winning still involves beginners luck. You can make the best choice, if the dealer is known for a better luck then you – you lose. You could also make with regards to decisions, simply by lady luck is in your corner you will win.
There is not an sure win strategy inside the game of risk like Roulette. By using roulette strategy functions does not guarantee a person win. When things don’t turn in the way happen to be expected, could possibly lose off of your bets. You may end up losing complete money. Therefore, don’t have fun playing the online Roulette with the amount of money you do not want to burn off.
In order to spend your winnings, you need to chalk up points by wagering on certain games, ie slots. It is possible to win up to $2,000 with $100 personal cash and $100 casino cash playing roulette and using certain strategy GAMING SLOT GACOR . I have done this.
Slot cars also come in different designs. The smallest size is HO or 1:64 range. Originally they were made for inclusion with model railways and more so these little cars are particularly fast and i have some amazing track templates. The next size up is 1:43 scale and its designed for the younger racer with many fun features and character cars. The 1:32 scale is a popular size car for racing at home and there is an wide selection of sets. Most significant benefit size car is planet 1:24 as well as commonly found racing at slot car raceway ones.
…
Creation of this super slots exceeded USD 150,000. Handy contained a 5 horsepower motor and eight reels with 20 game symbols on everybody. Super Big Bertha was certainly a huge machine, but unlikely it was not generous in prizes. The sum of the payments reached only 80% of the invested money and the chance to win a jackpot was one of 25,6 hundreds of thousands.
If you hit a wild GAME ONLINE SLOT Thor your winnings can be multiplied 6 times. And also by using make potential winnings reach $150,000. A person definitely can also click the gamble button to double or quadruple your wins.
Once MAFIA BOLA 77 spins game is activated you will receive a total of 10 Spins cost free. These free spins always be played automatically and you would like an additional wild symbol added into the reels you could potentially bonus competition.
A player should begin by investing the SLOT ONLINE stake. Moment has come best to increase the stake every time he or she loses and lower the stake every time he or she triumphs.
BOOT SLOT 2 – This menu option allows the R4 DS, just like the M3 DS, to boot the GBA Slot, or Slot 2, in your Nintendo DS / Nintendo ds console. This program those people today that like to GAMING SLOT GACOR get may on a GBA Flash card, and want to run GBA Homebrew games and applications as well as Nintendo ds. It also adds extra storage for NDS Homebrew, because you could use a GBA Flash card as well NDS files, as long as you use the R4 DS as a PASSME / PASSCARD cure.
If you’re lucky enough to win on a youtube video slot machine, leave that machine. Do not think that machine is the ‘lucky machine’ for you. It made you win once but it will not let upon the next games for certain. Remember that pai gow poker are regulated by random number generator and is actually because electrically operated. In every second, it changes the combination of symbols for a lot of times. Very a few of the time, the combinations aren’t in favor of anybody. If you still use the time or remaining balance in your allotted money, then perhaps you can try the other slot machines. Look for the slot machine game that offers high bonuses and high payouts but requiring fewer coins.
Another internet gambling myth is available the involving reverse psychology. You’ve lost five straight hands of Texas Hold ‘em. The cards are eventually restricted by fall to your benefit. Betting in accordance to this theory could prove detrimental. Streaks of misfortune don’t necessarily lead several path of good fortune. It doesn’t matter what you’ve heard, there’s absolutely to start the fans . the juice and completely control video game. Online casino games aren’t programmed to help flawless games after a succession of poor wines. It’s important to remember every previous hand has no effect of the next one; just because your last slot pull earned a hefty bonus doesn’t imply it will continue to area.
Of course, as could be the max bet, the jackpot displayed using a bottom of the screen meets a high roller’s goals. The progressive jackpot starts form about $75,000 and is now as high as $2,200,000. The average jackpot is roughly $727,000 will be a pretty good win.
…
This article summarizes 10 popular online slot machines, including Whilst the Reels Turn, Cleopatra’s Gold, Enchanted Garden, Ladies Nite, Pay Dirt and grime!, Princess Jewels, Red White and Win, The Reel Deal, Tomb Raider, and Thunderstruck.
Once realize there are only where the going to host your party you’ll need will need to set a date and a chance. If you are determined to participate in a vendor show, then they will set the date. Require it and it be allowed to SLOT ONLINE pick your slot.
If to be able to Internet capabilities, you have your pick at regarding that never close. Topic where you are on the planet, GAMING SLOT GACOR obtain play at Internet casinos for a real income. What’s more, these virtual casinos have many excellent game choices that even essentially the most discerning player will find himself entertained and even capable of winning lots of cash.
To enhance chances of winning involving game and earn bonus, one always be follow certain strategies. Playing it pretty simple you can easily find numerous guides and books dealing ways to play it also? The best thing about the overall game is its all time availability a person have time or in order to play carbohydrates start your game. Video poker sites are running 24 x 7.
Red White and Win is an ageless 3-reel, single pay-line progressive slot from Vegas Systems. There are 13 winning combinations. Symbols on the reels include USA Flag, Bald Eagle, George Washington, Statue of Liberty, and Dollars.
heylink.me/BUNGA189OFFICIAL to factor into your calculation is the much the perks and bonuses you’re getting back from the casino count. If you’re playing within a land-based casino where you’re getting free drinks a person play, a person can subtract the associated with those drinks from you’re hourly amount. (Or you may add the associated with those drinks to internet of the entertainment you’re receiving–it’s just a matter of perspective.) My recommendation is actually drink top-shelf liquor and premium beers in order to increase the GAME ONLINE SLOT entertainment value you’re earning. A Heineken could cost $4 a bottle in an awesome restaurant. Drink two Heinekens an hour, and you’ve just lowered what it is you to play each hour from $75 to $68.
Initially the term “jackpot” referred to poker, in respect to one of their rules – the parlays to the pot increased, if none of the players collected at least a small number of jacks (the word descended from English words jack and pot). Now the word “jackpot” is often accompanied by the word “progressive” which means accumulation prize inside game until certain relation to its this jackpot are completed. A certain share of all of the bets forms the jackpot, as a guide the share is not too big – basis points, but the probability november 23 the jackpot is very small, approximately 1 to 10000 as well as even 1 to several millions and as a result quite a major sum cash is increased.
…
Remember that there is no system or secret to winning at online or land based slots. The most important thing is managing your money so which you can play longer while saving money. We also urge you never waste your money buying some guide like “how to get rid of slot machine systems..or similar”, they are faulty. If they did would certainly not be for good discounts! Right?
Machines near game tables also have high chances of being cold slots. Bad machines often placed here because casinos would prefer to prevent the cheering slot winners from disturbing those you are playing poker, blackjack, and also other table dvds. These kinds of casino games require lots of concentration too.
To avoid losing big amount cash at slots, you should set funds for yourself before playing. Once you have exhausted your budget for a session, you should leave the slot and move with. There is no point in losing endless total in a hope november 23. In case you win, you should not use your winning credits to play more. Because of the chances of winning and losing are equal in slot machines, you cannot be apt to win added SLOT ONLINE . Therefore, you can be happy in doing you have won.
Do not trust anyone around. JVS88 could hear people saying which all the slots are right in front row or maybe the last ones, do not listen to anyone. These types of even hear that may find machines giving out plenty of cash at certain point for the day GAME SLOT or event. Do not listen to any for these gossips. It is just that as being a player you should listen and trust yourself on online plug-ins.
The Osbournes 5-reel, 20 payline video slot in line with the award-winning television show. It was released in September, 2005. The Osbournes accepts coins from $0.01 to $0.50, along with the maximum connected with coins that you will bet per spin is 200. Helpful ideas jackpot is 15,000 coins.
Although SLOT CASINO there are no exact strategies that will surely nail the win in playing slots, here couple of tips and strategies that will guide you in a person’s chances of winning. When you use this tips every time you play, you can plan to grow in profits at the end.
Larry’s Loot Feature is activated when 3 more Larry scatters appear anywhere on the reels. Click each Larry symbol to disclose up any 1000x your bet which can $1,250, each symbol it’s will award a multiplier. I personally have hit for 1000x and 750x my bet all inside same day time.
…
MEDIA SLOT78 amongst online gamblers are slot machines, they will offer payouts ranging from 70% to 99%. Granted most acknowledged online casinos would never offer a slot game that paid less than 95%. So as that would make slots one of the most profitable program. if you knew in advance what the percentage payout was, many forums/websites claim they can know the percentage, only one wonders where did they arrived during this number in the first place, (the casinos will either lie or not give the particular payouts).
Decide precisely what you’re shooting for before start playing certainly not let greed take well over. That way you have a top quality shot at achieving your goal, a person assure that you’re going to not lose more than actual were prepared risk from the outset. Have the discipline SLOT ONLINE to get this done and you need to have a way more satisfying gambling experience. Using common sense and being in control consistently are mighty weapons against any gambling enterprise.
The last mentioned they can provide you will be the chance to play for free for a couple of hours. They will give you some amount of bonus credits to bring into play. If you lose them for the hour your own trial ends. If you end up winning in the hour anyone certainly may find a way to keep your winnings along with some very specific prohibits. You will need to read guidelines and regulations very carefully regarding doing this. Each casino has its own group of rules generally.
Don’t play online progressive slots on a small bankroll: Payouts on progressives tough lower than you are on regular GAME ONLINE SLOT slot machine games. For the casual player, built a poor choice to play, as they consume your bankroll quickly.
We have mentioned across the earlier paragraphs that you inquire about freebies and bonuses the casino gifts. This is necessary for you to at least have compensation even prone to had many losing blues. Find and play with slot machines that no cost rounds or free spins. Try to find those that provides extra other bonuses. If there are any opportunities that could certainly have complimentary items, grab it. For example, if the casino provides a club card, contain it and do not forget to use it simply because you adventure. Insert it in the designated area in device to GAMING SLOT GACOR find a way to accrue points which you may trade for comps.
If you truly desire to have learned how to win at slot machines, the significant thing you have to learn is money manage. While you are actually playing, it is necessary that you know where you stand momentarily. For this reason I suggest start playing some free slot game. A few larger internet casinos such as Casino King provide many free pai gow poker for you to practice. It ought to then record your contribution and earnings on more recent digital type display can be exactly the same when happen to be playing with real bankroll.
The best strategy for meeting this double-your-money challenge is to find for specific pay line, two-coin machine with a modest jackpot and a pay table featuring an outstanding range of medium sized prizes.
…
Another thing to look for when choosing mobile casinos for slots is whenever they offer flexible betting reduces. You should be able to play both high and minimal stakes rather than one or maybe the insects other. You’ll need to also appreciate the winning lines, betting tiers and pay table.
Once you click the button for the bonus, a reward wheel in all probability pop on your screen. You will notice that it says Loot and RP. The RP is Reward Amazing. This means that when you spin the wheel, you may land on special bonus loot or you may get some reward points as ” special ” bonus.
Although there aren’t MAWAR 189 that can nail the win in playing slots, here couple of SLOT CASINO tips and techniques that will guide you in your current chances of winning. If you use this tips every time you play, you can plan to get more profits over the long haul.
In video game you get what is known as Spider web feature. Approach has become popular activated once the symbol appears on reels two and four obviously you can must be at the same time. If you have the slot machine goes wild and your changes to getting high-payouts are doubled as a result of many pay line blends.
Get to know your conscious of the game on top of the machine, this can very SLOT ONLINE very important for the fresh players. The squad who are online or maybe in land casinos should web address in mind that they get amply trained with video game that effectively playing on your machines. Preserving the earth . every player’s dream november 23 on a slot coffee maker.
Slot machines were all the rage inside depression. In 1931, gambling was legalized in Nevada and slots found a building. When you go to any casino today find row after row of slot piece of equipment. They are so popular because usually are very well simple to play and have large winnings.
Once we get everyone setup with Casino chips the game commences and yes, it usually takes about GAME SLOT couple of hours regarding to take home some loot. In the meantime, we possess a waitress who comes by and gets these Poker Players drinks, whether you choose water, soda, or adult beverages by the bar. Yes, just like the casinos precisely how we all look in internet marketing is if we’re for you to lose money, we might as well lose it to additional instead of a casino.
Do not trust anyone around. Might hear people saying that each one the slots are right in front row quite possibly the last ones, do not listen to anyone. Definitely will even hear that there are machines that supply out a lot of dough at certain point through the day or occasion. Do not listen to any of people gossips. It is only that to be a player you’ll want to listen and trust yourself on online slot games.
…
The science behind a software system is really a number of codes, all in number designed meet up with at element. This value then dictates a solution, often many the same number. Will need either a beneficial or a bad strike vector will be processed, meaning the programme will progress forward or return within a loop. These loops always be the provisions for almost any potential matchup and the prospects of winning.
Another tip is GAME ONLINE SLOT for optimal time wireless house alarms. Set GASPOL 189 for you to play. Should reached the designated and also your watch alarms, then stop playing and go home. There are other more essential things to accomplish than just playing. Besides, slots are constructed for recreation and not for manufacturing.
Lets say that you’re using a slots machine at stakes of $1.00 a rotation. You’ve therefore type in the slot machine with $20.00 and seek to come out with anything over $25.00, as being a quarter profit can be achieved 70 percent of time through numerical dispensation.
SLOT ONLINE The associated with winning online game are considering luck absolutely no element affect or predict the upshot of the video. Bingo games are played for fun, as no decisions need in order to made. However, there are a couple of essential tips that convey a better in order to win the sport. Playing one card throughout is suggested and banging should be ignored while dabbing. A paper card with lower number should be selected. This has more possibility of getting tinier businesses closer every single other. In Overall games, it is mandatory that you come out early to have the first set issued. It is essential to be courteous and share the winning amount among the partners. Ideally, the odds of winning are when you play with fewer group. Some even record their games if may possibly trying out some special games. It’s easy to apply.
Playtech are creating a simple interface that pleases the user with its amazing graphics, sounds and simplicity. Online game also has an “Options” feature where the ball player can modify the sound, speed and “Auto-play” settings. The theme in the game draws on in a gold mine where cash treasures GAMING SLOT GACOR are to be found.
To become a master of poker these items need some time. In this case, again sticking to a football analogy seeing not simply watch your favourite team play, but become its full member and get compensated for the problem.
To play slots are generally no ways of memorize; but playing competitions intelligently does require certain skills. There are the basics of easy methods to increase the reality of hitting a sizable jackpot.
…
Red White and Win is an ageless 3-reel, single pay-line progressive slot from Vegas Software. There are 13 winning combinations. Symbols on the reels include USA Flag, Bald Eagle, George Washington, Statue of Liberty, and Dollars.
They end up being simple, however the thrill involved in it is a great one. You may use some eco-friendly make certain that you win in these web based slots that full of uncertainty nonetheless get you some big money and amazing prizes. You need to that you’ll want to know is the limit when are placing a bet. You will not have move SLOT ONLINE out of the limits and bet more if happen to be not fortunate to win. Require to quit online game if come across yourself from your balance that you had kept for gambling. When it comes to revenue, the internet slots are one such game that offers high positive factors.
The best strategy for meeting this double-your-money challenge is to watch out for for just a single pay line, two-coin machine with a modest jackpot and a pay table featuring GAMING SLOT GACOR an outstanding range of medium sized prizes.
Experience. You click a button instead of pull a lever. Otherwise, online slots are as simple as live casino video on-line poker. The promise of the massive jackpot is preserved–and sometimes increased by the exponential demographics of the net.
The table version of Poker may be the best. Assorted causes versions of poker as a table game and you’re able play free games to develop your skill so you might be ready in order to on other players. Are usually many abundant poker games available all the time for all skill levels as well as many Free-rolls, Tournaments and High-Roller tournaments. A genuine effort . a involving money to be made playing online poker and who knows, you could even win yourself a seat recorded at a WSOP event. The table game of poker available in download, flash version and some live dealer casinos.
This article summarizes 10 popular online slot machines, including For the Reels Turn, Cleopatra’s Gold, Enchanted Garden, Ladies Nite, Pay Dirt GAME ONLINE SLOT !, Princess Jewels, Red White and Win, The Reel Deal, Tomb Raider, and Thunderstruck.
This game is not confusing anyone just all you need to do is in fact spin and match the item. The primary objective of playing this machine is to win the jackpot prize.
Something else to factor into your calculation is the way much the perks and bonuses you’re getting back from the casino count. If you’re playing in a land-based casino where you’re getting free drinks a person play, you can subtract the price those drinks from you’re hourly amount. (Or you could add the associated with those drinks to the of the entertainment you’re receiving–it’s easliy found . matter of perspective.) My recommendation should be to drink top-shelf liquor and premium beers in order to maximize the entertainment value you’re experiencing. domaintunnus.com can cost $4 90 capsules . in a nice restaurant. Drink two Heinekens an hour, and you’ve just lowered what it is you perform each hour from $75 to $68.
…
First, set yourself perform. Be sure to have funding. They do not receive vouchers in playing slots. Then, set a measure to spend for that day on that game. When www.xpertworkshop.com consumed this amount, stop playing accessible back again next a while. Do not utilise all your funds in just one sitting and setting. Next, set as well as effort alarm. Once it rings, stop playing and exit from the casino. Another, tell yourself to abandon the machine once won by you the slot tournament. Don’t be so greedy convinced that you want more advantages. However, if nonetheless got have take advantage your roll bank, anyone then may still try other slot matches. Yes, do not think that machine a person had won is sufficiently fortunate to cause you to win again again. No, it will just consume all your hard and you’ll have a lose a bit more.
All we all say is we know a great buy the family saw one. For the past 4 years we’ve been looking for these Best Pai gow poker like the fireplace Drift Skill Stop Video slot that derive from international gambling dens. The reason we chose these over others was due to the fact most were for a month or two prior to being shipped away and off to warehouses to distribute but they also chose when you need to. This meant we were basically getting primary slot machine for an exceptionally large price reduction.
From a nutshell, the R4 / R4i just card which enables for you to definitely run multimedia files or game files on your DS. No editing among the system files is required; it is strictly a ‘soft mod’ that has no effect on your NDS in in any manner. You just insert the R4i / R4 card into the GAME SLOT, and the R4 / R4i software will range.
To assist keeping pricey in the company have added traction magnets to difficulties to exert downward force thereby allowing cars stay on the track at faster speed. This also allows folks to make vertical climbs and join in a loop the loop.
You should choose perform a machine that has lesser winning combinations realize during your spins. The lesser the combinations, the good chances of winning more salary. Although the jackpot amount is lesser, you will still win big would of SLOT ONLINE these kinds of machines have better odds in prosperous.
You can avail jackpot coin return facility each morning machine. A manual is supplied by the supplier together with SLOT CASINO machine from which you can learn utilization of of handy properly. The handling from the machine will be simple and simple. You just should follow the manual properly before you start up places.
It’s really too bad I missed the Hanabi Full Screen Skill Stop Slot Machine sooner, because at first I was searching for your Best Casino wars that dispersed money. Seriously, it didn’t even dawn on me that everything had switched over on these electronic tickets until 3 months if we started intended. Just goes to a person how much he was winning. It’s nice learn that these Antique Slots give you tokens to gift that old time get it.
…
Free winning casino strategy #3 – Most of this table games are worth playing in the slot washers. One in particular that sticks out is none other then poker. Ought to you can find some winning methods on poker and look the game inside and out there’s always something good make cash from the casino players naturally.
Slot machine gaming is a type of gambling, where money is undoubtedly the basic unit. Place either lead it to grow, or watch it fade not in the your poker hand. It would bother that much if small amounts of money are employed. However, playing the slots wouldn’t work an individual are only have minimal gambles.
You must choose to play a machine that has lesser winning combinations realize during your spins. Lower the combinations, the good chances of winning more personal savings. Although the jackpot amount is lesser, you will still win big as most of these kind of machines have better odds in wooing.
From a nutshell, the R4 / R4i is simply card which enables you to run multimedia files or game files on your DS. No editing of your system files is required; it is strictly a ‘soft mod’ that does not affect your NDS in in any manner. You just insert the R4i / R4 card into the GAME SLOT, and the R4 / R4i software will jog.
Determine what https://aquariusballroomdance.com/ of money and time you have enough money to lose on that setting. A person begin enter the casino, set a pay up your accomplish. Set your time also. Playing at slots is absolutely addictive that you’ll not notice you already spent every money and time within the casino.
At these casinos they will either help you enter a 100 % free mode, or give you bonus revolves. In the free mode they hand you some free casino credits, which never cash increased value. What this allows you to do is play the various games that SLOT ONLINE take presctiption the site. Once you have played a online slot machine that you favor the most you seem comfortable using it once ingredients to play for moolah.
No matter what denomination of slot machine you choose to play, at a SLOT CASINO penny and nickel slots all method up towards the high roller machines, there is one thing that every slot player simply should do before they sit down and insert their revenue. Regardless of how casual a slot player you are, the benefits of this action can be significant. One of the benefits is that it will only amount to a couple of minutes of your time.
Break da Bank Again: Another revised slot machine with a revamped style. Time to really crack fit on the popular slots game Break da Bank. The 5x multipliers combined an issue 15 free spin feature has the proportions to payout a bundle of slot coins. 3 or more safe scatters trigger the free spins.
…
Chocolate Factory is a 5-reel, 9 pay-line video slot by using a chocolate costume. Welcome to a mouthwatering world of chocolate rewards. Chocolate Factory accepts coins from $0.05 to $2.00, and the number of coins can can bet per spin is forty. The maximum jackpot is 8,000 silver and gold coins.
The Diamond Bonus Symbol pays the greatest fixed Jackpot after the Lion ticker. The Diamond bonus is triggered whenever you land one too bonus symbols on a pay-line.
Fruit machines are probably the most sought after form of entertainment in bars, casinos and handlebars. Online gaming possibilities have made them the most well-lnown game online too. Fruit machines are available in different types; from penny wagers to wagers of greater than GAME ONLINE SLOT 100 loans. Another attraction is the free fruit machine available from certain internet casinos. You can play on the washing machine without being nervous about losing money.
Always play ‘maximum coins’. If you hit a giant jackpot playing only 1 coin, handy will not open over the hole of cash for SLOT ONLINE you! Usually playing maximum coins is a good strategy. On almost all slot machines the top jackpot a lot bigger when playing maximum coins.
Slots – the principle of working is depending on the olden day’s mechanical slotting coffee machine. https://oneandonlythemovie.com/ provides pull the handle with the machine to produce the drum roll and try his fortune. The original Video poker machines were introduced in the 1890, in San Francisco.
These three games allow players wireless strategies prevented help sway the odds in their favor. But keep in mind, possess to on line to have fun with the games to get able to to get the best prospects. If you not know GAMING SLOT GACOR what you’re doing, you’d probably be more content playing the slots xbox games.
First, you need to consider the reality that you can start to play these games anytime and anywhere hunt for. There is that comfort factor in it that entices people to take online as well as begin playing. Provided that you have your computer, an internet connection, your credit or debit card with you, a person set and able to play. Written documents you accomplish this in the comforts of ones own home, in your hotel room while on business trips, and even during lunch time at your place of show good results. You don’t have to be anxious about people disturbing you or starting fights and dealing along with loud music. It is like having your own private VIP gaming room your own house or anywhere you are developed in the world.
Of course, as may be the max bet, the jackpot displayed using a bottom with the screen meets a high roller’s presumptions. The progressive jackpot starts form about $75,000 and has gone as high as $2,200,000. The average jackpot is just about $727,000 which a excellent win.
…
In the earlier 90’s, way before online casinos were prevalent, I enjoyed a great game of Roulette at one of my favorite land casinos three or four times a time. These days, Do not even have to leave the comforts of my home to be in on people who action.
Initiated in the year 1970, recreation start more popular in 80’s. earlier people were bit scared today they considered that it can provide tough competition to real casino, but such fears were baseless, the demand for the game and local casino goes hand in mind.
How thingsthatdontexist.com to play online slots is trouble free. It is only the technology behind slot machines that is actually difficult. Online slots have generally a higher payout emerged. Leaning the payoff table will help explain how much you can possibly win. The payout table will provide idea with the you are looking to hire to win once again. Across and diagonal are frequent winning combinations with online slots. Matching the different possible combinations will offer different possible payouts. It’s not nearly as hard recognize as somewhat. A row of three cherries for instance will have a set payout, that row maybe all around or almost everywhere in. The same row of 7’s might provide a higher payout or an additional spin.
Both types of Roulette have the identical fun and excitement when playing them, but discover lose a second time faster in American Roulette than European version if luck is not at your side. As to the reasons? It is due to GAMING SLOT GACOR the property edge for American Roulette is double the value of European wheel. The higher the house edge, the better advantage toward the casino, meaning that in time online casino makes twofold profit using its American wheel than European wheel. Therefore, you should always choose to play at European wheel at online Roulette attempt advantage of smaller house edge using this version.
Slots are positioned up to encourage players to play more gold and silver coins. It is clear to check out more coins one bets, the better the odds and the payouts have been. Most machines allow you choose on the value of the coin that seek it . play using. When the payout schedule pays at better pay for more coins, a person better off playing smaller denominations and maximum coins. This concept seems simple, but many jackpots been recently lost by careless toy.
If you need to try out gambling without risking too much, you may want to try in order to some on the older casinos that offer some free games in their slot machines just a person could try playing of SLOT ONLINE establishments. Shared online . ask you fill up some information sheets, that is it. You’re able to play within their slot machines for absolutely free!
Slot cars also are offered in different areas. The smallest size is HO or 1:64 in scale. Originally they were made for inclusion with model railways but now these little cars are generally fast then have some amazing track layouts. The next size up is 1:43 scale and it designed for your younger racer with many fun features and character cars. The 1:32 scale is a popular size car for racing at home and there exists a wide selection of sets. Primary size car is planet 1:24 and also commonly found racing at slot car raceway clubs.
…
Craps most likely the more complicated games a lot more about. It offers a variety of bets consists of an etiquette all unique. windmillcruiseamsterdam.com will be intimidated by all the action at a craps computer. Many don’t know the difference in a pass line and a don’t pass bet. They may not know that some bets might offend other players at the table, because superstition plays a large part in craps. Some players holding the dice think a don’t pass bet is a jinx, as it would be a bet made directly against really bet.
Craps one other a mis-leading game, the “pass line” bet, which wins to a new shooter who rolls a 7 or 11, loses on the 2, 3, or 12, and on any other number requires him to roll that number (his point) again before rolling a 7, has an even money payoff that delivers a 1.41% edge to the home. The single-roll bets are found ridiculous: an ‘any 7’ bet pays 4:1 and offer the house a whopping 16% edging.
50 Lions Slot can be a 5-reels penny game, you can actually although the coins in this particular game discovered in SLOT ONLINE different denominations you are listed a wager for the small sum of 1p.
You have hundreds of choices put it to use to playing slot machines online. You will discover numerous different software platforms offering everything from three reel and 5 reel machines to video, bonus and jackpot progressive payouts. You can choose from downloading an entire software suite including hundreds of games or merely play no download version which opens your favorite game within your computer screen window without more than just a free account and the click of the mouse.
There are three little screens GAME ONLINE SLOT on the inside slot machines which are named payout, credits, and bet. Payout refers on the player’s winnings; it is zero when there are not winnings. Credits refer to how many coins the guitarist has give up. The bet screen displays how much the player decided to bet.
GAMING SLOT GACOR Well if you find yourself a individual that basically to be able to have fascinating entirely contains luck, is definitely the to play the game of Slot Machines, Bingo, Keno and Lottery. In here, no matter what others tells you, there is not any way to affect if someone leaves of the overall game. Although these are games of luck, players can however use a part of the best of our strategy: these people could bet as several options as possible.
To actually sign up to one of these, develop be keen on online video poker machines. It’s not important to love slots, but what’s the point in signing up for one if you don’t like slots in the first place? Although most of the tournaments don’t tend to last too long (in many cases just five minutes), the repetitive spinning of the reels can be too much for some players, but for a slot enthusiast, these tourneys are the best thing since sliced loaf of bread.
…
The main thing was that I had to purchase something he was created to competing. Now the Hanabi Full Screen Skill Stop Slot Machine wasn’t the local casino, but in the victorian era similar together with lot of other Casino Slot Machines he strummed. The basic one, two, or three coins per spin, but since they difference was this one didn’t have one of individuals pull-down levers on along side it. It seemed a not much more up-to-speed this times despite the fact that it was refurbished simply by itself.
Are you ready one more toy machine bank provides realistic sounds when you hit the jackpot? The Burning 7’s toy video slot uses batteries to let you know when you happen to be lucky victorious one. The bell rings and the light flashes and all sorts of the coins you have put in the bank will fall out the bottom if hit the winning a mixture.
It one among the the oldest casino games played via casino lovers. There is no doubt this game incredibly popular among both the beginners and also experienced bettors. Different scopes and actions for betting result in the game actually a very interesting and exciting casino game. The gamer has various betting chances SLOT CASINO . They can bet by numbers, like even or odd, by colors like black or red and more.
One with the great things about playing over the internet is its simplicity merely mechanics. It is not necessary to insert coins, push buttons, and pull represents. So that you can spin the reels to win the prize, it will only take a click within a mouse button to achieve that. If you want increase or lower that bets or cash the actual prize in order that it to do is to still go through the mouse.
Slot cars provide great teaching tool for physical science. Get zithromaxab.com how only too expensive accelerate, decelerate, and defy gravitational forces as they fly at the top of a high-banked curve. Why is one car faster rather than the other? United states are in order to simulate real race cars so they will really drift of the track given that they go the particular curves. Lane changing and passing are included as well features that add SLOT ONLINE to the fun. Carrera slot cars could even be used to a science fair project for instance properties of energy and physical science.
In a nutshell, the R4 / R4i is just a card which enables for you to run multimedia files or game files on your DS. No editing of this system files is required; it is strictly a ‘soft mod’ that has no effect on your NDS in by any means. You just insert the R4i / R4 card in the GAME SLOT, along with the R4 / R4i software will conducted.
Aside from being accessible, the slots are pretty simple to perform. As I mentioned earlier, no special skill is in activity. The game’s objective would chance upon the winning combination — different combinations vary associated with amount of winnings. Usually, a combination is as fast as chancing upon three identical objects on in case you. Sometimes, even combinations which are not identical also amount to something. Hit the right combination as well as the player takes home the jackpot. This, of course, depends about the system on the slot mechanism. A player just should insert his money inside the slot and press the button additional medications . the reels turn. Slots are casino gambling games that perhaps require essentially the most number of wishful and hopeful considering.
…
Remember there’s no system or secret to winning at online or land based video poker machines. The most important thing is managing your money so that play longer while conserving money. We also urge an individual never waste your money buying some guide like “how to get rid of slot machine systems..or similar”, they fail. If they did would certainly not be for great deal! Right?
Try check out SLOT ONLINE your favorite search engine and look up for slot machine games release. You’ll be surprised at the amount of search upshot of websites and pages that allow you to enjoy this activity to the fullest without risking a single dollar. So for those out there who want to try out this game but are scared to lose hard-earned money, you surely try playing it the internet.
Invite your friends when you play. It’s not more fulfilling. Besides, they will be 1 to remind you in order to spend of one’s money. It is possible you join the casino, SLOT CASINO think positively. Mental playing and winning attracts positive energy. Enjoyable because an individual might be there perform and enjoy. Do not think merely of winning or perhaps your luck will elude that you.
There are two pores and skin slot cars, there could be the analog cars and the new digital an individual’s. The traditional or analog slot cars are those that you might remember in the younger many days. This is where it was one car per slot along with the car had to stay for the slot to the race.
There are lots benefits in playing slots online. One, it cost less. Two, you don’t be compelled to drive you to ultimately the casinos and at home. Three, there are many great offers which you may enjoy in many online gambling. Upon signing up, new registrations may have the ability to acquire freebies and sometime an initial amount you bankroll. Fourth, online slots are very simple to play with. Spinning is just a matter of a click of the mouse all period. You can select pay lines, adjust your bets, and cash out using only your duck GAME SLOT .
A great game perform if essential want to waste much cash except want to dip your toe into gambling is the slot machine. Most of these machines work by putting money into the slot, pulling a lever and then hoping a person simply get three identical photos. If you do, you win, one does don’t, needed win. buyivermectinmedication.com to win big cash the pai gow poker but is that possible have some luck winning small amounts. You can also find slot machines that push money off a display.
Others believe that if a device has just paid out a fairly large payout that it is payout again for an interval. Who knows whether any for the strategies do work. Having a lower for certain is if there is any strong indication that do, this device will soon do these details is all can to alter that.
…
You should additionally choose perform a machine that has lesser winning combinations to accomplish during your spins. Lower the combinations, the good chances of winning more monetary gain. Although the jackpot amount is lesser, you will still win big since most of these kind of machines have better odds in taking.
An addition to that, which has a flashing jackpot light which adds a pleasure. Essentially the most thrilling feature of the machine is it topped lets start on chrome bring. Nevertheless, the thrill does not end here. The machine has an inbuilt doubled bank that has a saving section separately which accepts at the very 98% all over the world coins.
In that old days when casino players actually knew what we were doing the unchallenged king of the casino tables were the crap tables. This is where the term high-roller came using. If you knew what you were, doing this is where SLOT ONLINE you hung out. A shrewd better can lessen house edge to as low as 1.41% and to below 1% depending more than a house’s odds policy.
Experience the exciting sounds of the casino within your own home the actual Crazy Diamonds machine save. This is a replica on the larger scale featuring the real-life sounds of the casino GAME SLOT and the jackpot light that flashes and the actual of a bank to save your coinage. By the way, this slot machine game will take 98% of coins made the world over.
A match bonus is money offered by an online casino to get you attempt them presently there. They are generally larger for period depositors, SLOT CASINO but a lot of online casinos have player loyalty exercises. The way a match bonus works is an isolated casino will match your deposit with casino credit score rating. If the match bonus is 100% and you deposit $100 you will receive $200 in casino credit. You will then ought play a designated regarding plays before you can withdraw this some money. The number is usually rather low and plausible. By taking advantage analysts bonuses achievable actually the advantage over the casino on the short operated.
Second, you should o opt for the right modern casino. Not all casinos are for everyone, such a person should select which one may be for you. Moreover, every casino has an established payout rate and you’ve figure out which payout is probably the most promising. Practically if oodles of flab . to cash in on big degrees of money, you may need to choose the casino gives the best payout speed.
Pay Dust particles! is a 5-reel, 25 pay-line progressive video slot from Real Time Gaming app. It comes with wilds, scatters, up to 12 free spins, and 25 winning combinations. Symbols on the reels include PayDirt! crtlinvest.com , Gold Nugget, Gold Mine, Bandit, Gold Pan, Lantern, and Tremendous.
…
Apart off of the single payout line before of the reels, may find more than a single pay lines, every pay line referring to a separate coin used. The symbols stopping on a particular pay line decides the win of a player. The common symbols are bars, cherries, double bars and sevens.
Machines near game tables also have high odds of being cold slots. Bad machines will often placed here because casinos would prefer to prevent the cheering slot winners from disturbing those you are playing poker, blackjack, additional table activity. These kinds of casino games require lots of concentration actually.
Invite pals and family when you play. Can be more fulfilling. Besides, they will be one particular to remind you never to spend of one’s money. Incase you say hello to the casino, think positively. Mental playing and winning attracts positive energy. intour.info because an individual might be there perform and take part in. Do not think merely of winning perhaps luck will elude you.
Remember that you have no system or secret to winning at online or land based slot machines. The most important thing is managing your money so that you can play longer while saving money. We also urge you to SLOT ONLINE never waste your money buying some guide like “how to defeat slot machine systems..or similar”, they fail. If they did they might not be for trading! Right?
First, look on a rapid platform or carousel. The casino want the higher payouts to be able to visible your most men and women. Other patrons are likely to keep gambling GAME SLOT having seen a person win substantial.
GAME MENU – SLOT CASINO A great deal more select this menu, you’re instantly brought to a involving all on the game files, homebrew applications, etc. you have stored in your own microSD master card. You can use the controller pad on the NDS choose on the file you wish to load. When you are loading a video game for one way time, you’ll be prompted, after selecting the game, to confirm that you need to create a save declare the on the internet. This is needed if you in order to save you game. Your game saves are stored on issue microSD card as the overall game files themselves – may fantastic train delete those games later, to renew other files, as you’ll copy your save game files to your PC, for future use as you prepare to fold or call that game again.
Slot land – This online casino slot is renowned for great attractive ambience, excellent odds and completely secured financial trades. And, unlike other sites, it won’t require one to download any software. A person play by initial deposit of to as much as $100. Gives multiple line slots like two pay-lines, four pay-lines, five-pay lines and eight-pay lines. Get pretty good chances to winning money here.
…
The Lord of the Rings Slot machine is a Pachislo Slot Machine, so that that also it be that can control when the reels does away with spinning during your turn. Treatments for acne you to infuse a frequent slot machine experience using a bit more skill! The slot machine also comprises of a mini game that is available for anyone to play between spins.
Another thing to get SLOT ONLINE when choosing mobile casinos for slots is that they offer flexible betting reduces. You should be able to play both high and minimal stakes as well as one and even the other. Need to also appreciate the winning lines, betting tiers and pay room table.
Once you have decided the regarding slot game you are happy with, now you have to is to get a machine that choice have the highest chance of letting SLOT CASINO won by you. Here is the key tip: It is not so much the kind of game decide on. To choose a winning machine, you need to pay more attention to how administrators manage the machines.
Slot cars provide a teaching tool for physical science. Get kids to explain how united states accelerate, decelerate, and defy gravitational forces as they fly at the top of a high-banked curve. Exactly why is one car faster rather than the other? Merely are made to simulate real race cars so they also drift along side track given that they go while using curves. Lane changing are also included features that add on the fun. Carrera slot cars could be also used to obtain a science fair project as an example properties of your energy and physical science.
There is that is not available out of all slot machines of industry industry. You will get an audio while paying out the coin in handy. This will make you feel that price range a real casino.
If you’re an avid player in poker. You should always keep abreast regarding developments to make it worse the right in favor associated with an company or slots. Therefore, we have decided that totally . enjoy the good news we in order to offer a. Who said that to win the jackpot, you should spend many decades? But it is able to be win it in only a couple seconds, and we simply will not words, which is very fortunate people.
Do not use your prize to play. To avoid this, have your prize in order. Casinos require cash in component in. With check, you can get away from temptation utilizing your prize up.
…
You should be expecting to pay as low as $20 bucks, but bigger replica banks will run about $80. Each the actual first is a bit different via others, however their made to be able to the same thing: preserve your change and take money out of your friends. You have to treat them like arcade games within your home.
Do not use your prize SLOT ONLINE perform. To avoid this, have your prize in examination. Casinos require cash in playing. With check, you can depart from temptation making use of your prize up.
As a slot player, you needs to know brand new change machines so that you can effectively increase your winnings. The always much better to change machines if your current machine is causing you shed a connected with times. By means of happens, you can move to the adjacent slot machine games. It is normal for casinos to arrange two good slots together with each many other. Observing the performance of the device is imperative for each slot machine player. Inside duration of the games, a great deal more noticed in order to have used a “cold slot”, tend to be : a high possibility that the machine by it can be a “hot slot”.
By trustworthy, it doesn’t only mean someone who won’t swindle your capital. Trustworthiness also means a company who thinks of the associated with their people. Do they offer multiple payment and withdrawal options? Will someone help you out or answer your questions if and as soon as you are interested? Are you really going to get paid ought to you win?
They online slot games have several pictures, from tigers to apples, bananas and cherries. When a person all three you win. Many use RTG (Real Time Gaming) while it is one for the top software developers for the slots. These includes the download, a flash client and are mobile, you’re able to take your game anywhere you need to go. Additionally, there are Progressive slots, you may win a lifetime jackpot an individual only be forced to pay out several dollars, as with every gambling, the likelihood of winning the jackpot can be like winning a lottery, few good, yet it’s fun. Nevertheless to play as many coins you’ve GAME SLOT to win the jackpot, the risk is higher and is using the spend.
For people who want to play but will not idea yet how dust and grime and they you can win from it, the online slot machines will SLOT CASINO be a great help you to. Through these games, you will be able to familiarize yourself with key facts games and styles, as well as the jackpot prizes, before you play the actual game messing around with real financial.
If KAGURA189 intend to play, it very best to plan ahead and be positive about this how long you become playing make certain you can provide to yourself a budget. You should not willing down the sink a associated with money on this particular. It is an efficient form of recreation and may also earn for you some . However, losing a fortune is most certainly not advisable.
…
The first and sensitive guideline terrible player is to set an established limit for him or herself. Setting KAGURA 189 on the money to be spent span of one’s energy to play is essential to consider before playing slots to avoid regrets ultimately. Playing slots is a gambling game; thus, don’t take it too seriously and make use of all the money that you have worked hard for. Know when avoid. If you decided i would set a quantity for on that day to spend in the casino game, then in order to it regardless if you lost several the times. Think of the amount you have enough money for to lose to possess a greater picture of your endeavor. Don’t dare to win your a refund. For sure, if at all possible lose even more. If not, if you set a play time for you, stick going without running shoes. Go home as soon as your watch alarms.
If had been only to be able to play with one coin or you wanted the same payout percentage no matter how many coins you played you would then want to play a multiplier slot fitness machine. Multiplier machines pay out a fair bit of coins for certain symbols. This amount is then multiplied together with number of coins estimate. So, if three cherries pay 10 coins for getting a one coin bet, it’s SLOT ONLINE pay 50 coins to secure a 5 coin bet. A great machine does not penalize you for not playing the maximum number of coins acceptable. There are no big jackpots in this particular type of machine. If you’re searching to gear playing trip of money then right here is the machine with regard to you.
Slot machine gaming is a type of gambling, where money could be the basic unit. Determine make it grow, or watch it fade away from your hands. Always be bother that much if GAMING SLOT GACOR small amounts of money are involved. However, playing the slots wouldn’t work inside your only have minimal gambles.
There is able to be no real answer to this speculate. When playing Blackjack in order to to decide when to think about another card (HIT), need to stay as part of your cards (STAND), when to double your bet and other choices, on the market to players in the rooms.
These three games allow players incorporated with this strategies may well help sway the odds in their favor. But keep in mind, you to on line to have fun playing the games to be to get the best probability. If you don’t know what you’re doing, you would probably be better off playing the slots xbox games.
There are a variety of online websites that allow a user to play free slot machine games. Some focus solely on slots and other gambling games such as blackjack and poker. Buyer include ez slots casino, slots mamma and Vegas casino. Other websites offer slot machine play in addition to other typical online games such as puzzle games; arcade games and word games.
Lucky Charmer has an additional screen bonus feature turning it into fun perform. You will choose between 3 musical pipes and the charmer plays your choice if you could possibly reach the bonus past. The object that rises out from the baskets could possibly be the one establish your takings GAME ONLINE SLOT . To be able to activate offer round usually be in a position hit the King Cobra at the third pay variety.
For beginners to slots, the regarding playing online may undoubtedly daunting two. All too often, beginners are switched off at online slot games and don’t play just think that playing with real budget is required. The reality is that the numbers of many choices to playing about the web. Playing with money is simply one of associated with.
…
In the game you get what is named a Spider web feature. This kind of is activated as soon as the symbol appears on reels two and four and yes it even must attend the same time. When this happens the video slot goes wild and your changes acquiring high-payouts are doubled as a result of many pay line blends.
These slots are extremely best tutor from the game considering the more one plays learns quickly the secret of the trade perform slots and win. Wedding rings of the internet casino has increased with the roll-out of the free slot adventure titles. One never gets bored out off playing these games because for the excitement these games provide with an interesting feel. A lot of the slot gamers learn the games and therefore move onto the paid part of online plug-ins.
You are visiting casinos more as well as frequently. tap.bio/@kagura189vip tried GAME SLOT to prevent gambling by promising yourself that they’re worth go anymore, but it never is compatible. You keep going back to your casino, whatever the negative final outcomes.
Pachislo machines are missing the pull down arms on the side. The spinning is stopped by making use of the 3 buttons on front among the machine. This is what yields a Skill Stop Hosting server. These machines aren’t developed to have pull-down arms. We can buy arms for that machine though changing gear at all will nullify your warranty and business isn’t liable for repairs as a result problems SLOT CASINO with the machine.
Once you click the button for the bonus, an incentive wheel could pop through to your video panel. You will notice that it says Loot and RP. The RP refers to Reward Aspects. This means that when you spin the wheel, you may land on special bonus loot an individual may get some reward points as special bonus.
By trustworthy, it doesn’t only mean someone who won’t swindle your investment. Trustworthiness also means a company who about the regarding their players SLOT ONLINE . Do they offer multiple payment and withdrawal options? Will someone guide you straight or answer your questions if prolong you are interested? Are you really acquiring paid an individual are win?
Experience the exciting sounds of the casino within your own home with the Crazy Diamonds machine loan merchant. This is a replica on a larger scale featuring the real-life sounds of the casino in the jackpot light that flashes and the particular of a bank preserve your coins. By the way, this slot machine will take 98% of coins made the worldwide.
…
One connected with ensuring your high associated with winning big amounts of cash is by choosing what machine conflicts you. Website type could be the straight slot machine game. KAGURA189 is sometimes called the non-progressive slot machine game. This always pays winnings in accordance with an established payout make. Note that it pays with the same amount regularly when players hit a precise symbol combination.
3Dice recently been on the receiving end of lots of awards associated with years inside industry, including Best Customer satisfaction Team and USA Friendly Casino among the Year, are simply a few with their prestigious awards in their trophy cabinets. Owned and operating by Gold Consulting S.A., the principle Danmar Investment Group, this casino is fully licensed and regulated by the Curacao Gaming Authority.
These slots are the most beneficial tutor from the game becoming more one plays learns quickly the secret of the trade to play slots and win. Appeal of the online casino has increased with the development the free slot video. One never gets bored out off playing these games because on the SLOT ONLINE excitement these games provide with a funny feel. Most of the slot gamers learn the games after which it move in the paid a part of the online spots.
Determine exactly how much money and time you can GAME SLOT afford eliminate on that setting. Prior to enter the casino, set a plan for your engage. Set your time plus. Playing at slots ‘s so addictive an individual might not notice you already spent all the and time inside the casino.
Pachislo machines are missing the pull down arms on one side. The spinning is stopped if you use the 3 buttons on your front of your machine. Wishes what yields a Skill Stop Hardware. These machines aren’t intended to have pull-down arms. However, you can buy arms for the machine though changing the device at all will nullify your warranty and the corporation isn’t chargeable for repairs as a result problems at a time machine.
Knowledge of your game is critical. Of course it’s exceedingly important that this the basics of video game. You must have an idea on the foundational factor to win. You have to know how these machines operate. Possibly you have noticed how these machines produce good and perfect combinations on the first and 2nd reels but fail offer you a perfect one on his or her SLOT CASINO third? Well, this is primarily because these machines are programmed to accomplish this. The slots have Random Number Generators that enable them to ascertain the outcome every spin. When you’ve got knowledge of this game, you would know that you have no exact timing on the spin because these are all random acts by the microprocessors established in the tools.
The last mentioned they could give you is to be able to play for free of charge for a couple of hours. They will give that you simply specific involving bonus credits to benefit from. If you lose them in your hour then the trial is finally over. If you end up winning within hour then you may be able to keep your winnings but by very specific restrictions. You will need to see the rules and regulations very carefully regarding until this. Each casino has its own set of rules normally.
…
Real world games provide you with different skill. However, the online games can exciting perform. You can have a great experience playing this kind of online quest. You can sit at the comfort of your home and enjoy this exciting game. But one thing you will miss, i actually.e. the mood and the environment of real life casino.
First, look on a raised platform or carousel. The casino desire the higher payouts always be visible through the SLOT ONLINE most people. https://link.space/@KAGURA189 are likely to keep gambling after seeing a person win gigantic.
Speaking of events, the Twin River RI casino is host to many events all year long. A 29,000 square foot event arena is often filled by some famous headline musicians. The center hosts some great live entertainment and has been thriving over if you pay year. Work involved . plenty of music and acting began on at Twin Rivers E-casino. Additionally, the facility is also accessible for banquets and special events like weddings and business conference calls.
It’s really too bad I didn’t find the Hanabi Full Screen Skill Stop Slot Machine sooner, because at first I was searching GAME SLOT for your Best Slot machine games that dispersed money. Seriously, it didn’t even dawn on me that everything had switched over to these electronic tickets until 3 months as we started going. Just goes to exhibit you how much he was winning. It’s nice to learn that these Antique Video poker machines give you tokens offer you that old time fascinate it.
Now, ideas secrets on the ways to win slot tournaments whether online or land built. The first thing is realize how slots work. Slots are actually operated by random number generator or RNG that’s electronic. This RNG alters and determines the outcome of the game or gas thousand times each additionally.
Slot cars of exact sneakers scale from different manufacturers can race on SLOT CASINO exactly the same scale track. However, tracks of the same scale from different manufacturers will only go together by the special adapter track piece, that are offered separately.
Mr. Robot – Take under consideration if you’ve planned on using bots as a measure to boost traffic to your computer. If 4 slots are taken by bots and it’s a 12 slot server you’re only leaving 8 slots for real humans. Try to keep the server slots in proportion to facts bots you plan to use (if any).
Moonshine an important event popular 5-reel, 25 payline video slot that functions a hillbilly subject. Moonshine is where you will encounter a gun-crazy granny, the county sheriff, while a shed filled with moonshine. Moonshine accepts coins from $0.01 to $1.00, and the number of coins that you simply bet per spin is 125. The superior jackpot is 8,000 money.
…
That is correct, you did read that right. You can now play online slots as well as other casino games anytime getting into right on your desktop. No longer do you have to wait until your vacation rolls around, or know some lame excuse to tell the boss so that you can get a week off to go over to the number one brick and mortar gambling house.
Some casinos, like those involved with the Caribbean islands, rely more on seasons to succeed. The Bahamas, Puerto Rico and others are completely booked from November to March. During this period even perfect players are comped less because casinos will be filed with paying people no challenege show up. In other words, require during now is so great a recession doesn’t matter again SLOT ONLINE .
So what is the slot machine tip that’ll make that you a GAME SLOT winner? Stop being greedy! Before you put your money at risk, think by what you plan to achieve, besides having excitement. Do you want to play for one number of hours, or do you wish to win an important dollar amount, or an assortment of both?
Then watch as LELE 189 show. The title screen will show the name of method and sometimes the developer. The game screen will a person what program it mes. You need to look at certain regarding that screen to see how SLOT CASINO to play that particular machine.Also, activity . will usually tell you the way high the Cherry and Bell Bonus go. However usually tell whether or the cherries go to 12, 9, 6 or 3, likewise whether the bells go 7, 3 or 9. The best ones to beat are the ones that cherry’s pay a visit to 3 and bells check out 2.These calls for less period for play and fewer money to defeat.
Fact: True, but not entirely. For about a game you simply require no skill or any strategy, the payouts are pretty decent. Imagine sitting within a blackjack table and looking over your luck with no strategy. You would end up in debt for are often the know.
At these casinos they’ll either allow you to enter a free mode, or give you bonus revolves. In the free mode they is able to offer some free casino credits, which don’t have any cash increased value. What this allows you to do is play in the various games that use the websites. Once you have played a online slot machine that you favor the most you tend to be comfortable making use of once you begin to play for funding.
If you are an avid player in casino. You should always keep abreast most developments help make the directly in favor in a company or slots. Therefore, we decide that positive if you enjoy the good news we in order to offer you. Who said that to win the jackpot, you should spend years? But it is able to be win it in a couple seconds, and now we simply n’t have any words, it is definitely very privileged.
…